KUALA LUMPUR, Dec 19 — Overcrowding has transformed the emergency department in public hospitals – at the patient’s detriment – from resuscitating and stabilising very sick people into a makeshift ward, dialysis centre, and even intensive care unit (ICU).
Emergency doctors from two public hospitals in Kuala Lumpur explained that things that would usually be done in a ward – such as investigations, planning, and management by other teams like the medical or surgical teams – are now done in the emergency and trauma department (known as ETD or ED), as patients are stranded in the ED for days due to full wards.
Dr John (pseudonym) – an emergency medical officer working at Hospital Canselor Tuanku Muhriz UKM (HCTM), a university hospital in the capital city – said that when all the beds and wards are full, the hospital’s primary team treats patients in the ED.
If the patient is stable enough that only outpatient monitoring is required, then the patient will be discharged from the emergency department and sent home.
“When the wards are full house, patients would often be left stranded in either our observation area, or worse, our Yellow Zone (Semi-Critical Zone) for one to two days (rarely three days) and the intubated patients, which often would require intensive care, can be stranded for up to five days, based on my observation, due to scarcity of the intensive care bed,” Dr John told CodeBlue recently.
“When the primary team, i.e. medical team, feel that they are stable enough for discharge and only outpatient monitoring is required, they would usually be discharged by them (doctors) from our ED.
“Mind you, preceding such a decision, there would be a whole lot of investigations that would have to be done (often which is what needed to be done in ward but is now done in ED).
“The problem is that when this happens, all the active plans that need to be carried out – including the request, referrals, discharge plan etc – would have to be done by the ED team, since these patients are stranded in ED. This has contributed to even more work for the ED team when ED is already a war zone.”
Dr John spoke on condition of anonymity as civil servants are prohibited from speaking to the press.
The accounts by emergency doctors in Kuala Lumpur on patients who are stranded for days in the ED of their hospitals indicate that such long waits for ward admission are not an isolated phenomenon specific to Raja Permaisuri Bainun Hospital (HRPB), the general hospital in Ipoh, Perak, but likely occurring across the country in busy public hospitals.
CodeBlue reported last Monday that critically ill patients, including ventilated cases, are stranded for up to six days in the Red Zone of HRPB’s emergency room due to insufficient critical care beds and staff. Doctors from the Ministry of Health (MOH) hospital said the situation this year has worsened from pre-pandemic days, when patients waited one and a half days at the most back then for beds in a ward.
Unfair To Ask ED Staff To Perform Work Beyond Their Expertise
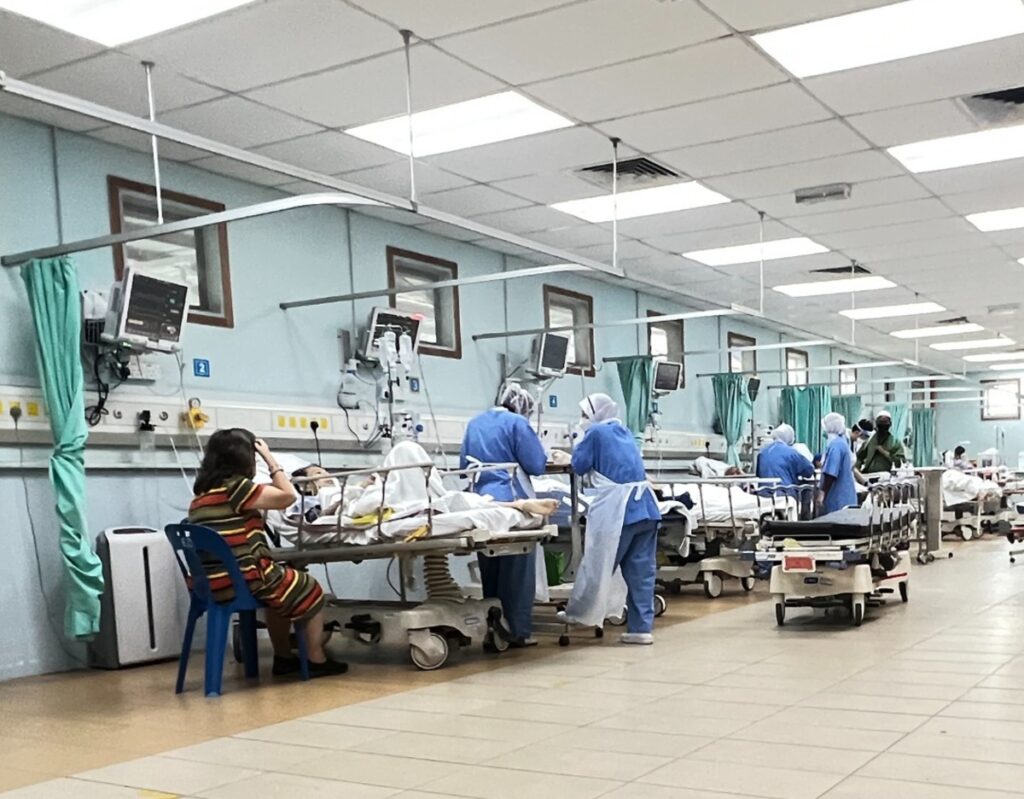
Death following long waits in the ED is something that has occurred in HCTM, Dr John said.
