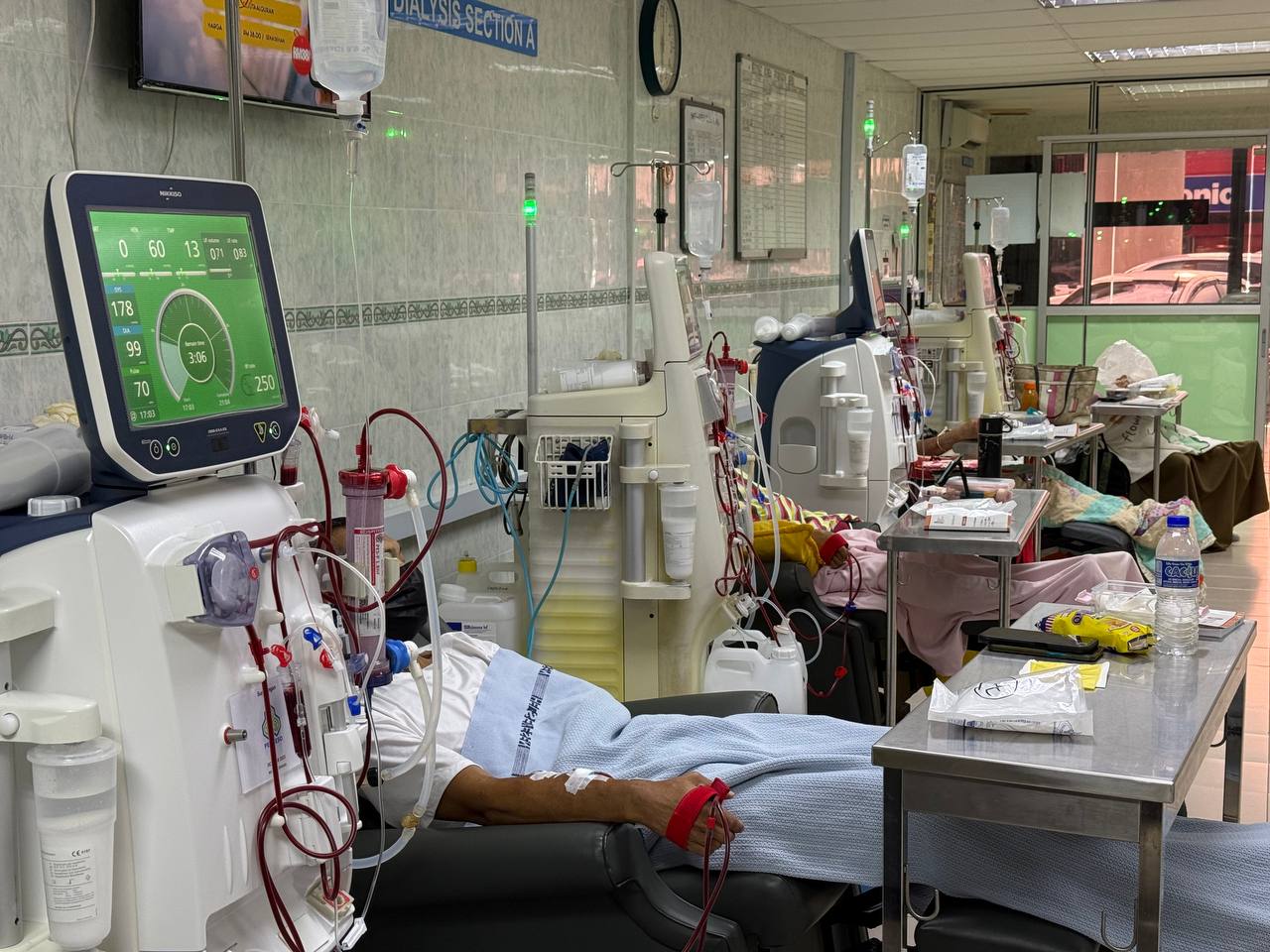
KUALA LUMPUR, April 17 — National Kidney Foundation (NKF) Malaysia has suggested decreasing the frequency of dialysis treatment if shortages of plastic-based medical devices and consumables worsen.
NKF chairman Dr Zaki Morad Mohd Zaher was frank in his assessment of potential long-term shortages of critical dialysis product components due to the West Asia conflict, even though he noted that dialysers and other consumables aren’t currently in short supply at NKF.
“All forms of kidney replacement therapy (KRT) will be affected if supply chains for consumables and even medications are affected. Switching from one form of KRT to another will not solve the problem,” Dr Zaki told CodeBlue when contacted.
CodeBlue recently reported on shortages of dialysers and canister or bottle packaging for haemodialysis (HD) concentrate solutions that are emerging at the distributor or supplier level. A supplier said it has stopped accepting new customers for concentrate orders.
Dialyers or artificial kidneys, a core component of HD therapy, aren’t required for peritoneal dialysis (PD), although the home-based treatment still relies heavily on plastic-based consumables.
“A potential measure that may be used if the situation becomes more acute is to consider reducing frequency of treatment,” said Dr Zaki, who is also a consultant nephrologist.
“In HD, centres will have to identify patients who are fit enough to take two sessions a week instead of three for a short period, thus reducing use of consumables. In CAPD (continuous ambulatory peritoneal dialysis), exchanges can be reduced to three a day instead of four; likewise with APD (automated peritoneal dialysis).”

