KUALA LUMPUR, August 10 – A new report shows that annual direct health care costs from diabetes in Malaysia total about RM4.4 billion, 227 per cent higher than cancer (RM1.3 billion) and 11 per cent higher than cardiovascular disease (RM3.9 billion).
According to the report by the Ministry of Health (MOH) and the World Health Organization (WHO) released yesterday, the health care costs of diabetes (RM4.38 billion), cardiovascular disease (RM3.93 billion), and cancer (RM1.34 billion) ran upwards of RM9.65 billion, accounting for 16.8 per cent of total health expenditures, based on 2017 data across the public and private health care sectors.
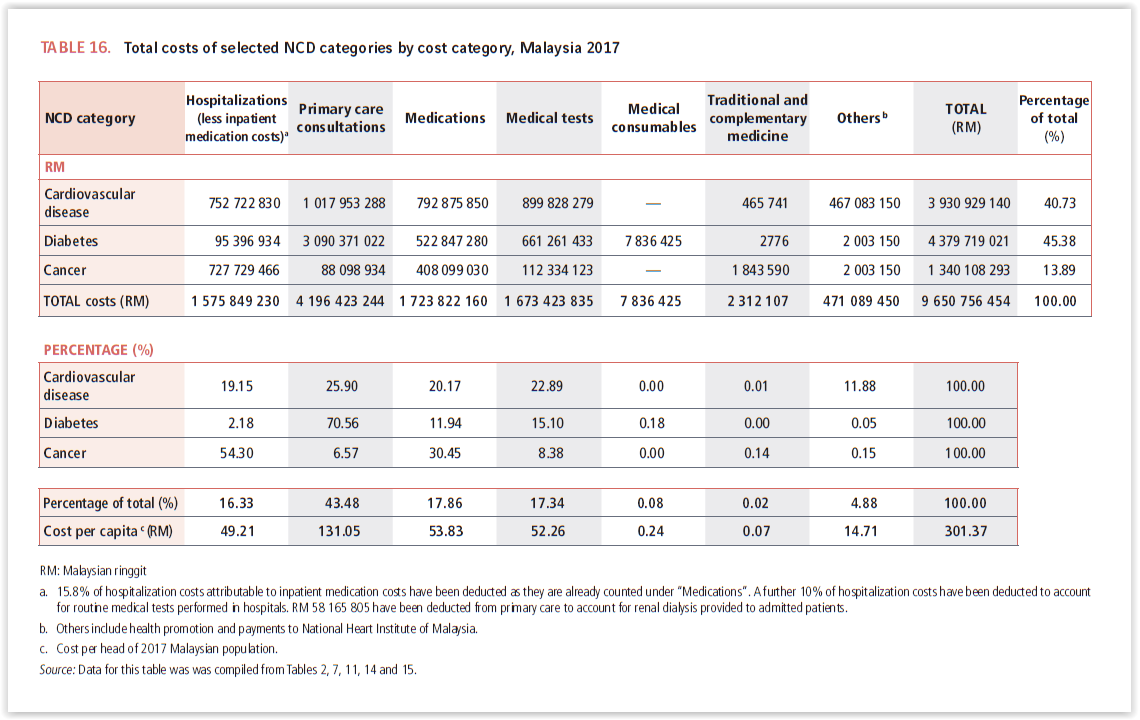
Diabetes consumed the highest annual health care spending among the three chronic illnesses at 45.4 per cent, compared to cardiovascular disease (CVD) at 40.7 per cent and cancer at 13.9 per cent. In other words, for every ringgit spent on the three NCDs, 45 sen goes to diabetes, 41 sen goes to CVD, and 14 sen to cancer.
The yearly direct health care costs of the three non-communicable diseases (NCDs) amounted to an average of RM301.37 spent per capita, or per head of the 2017 Malaysian population, with the figure set to increase as the population ages, according to the study by MOH and WHO’s Malaysia, Brunei Darussalam and Singapore office titled “The Direct Health-Care Cost of Noncommunicable Diseases in Malaysia”.
The largest components of the total annual direct health care costs across diabetes, CVD, and cancer were primary care and outpatient attendances that accounted for RM4.2 billion, or 43.5 per cent of the total, and medications at RM1.72 billion (17.9 per cent of total costs), followed closely by medical tests at RM1.67 billion (17.3 per cent of total costs).
Spending on hospitalisation across the three NCDs amounted to RM1.6 billion, comprising 16.3 per cent or the fourth largest component of total direct health care costs (excluding inpatient medication costs that were already counted under the “medications” cost).
Primary care and outpatient attendances for diabetes at RM3.1 billion were 325 per cent higher than hospitalisations for cancer at RM728 million and 311 per cent higher than hospitalisations for CVD at RM753 million.
The RM3.1 billion spending on primary care and outpatient attendances for diabetes was 204 per cent higher than that for CVD at RM1 billion and 3,408 per cent higher than that for cancer at RM88.1 million.
On medications, CVD took up the highest cost among the three chronic conditions at RM793 million, 52 per cent higher than diabetes (RM523 million) and 94 per cent higher than cancer (RM408 million).
As for medical tests, CVD comprised the largest cost out of the three NCDs at nearly RM900 million, 701 per cent higher than cancer at RM112 million and 36 per cent higher than diabetes at RM661 million.
The MOH-WHO study excluded complex tests like echocardiogram and coronary angiogram from the medical tests component for CVD, as these were assumed to be performed as inpatient and captured in the hospitalisation costs. CVD refers to a number of conditions: heart disease, heart attack, stroke, heart failure, arrhythmia, and heart valve problems.
Among the three NCDs, primary care and outpatient attendances formed the largest portion of costs for diabetes and CVD at 70.6 per cent and 25.9 per cent respectively; for cancer, hospitalisations accounted for the largest component of costs at 54.3 per cent.
Including Lost Productivity, Diabetes, CVD And Cancer Cost 1.6% Of GDP