“Yes, there are patients who have passed on in our ED after being stranded for many days, but whether or not this is because of less than ideal care that is needed by them is questionable.”
Explaining the context for his answer, Dr John stated that ED staff do not specialise in critical care, and thus, it is unfair to ask them to perform a job that is beyond their area of expertise. And unlike regular patients, critical patients require constant observation and intervention by a trained critical care staff nurse or medical assistant.
“Neither ED doctors nor ED nurses are particularly trained in some aspect that the primary team would expect us to cover,” he pointed out.
“Let me give an example. If a medical team is investigating an autoimmune connective tissue disease that comes in [with a] flaring episode, they would need to send a whole lot of investigations.
“Often, these investigations are not available to be done at ED (simply because we don’t have the expertise and tools for it). Furthermore, some of these investigations can only be done on a certain day of the week because it will need to be sent to an outside lab or even overseas lab. When the patient is stranded for a day or two at ED, they would lose the precious time to come to an exact diagnosis. Hence, this is what suboptimal care is about.”
Though the ED serves as a stabilisation and resuscitation unit where patients in critical condition are rushed in, stabilised, and rushed out to be immediately admitted into their respective inpatient wards, the transitory nature of the emergency room has inevitably changed with the rising tide of patients and the lack of beds.
“In all fairness, I feel that the ED role has gotten more versatile over the years. Due to the number of backlog patients in ED, often active plans from multiple other teams, such as medical, surgical etc., would have to be done mainly by the ED team simply because the patient is stranded in ED,” Dr John said.
“The reason is because the primary team often consists of only one or two MOs (medical officers) on duty, and in the case of the medical team, they would have to see like up to 50 patients under them at ED (and many, many more who keep coming in and referred to them).”
HCTM Turns New Non-Critical Patients Away (Except Paediatric Cases) When Wards, ED Hit Maximum Capacity

HCTM, a university hospital, forms the public wing of the Universiti Kebangsaan Malaysia Medical Centre. According to Dr John, its day-to-day running comes under the Ministry of Higher Education (MOHE), while health professionals there work under MOH.
Due to it being a university hospital, patients seeking treatment need to put down a deposit that ranges from RM100 for a four-hour observation admission to RM5,000 for admission into the intensive care unit (ICU), coronary care unit (CCU), and so on.
Based on Dr John’s description, HCTM has six general medical wards. Each ward has two to four isolation rooms and can accommodate 28 patients. Of these 28 beds, four to six beds are reserved for acute care patients while the rest are for patients requiring sub-acute care.
Though the average length of stay for patients is about five to seven days, Dr John said, there are patients who have stayed for up to 14 days. Because there is “no such thing as an extra extension bed that can be set up (unlike MOH)” — as the patients are full-paying patients — patients will have to be managed in the ED once wards are full, contributing to the backlog.
“Usually, this would happen towards the end of, I would say, three to four weeks’ cycle when the wards are full, and our ED would have to triage away new patients,” Dr John said.
“What this means is that when our wards and ED are both at almost maximum capacity, we would need to turn away new patients who are not super critical, and we would have to turn away patients (without immediate life-threatening issue) who arrived by private ambulance, to the nearest public hospital.
“We would only accept new patients who come in with an immediate life-threatening event, and thus, arrive by our own ambulance. This is of course with an exception to paediatric patients – we can never triage them away by law no matter how sardine-packed our ED is, even if we have to put them in the corridor.”
