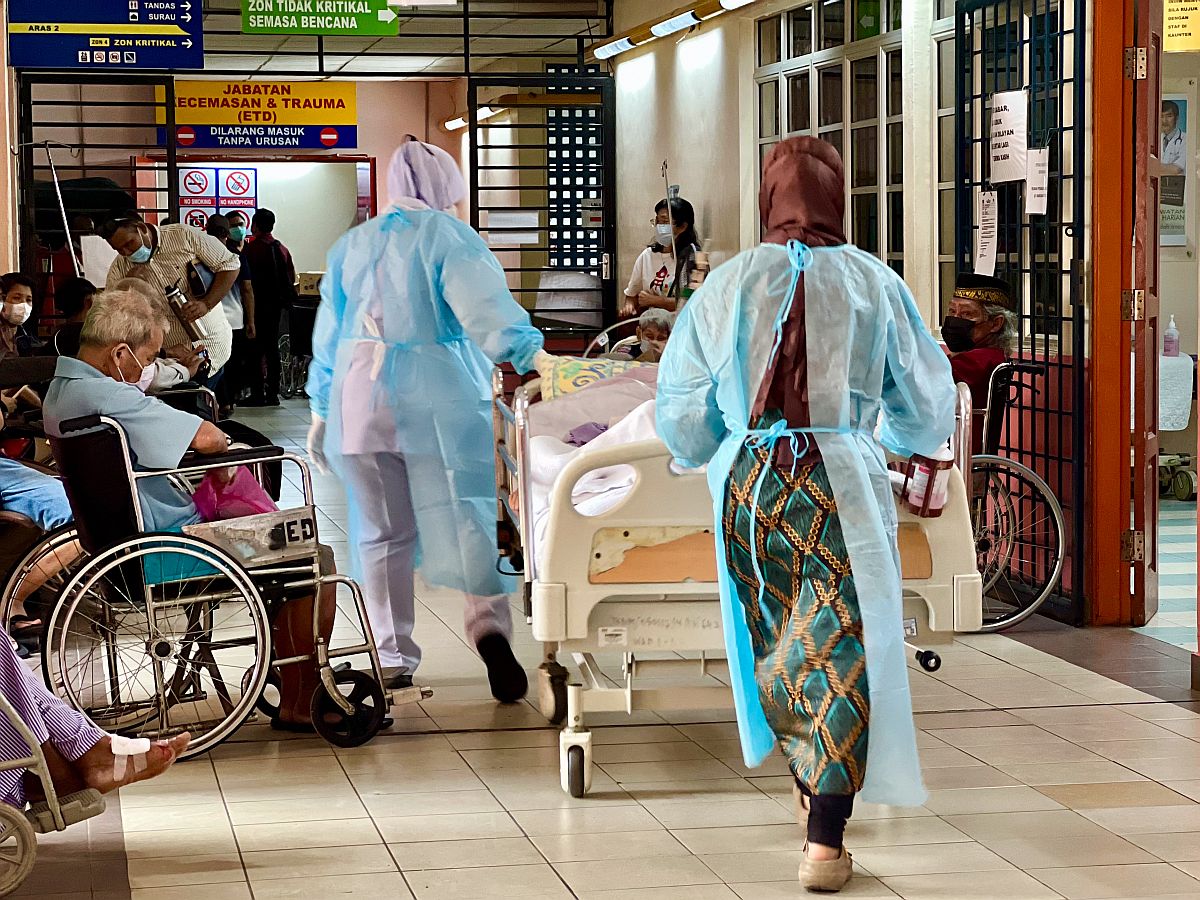
As Malaysia’s health care system grapples with rising costs, operational inefficiency, uneven insurance coverage, and public anxiety over medical bills, a provocative question has arisen: “Why not bypass incremental reforms and adopt a comprehensive National Health Insurance (NHI) system now?”, an interesting thought-provoking article on LinkedIn by Wong Teck Jin.
