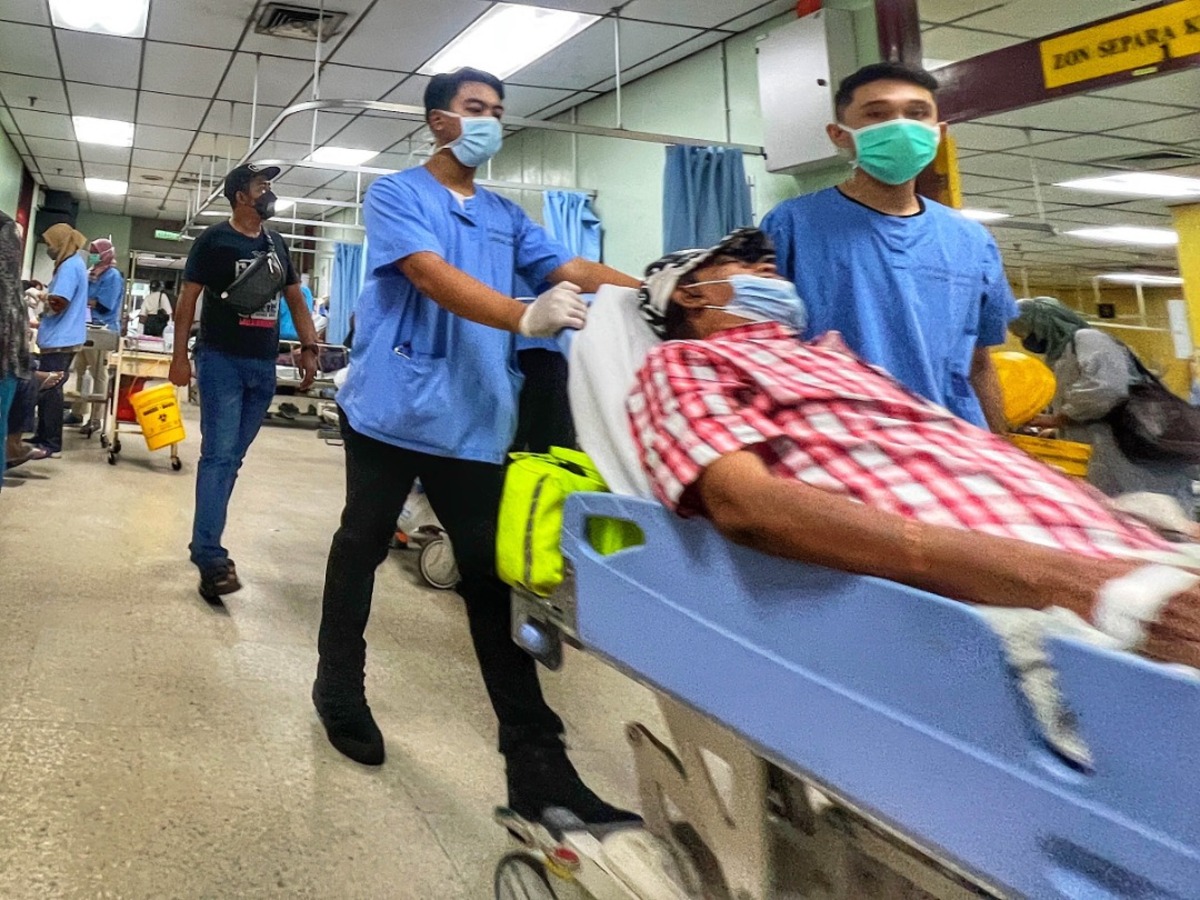
Recently, there was a discussion about patients waiting for 15 hours to get care at a hospital in Selangor. It started from the Emergency Department (ED).
This article will cause some discomfort to readers, but administrators may see it as “saying it point blank.” This is a two-part article. Part One just states the facts on pain points. Part Two states the facts for improvement.
Let’s talk about the pain points.
Pain Point 1: Triage is always done by Assistant Medical Officers and without proper supervision.
Triage is unique because it has no exact science – it works by experience, especially when patients do not present in distress.
The Assistant Medical Officer (AMO) profession is failing to achieve any standards of care. ED has always been said to be the domain for AMO, but they are failing to excel in this domain despite having written guidelines on standard of practice in Emergency Care and Triage.
When one walks in the ED, try to look for an AMO Supervisor doing clinical tasks of seeing patients or even being in the triage area for a full shift. The answer is “no.” Triage CCTV will attest to this. A profession whose clinical standards are unsupervised on a daily basis will never reach service excellence.