NKF currently provides treatment to nearly 1,800 patients across its 32 HD centres nationwide. The major dialysis charity has been practising single-use dialysers in all its centres for the past few years.
“We do not stockpile dialysers or other consumables beyond two weeks’ usage as store space in our HD centres (and this is true for all HD centres) is very limited and these items are fast-moving,” said Dr Zaki.
“We are closely monitoring the situation. Moving to reuse dialysers can be an option, but there are other items such as blood lines and needles that are no longer reused in present-day practices.
“Furthermore, to reuse dialysers we need reprocessing machines. Centres that do not reuse would have disposed of their reprocessing machines, complicating return to reuse of dialysers.”
Another option, said Dr Zaki, is to optimise the strength of dialysate concentrate in the containers that, upon dilution, can be used for more than one dialysis session.
The nephrologist also suggested delaying the start of HD or PD for new patients with end-stage kidney disease (ESKD), with prolonged conservative treatment and close monitoring of affected patients instead. Conducting preemptive live kidney donor transplants will also bypass the need for dialysis, besides increasing kidney transplants from deceased donors.
More than 10,000 patients are on Malaysia’s waiting list for kidney transplants. Pending kidney transplantation, dialysis is necessary for the survival of people with kidney failure, as they can die within a few days without the treatment.
Maaedicare Plans To Increase Buffer Stock, Identify Backup Suppliers

Maaedicare Charitable Foundation said it’s not experiencing any significant delays in the supply of dialysers or other haemodialysis components at the moment.
The nonprofit, which provides dialysis and cardiac treatment, currently provides HD treatment to more than 770 patients across its 11 dialysis centres in the Klang Valley, Johor, Perak, Pahang, Kelantan, Penang, Sabah, and Sarawak.
“Supply chains remain stable, and all centres are currently able to treat patients as scheduled without disruption,” Maaedicare head of operations Dr Parathythasan Rajaandra told CodeBlue.
“Maaedicare’s buffer stock of dialysers and other haemodialysis consumables is currently planned to last for approximately one month, depending on patient load and centre‑specific usage patterns. This buffer is designed to help maintain uninterrupted treatment during any short‑term supply disruptions.”
Dr Parathythasan added that Maaedicare dialysis centres follow a strict single‑use policy for dialysers, in line with international best practices and infection‑control standards. “This approach prioritises patient safety and reduces the risk of cross‑contamination.”
The dialysis charity’s priority is to increase its buffer stock, as well as identify alternative vendors and potential backup suppliers.
“This strategy aims to maintain uninterrupted care without resorting to triaging based on availability of dialysers or other HD components,” said Dr Parathythasan.
“Maaedicare currently has no plans to stop admitting new patients into its haemodialysis programme. The Foundation remains committed to providing access to life‑sustaining dialysis for all eligible patients.”
Socso Backed By Satellite Dialysis Stock Arrangement

The Social Security Organisation (Socso) said it has yet to identify any “sustained” supply issue that has affected patient treatment in its own dialysis facilities.
The statutory body, which is both a provider and payer of dialysis treatment, operates six Perkeso dialysis centres in the Klang Valley, Penang, and Johor, catering to approximately 400 HD patients.
“We continue to monitor stock levels closely, supported by buffer stock at centre level and ongoing coordination with suppliers, so that any emerging issue can be addressed early before it impacts services,” Socso told CodeBlue in a statement.
“Dialysis consumables are fast-moving clinical items, but centres do not operate on a purely just-in-time basis. In practice, centres maintain a reasonable level of buffer stock based on usage patterns. This is further supported by a satellite stock arrangement, which allows supplies to be redistributed between centres when required.”
Socso said it continues to monitor stock levels of dialysis products and coordinate with suppliers, “including redistribution where necessary”.
Like Maaedicare, Socso appeared to be disinclined toward switching back to reuse of dialysers in a shortage, saying Perkeso dialysis centres are progressively moving towards a single-use dialyser approach as part of ongoing quality and safety standardisation.
“Any clinical practice is guided by patient safety requirements and applicable clinical standards. At this point, there is no change to the current direction, and any supply pressure is managed through operational measures rather than changes to clinical standards.”
Socso – which pays for dialysis treatment at over 700 private dialysis centres nationwide under its panel – also said it would need to consider any financial requests carefully, when asked if it would consider increasing allocations for particular panel dialysis centres to obtain HD supplies early at a premium in a shortage.
“Perkeso does not adjust payments on an ad hoc basis in response to short-term market changes, but will continue to monitor developments and engage with relevant stakeholders where necessary to support service continuity.”
Over Half Of ESKD Patients Treated In Private Dialysis Centres