His idea that bold action trumps cautious steps carries moral appeal for many Malaysians facing rising medical inflation and a patchwork of insurance options outside the government health care system.
When analysing such a topic, one needs to dichotomise the providers and services given. Government data (2023 figures from the Ministry of Health’s Health Facts 2024) should bring clarity
- Inpatient Admissions indicate that ~ 66.9 per cent of hospital admissions occurred in public hospitals, with ~ 33.1 per cent in the private sector. As of November 2024, approximately 80 per cent of public hospitals were reported to be at full capacity.
- Outpatient attendance indicates that public hospitals accounted for approximately 83%, whereas private hospitals accounted for approximately 17 per cent.
- MOH’s budget rose steadily from RM36.1 billion (9.3 per cent of the national budget for 2023) to RM46.5 billion (11 per cent of the national budget for 2026), reflecting increased expenditure that warrants further assessment of how the budget was spent.
- The National Budget deficit shows a reduction trend from 5 per cent (2023) to an expected 3.5 per cent (2026) of the gross domestic product (GDP). However, certain government MPs have raised troubling questions on the possibility that the 2026 data is inaccurate.
These figures reflect overcrowded public hospitals, escalating operational expenses, and increasing fiscal pressure on the government from competing budgetary demands. Against this backdrop, this article examines and responds to Wong’s perspective.
What Does National Health Insurance Actually Mean?
Wong’s article goes beyond proposing a new insurance product under Bank Negara Malaysia (BNM). He advocates for a comprehensive, mandatory, and publicly funded national health insurance system that would centralise purchasing power, regulate health care prices, and ensure universal coverage.
Such a model could significantly transform Malaysia’s health care system and redefine the government’s role in public health.
However, this ambitious vision also raises important practical, economic, and political concerns. One key issue is that the concept of “insurance” reflects a commercial approach, whereas national health care financing should be structured on a not-for-profit basis.
Moreover, by shifting health care costs to the public without introducing new taxes, the scheme may effectively function as an indirect form of taxation.
Benefits Of Adopting The National Health Fund: Universal Coverage And Financial Protection
A national health fund has the potential to transform the country’s health care landscape by significantly expanding coverage and strengthening financial protection for all citizens.
By replacing the current voluntary, fragmented system with a mandatory universal risk pool, the scheme would help reduce out-of-pocket spending, protect individuals and families from catastrophic medical expenses, and provide much-needed health care services.
This is particularly important as rising private insurance premiums have made coverage increasingly unaffordable for many, forcing more people to rely on the already burdened public health care system.
Universal participation would ensure that access to essential health care services is not determined by income, employment status, or health conditions.
From a fiscal perspective, such a system would also benefit the government by creating a more sustainable funding base and enabling long-term investment in the modernisation of MOH hospitals.
Through national risk pooling, costs would be shared among healthy and sick individuals, young and old, creating a more equitable financing structure.
This approach would reduce the financial burden on individuals with chronic illnesses and limit adverse selection, where only high-risk individuals purchase insurance, leading to escalating premiums.
As a result, the system could promote long-term sustainability, improve access to care for the population, and enhance government finances.
Furthermore, consolidating multiple private insurance schemes into a single national system could reduce administrative duplication and operational inefficiencies.
Fragmented arrangements often involve overlapping management, billing, and claims processes, which increase costs without enhancing service quality. A unified structure may allow resources to be redirected toward patient care and system improvements.
Beyond financial and operational benefits, a national health fund could foster social solidarity and public confidence in the health care system.
By emphasising shared responsibility and collective protection, the scheme would reinforce the idea that health care is a social good rather than a privilege.
Experiences from other countries suggest that such systems can enhance social cohesion and provide long-term security, making universal health care a cornerstone of national well-being and development.
Challenges In Implementing A National Health Fund
While a National Health Fund (NHF) system offers important social benefits, its implementation presents several significant challenges that must be managed carefully.