HCTM’s emergency department is divided into four zones: Observation Zone, Green Zone (non-critical), Yellow Zone (high risk), and Red Zone — a critical zone which requires patients to be seen immediately.
Described as a “very dynamic area” by Dr John, the Red Zone of HCTM holds about six beds, but is only allowed to hold five patients at any given time as one bed needs to be kept vacant for immediate resuscitation.
“This zone usually would be fully occupied. So far, I have seen patients being stranded in Red Zone for about one to two days at most before we had to down triage them to Yellow Zone, even if they are ventilated and sedated, because we need the resus bed for new immediately critical patients.”
Don’t Allow ‘Hospital Shopping’, Follow Australian System Of Assigned Hospitals
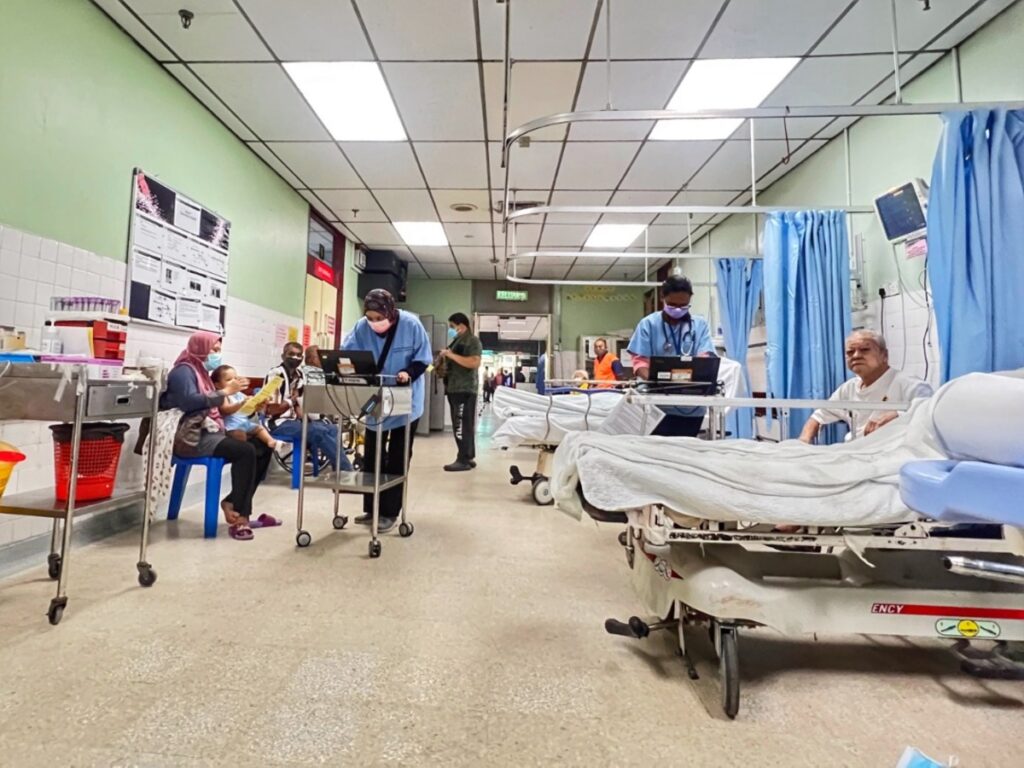
To better address these systemic problems, Dr John proposed two areas that the government ought to look into: the overall system and issues at the hospital level.
When it comes to the system, Dr John held that the “concept of the ED visit needs to be revamped” with a system akin to that employed in Australia.
The Australian system, according to Dr John, assigns patients a public hospital, preventing them from choosing their hospitals. By adopting such a system, Dr John seeks to make the system fairer for patients living in the area the hospital is located and fairer for the hospital itself.
“Famous hospitals like HCTM would receive non-emergency cases via our ED even from as far as Perlis and Langkawi, due to patients’ preference, which is unfair to the local community. Not to mention the strain on our limited resources when this happens,” he said.
“Unless there is a real emergency and the patient is reasonably near to our hospital, I don’t see why they should be allowed to go hospital shopping. Mind you, we are always receiving patients who went to other government hospitals first, got discharged by ED there, and they came to our hospital’s ED for a second opinion. This is just so inefficient.