Previously, the supervisors were known as “baju hijau“, but with the current uniform for AMO now, we can’t really differentiate the Supervisor from the rest.
One of the peculiarities of Ministry of Health (MOH) hospitals is that AMO Supervisors are always in charge of store, inventory, and non-stop meetings. Store and inventory management is a non-clinical task. Procurement requires clinical knowledge, but inventory management is not one.
Pain Point 2: Despite having many Emergency Physicians, especially in large centres, the ED is still managed by Medical Officers.
One of the greatest things about Emergency Medicine is that it is creative in expanding and creating new areas – toxicology, trauma care, emergency critical care, prehospital care, and disaster medicine.
This has led to a new phenomenon where Emergency Physicians (EP) who have done these Areas of Interest are not doing so-called General Emergency Clinical Care anymore. They are too highly trained to be working in the “pit.”
Distributions of EPs who have completed Area of Interests advanced training also lack strategic vision. We have hospitals with more than many Disaster Emergency Physicians, Emergency Trauma Physicians, and Emergency Critical Care Physicians. There is also now a new sub-specialised service in the ED, which is meeting management for the Head of Service.
New areas of care and Areas of Interest have all led to the perception of insufficient Emergency Physicians in tertiary centres. In the end, within the ED, the first contact for patients continues to be the Medical Officer (MO). Most of the time, the MO decides the care of the patient and not the Emergency Physician.
From the health care system perspective, ALL patients need to be seen by an EP because the traditional hospital-based system of MO-then Specialist consultation has caused bottle-necking. EPs in Yellow and Red Zone need to apply advanced triaging techniques to identify patients requiring inpatient services.
It is imperative that EPs practice “the right patient to the right disposition in the shortest period of time using the right supportive resources.”
Pain Point 3: No matter what zone you are in the ED, your first contact point to Specialty is the junior Medical Officer or even House Officer.
This is a vicious cycle. Because the ED is managed by the MO and not EPs in clinical zones, referrals to specialty may be regarded as “not properly assessed” by other Specialties.
Specialties will send the junior Medical Officer to attend to the patient first. Then it is a step-ladder hierarchical system climb for the patient – HO to junior MO to senior MO to Registrar and, if lucky, to Specialist. Each ladder will add an investigation, causing infinite hours of waiting sometimes.
All of this is because the ED system is broken – triage is unsupervised and the EP does not see patients. Specialties feel that they need to really work up the patients in ED to prevent unnecessary admission.
Pain Point 4: The ED Observation Ward or Yellow Zone is “treated like a ward”, but with different standards of care.
This point is easy to sum:
- No nursing to patient ratio.
- No nursing ratio means you can continue to push patients in – “selagi boleh nampak lantai, boleh masuk lagi.”
- If you cannot see the floor, please proceed to corridor medicine.
- After staying for more than four hours, you may get discharged but no discharge summary.
Discharge summary is an important document for patients to have, especially for those who have been seen by other Specialties in the ED. It will direct the next doctor to the care that has been given by the Specialty and future care planned for the patient.
Pain Point 5: The Green Zone is the worst zone to be in.
There are many false beliefs that the Green Zone is Outpatient Service. This false belief has led to many interventions, such as wrong patients diverted to Klinik Kesihatan.
The best summation is what the green zone is:
- If all other zones are full, and the triageur feels that you’re not sick enough, then go to the Green Zone.
- If a specialist clinic refuses to see you despite having a proper referral letter, then go to the Green Zone.
- If Klinik Kesihatan or a General Practitioner does not know what is wrong with you, then go to the Green Zone.
- If a patient refuses to go to a Klinik Kesihatan or General Practitioner, then go to the Green Zone.
- if you are hospital staff who needs an MC, then go to the Green Zone.
The Green Zone is the most dangerous zone to be in for any patient. It has no limit to the number of registered patients; the numbering system is mysterious as to when a patient will be called; and there are incidents of patients silently stopping breathing while waiting to be seen.
Summary
What is said about the pain points is not a trade secret. Many health ministers have tried to change it, but it was never sustainable. It actually boils down to culture and the existing hospital system that refuses to change even though it is broken.
We cannot be doing the same thing again and again, expecting different results.
The author is an emergency physician at a government hospital in the Klang Valley. CodeBlue is providing the author anonymity because civil servants are prohibited from writing to the press.
- This is the personal opinion of the writer or publication and does not necessarily represent the views of CodeBlue.