Establishing and maintaining a nationwide health requires a substantial legal framework and administrative capacity. The government would need to develop robust systems for collecting contributions, managing claims, regulating prices, and monitoring performance.
These processes entail substantial upfront costs and ongoing expenditures, which may necessitate the reallocation of existing public funds.
Political and stakeholder resistance is likely to emerge. While private insurers may be willing to support reforms if they are assigned a meaningful role within the system, private health care providers and other industry players, including pharmaceutical and medical suppliers, may oppose such changes due to potential impacts on their commercial interests.
This resistance may intensify as the MOH network begins to offer more equitable services in terms of quality, accessibility, and speed.
At the same time, segments of the public may be concerned about increased financial obligations, particularly if the government fails to establish adequate mechanisms for financial support for those unable to contribute.
Such concerns could weaken public acceptance and complicate efforts to build a broad-based consensus. A balance must therefore be maintained between regulation and competition.
Finally, the transition process itself carries operational and political risks. Existing initiatives, such as the voluntary medical assurance scheme, serve as testing grounds for future reforms.
Bypassing these gradual steps may expose the system to implementation failures or temporary gaps in coverage. Careful planning and phased reform are therefore essential to ensure long-term sustainability and public confidence.
The Current Malaysian Context
Malaysia is currently exploring reforms to improve health care financing and expand access to medical coverage. One key initiative is the proposed base Medical and Health Insurance/Takaful (MHIT) plan, designed as a voluntary and more affordable option.
However, because participation remains optional, it is fundamentally similar to existing health assurance products sold in the market. While lower premium targets aim to widen coverage, important issues remain unresolved, particularly regarding the treatment of pre-existing conditions, medical screening, and the pricing of chronic illnesses.
Experts and consumer advocates caution that the effectiveness of these reforms will depend on whether policy commitments—especially those relating to coverage for individuals with existing medical conditions—are honoured in practice.
At the same time, civil society groups are calling for stronger regulation of hospital charges and for national social assurance, such as a National Health Fund (NHF), to be considered as part of a broader cost-control strategy.
Overall, current policy efforts reflect a preference for a gradual, evidence-based approach. This involves refining voluntary products, strengthening the regulation of private health care costs, and relying on pilot data before moving toward a comprehensive national system.
Conclusion
The question of whether Malaysia should move directly toward a National Health Insurance or National Health Fund system reflects broader concerns about affordability, equity, and long-term sustainability in the health care sector.
While we share Wong’s aspiration for comprehensive reform, we remain cautious about the legal, operational readiness, and practical execution of such a transition.
As discussed, rising medical costs, overcrowded public hospitals, and fragmented financing arrangements continue to place significant pressure on both households and public finances.
A unified national system offers considerable potential benefits, including stronger financial protection, improved service, reduced operational cost, broader coverage, greater efficiency, and stronger social solidarity.
Nevertheless, these reforms must be approached with careful planning and strong institutional support. Fiscal limitations, administrative capacity, stakeholder resistance, and public acceptance remain substantial challenges.
Without sound governance, transparent pricing mechanisms, and effective safeguards for vulnerable groups, a national scheme risks weakening public confidence and creating new inefficiencies.
International experience shows that successful universal systems are typically built through gradual implementation, supported by reliable data, stable funding, and broad political consensus.
Although Malaysia’s current emphasis on voluntary products and regulatory improvements suggests a cautious, evidence-based approach, there is limited public indication of a clear roadmap toward comprehensive national health financing.
Ultimately, while bold reforms are attractive, lasting progress depends on institutional readiness, policy coherence, and public trust. A carefully sequenced and transparent reform strategy is essential to ensure that universal health care remains financially sustainable and socially equitable for future generations.
Dr Mohamed Rafick Khan is a trained physician with 12 years of experience in military medical services and over 22 years of experience in the assurance industry. He retired as the CEO of a multinational reinsurance company in 2019 and remains active as an independent international assurance industry consultant.
- This is the personal opinion of the writer or publication and does not necessarily represent the views of CodeBlue.