“Spoiler, HPKK (UKM Specialist Children’s Hospital) next door to HCTM is experiencing a major manpower issue. Staff are being shared between our two hospitals when HCTM is already by itself experiencing manpower issues. AND ON WEEKEND AND AFTER 5PM ON WEEKDAY, HPKK ED is closed, and they are dependent on HCTM ED for admission to their hospital. What a joke, right?” he wrote to CodeBlue.
When it comes to the hospital level, Dr John cited three issues that need to be dealt with— staffing, the physical size of the hospital, and the lack of new hospitals.
Having sufficient manpower to ensure hospitals run smoothly is one of the most pressing issues of the Malaysian health care system, and in university hospitals, this issue of staffing becomes a more serious matter during examination season.
“In between exam seasons, MOs would also be assigned to other MOH hospitals as attachment MOs as part of the master’s programme training. Not to mention, the dwindling number of HOs (house officers) coming into our hospital has led to even bigger strain on the ED team. Thus, when this happened, the care of patients would be suboptimal, with exhausted doctors and nurses on duty.”
The second issue — size — is directly related to the lack of hospitals. According to Dr John, it is a “common fact” that public hospitals in the Klang Valley are functioning at full capacity. Yet, many major cities such as Subang Jaya and Petaling Jaya do not have their own public hospitals, “save for UM”.
“Why are dense areas like Cheras dependent only on HCTM and HKL (Kuala Lumpur Hospital) for tertiary care? Frankly speaking, whenever our hospital is full house, we would triage them all away to HKL. And this is true for many other hospitals around HKL too,” Dr John said.
“What would happen to HKL then? To solve this problem, it is crystal clear that the government needs to build more hospitals in those highly dense areas and employ more manpower.”
Not Much Improvement Since AG’s 2018 Report On Overcrowded Emergency Departments
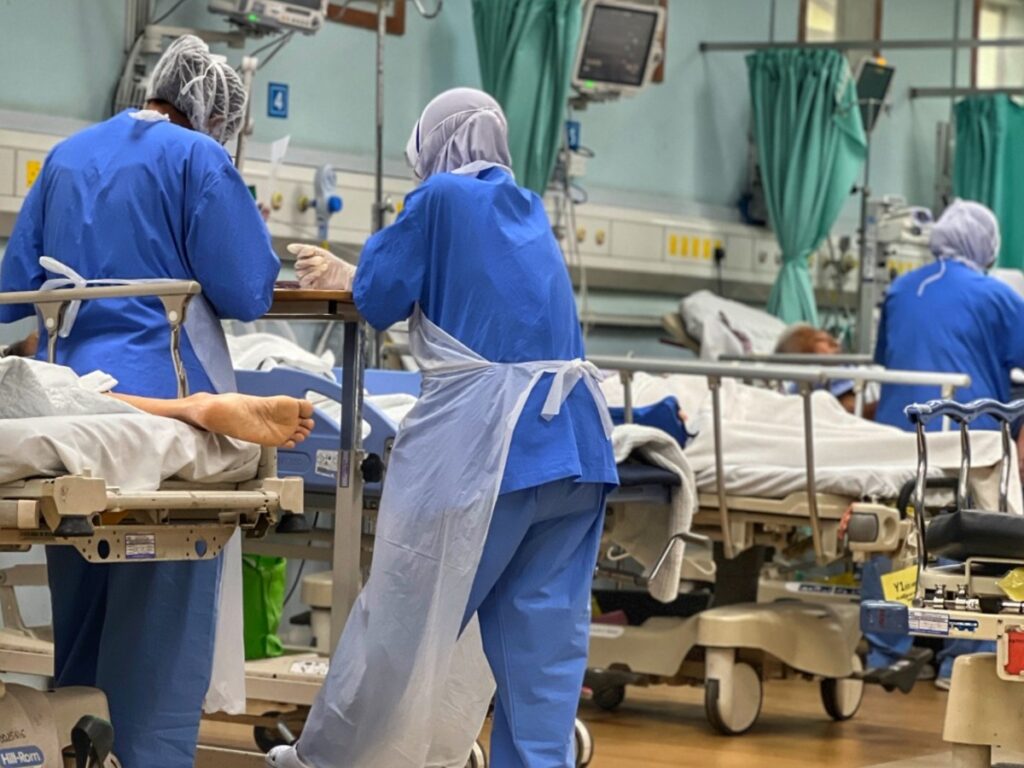
In an interview with CodeBlue, Dr Rizal (pseudonym), an emergency medicine doctor from a government hospital in Kuala Lumpur, attributed the congestion in public hospitals to an insufficient number of hospitals to meet the needs of a growing population.