CodeBlue understands that some dialysis centres are already advising their clients that a shortage can happen at any time and with very little warning, and that patients should seek advice from their doctor about potential treatment modification.
In Malaysia, which has a very high kidney failure burden with an estimated 60,000 dialysis patients, private centres remain the largest provider of dialysis.
“Among new patients, 62 per cent were accepted to private dialysis centres, followed by government centres (26 per cent) and NGO [non-governmental organisation] centres (12 per cent). The proportion of patients dialysing in the private sector has been steadily increasing over the last 30 years, accounting for more than half of prevalent patients since 2018,” said the Malaysian Dialysis and Transplant Registry 2024.
According to the report, 56.5 per cent of 55,237 ESKD patients received dialysis in private centres at the end of 2024, followed by public centres (28.1 per cent) and NGO centres (15.5 per cent).
In 2024, private centres comprised about 70 per cent of 1,047 HD centres in Malaysia at 700, followed by public (179) and NGO (168).

This means that a shortage of dialysis products is likely to hit small private centres first before bigger service providers or government (Ministry of Health) facilities, with the latter managing less than 30 per cent of the country’s dialysis patients.
While Maaedicare and Socso only addressed potential “short-term” shortages of dialysis medical devices and consumables, the plastics industry’s concerns about prolonged disruptions of supply of petrochemical derivatives support NKF’s preparations for treatment rationing and delays.
The Edge weekly reported this week plastics makers as saying that the supply disruption from the Iran war is more severe than the Covid-19 pandemic.
“During the pandemic, factories were generally allowed to continue production and the underlying supply of raw resin remained relatively stable. The primary issue was logistical,” Malaysian Plastics Manufacturers Association president C C Cheah told The Edge.
“Today, the scenario is driven by a severe upstream crisis. Asia, along with the broader global market, is facing critical shortages of fundamental feedstock, being crude oil and natural gas. Without these raw materials, refineries are unable to produce the essential grades of aromatics and chemical precursors required by the entire industry.
“Even if the conflict ends in the near term, a true normal will not be immediate. We must first assess the actual physical condition of the region’s oil refineries, petrochemical plants, and supporting infrastructure to accurately gauge future supply capabilities. It may take many months or several years to normalise.”
MOH Must Form Nephrology Task Force, Activate Central Command Structure

Dr Rosnawati Yahya, a consultant nephrologist and kidney transplant physician at Sunway Medical Centre, urged the Ministry of Health (MOH) to form a nephrology task force to face emerging shortages of dialysers and HD components as a national problem, rather than piecemeal responses to individual facilities.
She pointed out that even though large hospitals have more established procurement pathways than smaller service providers, a global supply chain disruption affects the entire ecosystem.
“To mitigate this, we must prioritise central coordination over a fragmented response. Activating a central command structure at the MOH or network level and establishing a real-time stock visibility dashboard is essential to ensure equitable resource allocation and controlled distribution across all facilities, regardless of size,” Dr Rosnawati told CodeBlue.
The former head of the National Kidney Transplant Centre (renamed as the National Transplant Centre) recommended the following immediate actions for dialysis centres:
- Conduct urgent stock audits: Establish facility-level visibility and maintain a minimum stock buffer (for example, four to eight weeks).
- Rationalise use: Avoid unnecessary consumption and consider temporary, clinically supervised adjustments to dialysis frequency or duration for selected stable patients.
- Resource sharing: Establish regional pooling of supplies and inter-centre transfer protocols.
- Alternative sourcing: Activate emergency procurement pathways and identify parallel suppliers.
As for medium-term planning, Dr Rosnawati suggested diversification of supply chains to avoid single-source dependency, besides exploring local manufacturing or national strategic stockpiles.
Dialysis centres should increase PD uptake by quickly starting peritoneal dialysis programmes for suitable patients and establish clinical prioritisation frameworks based on clinical stability, for example Tier 1 for life-threatening cases versus Tier 3 for stable patients eligible for reduced treatment intensity.
“Provide clear explanations of temporary measures to patients and staff to prevent panic and ensure equity,” added Dr Rosnawati.
On switching from single-use to reuse of dialysers, the nephrologist stressed that any alternative products or changes in practice must strictly adhere to AAMI/ISO standards.
“Patient safety and sterility are non-negotiable. While the primary goal is maintaining the continuity of dialysis, any shift in practice would need to be clinically supervised and documented without compromising quality standards,” said Dr Rosnawati.
The MOH told CodeBlue recently that it wouldn’t reuse dialysers in its facilities beyond 12 times, even if prerequisite conditions of above 80 per cent total bundle volume (TBV) during reprocessing are met.
The ministry touted building buffer stock for the short term, without addressing potential long-term shortages of critical dialysis consumables.