“The emergency departments in Malaysia are congested due to:
- Increased number of patients in line with population growth;
- The expansion or increase of the number of hospitals does not go in line with population growth;
- Staff numbers are not increased to commensurate the work burden; [and]
- Hospital beds are full almost all the time and patients at emergency departments could not be pushed into wards — clogging the department. This despite all treatments started and given while they are in the emergency department.”
Citing the four-year-old 2018 Auditor General’s (AG) report, which details some of the problems mentioned above, Dr Rizal held that the issue of overcrowded EDs is not the fault of the emergency room. Rather, the congestion is a symptom of a larger problem; and the ED is nothing more than a “victim” of full wards.
Regrettably, Dr Rizal said, since the publication of the AG’s 2018 report in July 2019, “there has not been much improvement”.
The AG’s report concluded that emergency and trauma department services were inefficient due to rising patient arrivals, insufficient facilities, and an increase in the work burden of ETD staff. Emergency units, said the audit, were underfunded, understaffed, and overcrowded.
The national audit – which investigated four public hospitals in Selangor: Tengku Ampuan Rahimah Klang Hospital (HTAR), Selayang Hospital, Serdang Hospital, and Kajang Hospital – found that patient arrivals exceeded the standard Level of Care by between 5.7 per cent and a whopping 95.6 per cent.
Only 58.7 per cent to 74.5 per cent of patients were treated in less than four to six hours. The national audit also found 917 cases of “access block”, where patients could not be moved to medical wards. Audited hospitals failed to achieve their Medical Emergency Coordinating Centre’s (MECC) key performance indicator for Priority 1 cases (critical cases).
The AG’s 2018 report also found that based on the Workload Indicators of Staffing Need (WISN) 2010, there was an overall deficit of ETD job positions that ranged from 11.6 to 53.1 per cent, compared to the positions needed. The biggest staff shortages were emergency specialists (75.6 per cent to 79.5 per cent), medical officers (41.2 per cent to 64.6 per cent), assistant medical officers (2.6 per cent to 33.9 per cent), and trained nurses (17.4 per cent to 67.1 per cent).
“Despite all these, staff still gave all they can, but full hospital beds that require hospital beds’ expansion is beyond them. Solution is to open new wards with staff to run them,” Dr Rizal said.
“Twenty years ago, six new hospitals were built in Klang Valley alone in anticipation of an increased number of patients. Now, not many new hospitals. MOH staff are taken on contract basis. Number of posts not increased.
“Even with new hospitals built, staff are ‘taken away’ from existing hospitals or clinics (example Hospital Tunku Azizah, Hospital Cyberjaya, Hospital Tanjung Karang… etc),” Dr Rizal wrote to CodeBlue.
Dr Rizal, however, held that it is important for people to understand that although they are waiting in the ED, it does not mean that they are not receiving treatment.
“The perspective should be correct: Being stranded in ED does not mean no treatments. It’s given, but devoid of the comfort of proper beds in ward. And ED, with all of them still there, has to continuously see new cases,” he said.
“As at this rate, the number of patients will further overwhelm the already overwhelmed EDs.”
CodeBlue’s report on days’ long stranding of patients in HRPB’s emergency department cited medical officers as saying that most of the critically ill patients coming into the ED are presenting with advanced non-communicable diseases (NCDs) — such as heart disease, kidney failure, and stroke — following the disruption of care during two years of Covid lockdowns.
ED Now Functions As Makeshift Ward, ICU, Dialysis Centre
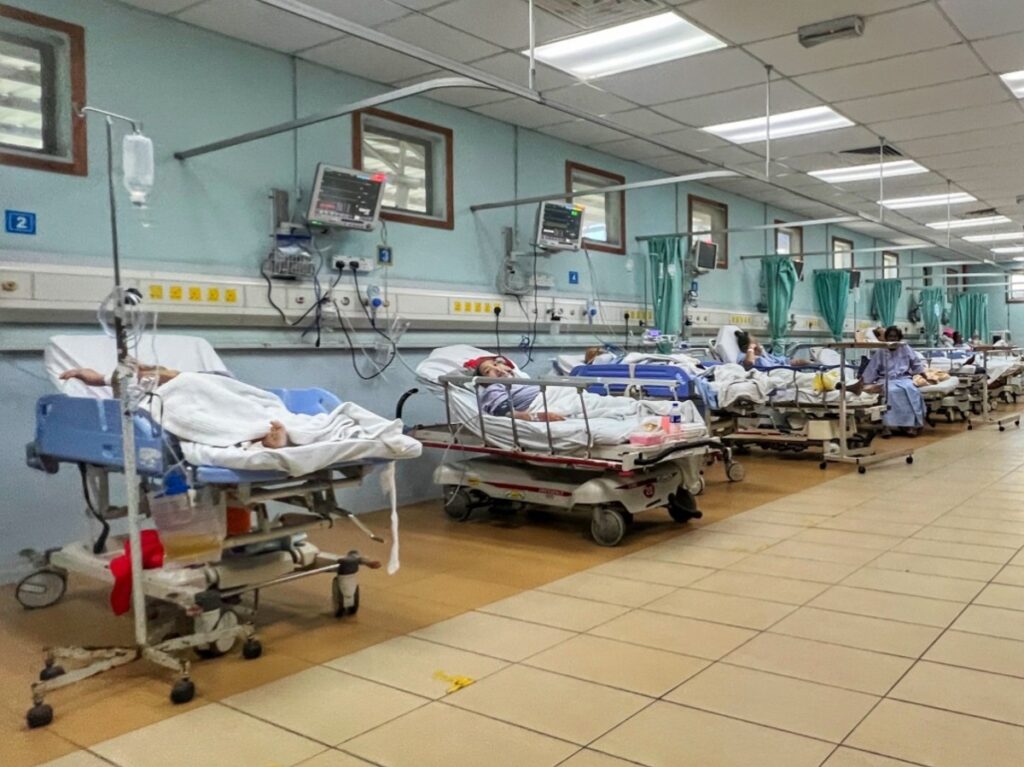
With the ED adopting a dual role as both a stabilisation and treatment unit, Dr Rizal held that doctors and staff in the emergency room now determine the stability of patients; resuscitate patients; and initiate all required treatment from the beginning.
This continues as long as patients are in the emergency department – take referrals and provide treatment; perform dialysis; and if the patient is still in the ED, then doctors even remove tubes, reduce medication, and discharge them from the emergency room.
“In a way, we (ED) function as ward, ICU, and dialysis centre – despite our focus is to resuscitate, stabilise, initiate treatment plans – and admit them to ward (20 per cent of patients we see in ED admitted, whilst 80 per cent others discharged),” Dr Rizal said.
While this tremendous movement is going on in hospitals to save patients’ lives, the question on whether such a situation is ideal and whether the patient receives appropriate care still remains.
To that, Dr Rizal wrote: “No (the ones meant for admission). The crowd also disturbs the treatment for other patients. Doctors will give the essential treatments — but overcrowding can delay the subsequent treatments. So it can lead to subpar [treatment].”
As a final reminder of how unacceptable and undesirable this situation is, Dr Rizal drew CodeBlue’s attention to a statement released last month by the International Federation for Emergency Medicine (IFEM) that found 100 per cent of 41 IFEM member countries surveyed in November 2022 reported overcrowding in their EDs.
“The current state of overcrowding at hospital Emergency Departments in many nations globally is an unacceptable and preventable threat to patient safety which must be immediately addressed,” said IFEM.
Dr Rizal told CodeBlue: “The new minister needs to address the AG’s audit report and take this seriously. So far, the upper management just ignored the audit report.”
Health Minister Dr Zaliha Mustafa has yet to issue a statement on CodeBlue’s 5,000-word report on HRPB’s overcrowded emergency department that had sparked personal anecdotes on Twitter of similar congestion in the EDs of government hospitals in other states.
Medical experts like Universiti Malaya’s Prof Dr Adeeba Kamarulzaman and former Health deputy director-general Dr Christopher Lee have similarly expressed concern about the wide-ranging problem across emergency rooms in busy public hospitals nationwide.
In a brief text to CodeBlue yesterday, Dr Zaliha said: “It is a chronic situation that of course needs to be addressed. It has to be looked into in a holistic manner and a sustainable solution.”