Combined with lost productivity costs, the combined burden of diabetes, CVD, and cancer is estimated at RM22.53 billion, or 1.56 per cent of Malaysia’s GDP in 2017, a proportion considered to be small partly due to the fact that not all NCDs were costed in the MOH-WHO study.
The report, which drew heavily on MOH data, noted that the cost estimates were limited to the three largest categories of NCDs and excluded others such as respiratory diseases, mental health, and osteoarthritis, a common chronic joint condition.
Of the diseases included, some components of costs were not taken into consideration, given the lack of available data, such as rehabilitation, palliative, and long-term care.
“Therefore, we need to consider that these estimates are likely to be an underestimate of the true cost of these three NCDs,” said Jaithri Ananthapavan, health economist and public health researcher at Deakin University in Australia, who co-authored the report.
Martin Taylor, director of the health services department at the WHO Western Pacific Regional Office, said the underestimate of the costs involved, due to unavailable data, underlined an “urgency” to promote healthier lifestyles and activities.
“We know that what we’re seeing at the moment is the start of an upward curve, and therefore, a problem that needs to begin to be addressed now if we’re not going to be overwhelmed in the future,” Taylor said in a panel discussion at the launch of the report yesterday.
“It really reinforces the need to undertake that (promoting healthier lifestyles and activities) now to prevent a huge wave that could overwhelm the health care system and have economic consequences in the future.”
Direct health care costs included in the study covers hospitalisations, primary care and outpatient attendances, medications, medical consumables, medical tests, traditional and complementary medicine, and health promotion programmes.
CVD Tops Hospitalisation Discharge Costs

Hospitalisations refer to costs incurred when patients are admitted to hospital and treated as in-patients.
There were an estimated 350,789 hospital discharges in 2017 for the three NCDs. However, this excludes admissions in two hospitals under the Ministry of Higher Education and all five Ministry of Defence hospitals.
CVD accounted for 188,774 or 54 per cent of the estimated hospital discharges, followed by cancer at 138,396 hospital discharges, or 39 per cent.
Total cost of discharges from hospital amounted to RM2.1 billion, the bulk of which was attributable to CVD discharges (47.8 per cent) and cancer (46.2 per cent).
Diabetes accounted for only a very small proportion of both discharges and cost of discharges (6.7 per cent and 6.1 per cent, respectively). However, it is likely that many of the patients admitted with a principal diagnosis of CVD are very likely to have diabetes as a comorbidity, as it is a common precursor to a cardiovascular event, the report noted.
Diabetes Forms 32% Of Outpatient Attendances, But 74% Of Costs

Outpatient and primary care attendances refer to all medical attendances occuring outside the hospital in-patient system.
A total of 3,356,719 outpatient and primary care attendances were associated with a total cost of RM4.3 billion. CVD accounted for the largest number of attendances (2,017,021, or 60 per cent), but only 24 per cent of total costs (RM1 billion).
Diabetes patients, though they account for only 32 per cent of all attendances, accounted for 74 per cent of costs.
Cancer only accounted for 8.2 per cent of attendances and 2.1 per cent of total outpatient costs.
Of the total of 139,866 outpatient attendances recorded at the National Cancer Institute (NCI), the biggest share was for follow-up visits at 73.5 per cent (RM60 million) of the total costs of RM 81.5 million.
CVD Takes Up Nearly Half Of Medication Costs

Medications cover all medications used in the prevention and treatment of the three NCDs.
In 2017, about RM1.7 billion was expended on medications for the three selected NCD categories.
About 46 per cent (RM792.88 million) of this expenditure was incurred on drugs for patients with CVD, while the balance was reasonably evenly distributed between drugs for diabetes (30.3 per cent) and cancer (23.7 per cent).
Some 61.3 per cent of the drugs were distributed through the private sector; this proportion was greatest for cardiovascular drugs (70.5 per cent) and lowest for diabetes drugs (52.6 per cent).
The private sector accounted for RM1.1 billion on drugs for the three chronic conditions, the largest proportion being distributed through pharmacies, followed by private hospitals and private clinics.
The public sector accounted for RM667.7 million on medications for the three NCD categories (38.7 per cent of expenditure), with public hospitals accounting for the biggest proportion.
Cancer Screening Under 7% Of Medical Test Costs


For medical tests, on average, CVD patients accounted for the largest share of the expenditure at nearly RM900 million or 53.8 per cent of the total, followed by testing of diabetes patients at RM661.3 million (39.5 per cent) and cancer screening at RM112.3 million (6.7 per cent).
On cancer, spending on mammograms to check for breast cancer comprised RM94.4 million, while pap smears for cervical cancer cost RM17.8 million and immunological faecal occult blood tests spending amounted to about RM155,000.
Cancer Comprises 80% Of TCM Costs

For traditional and complementary medicine (TCM), the largest component of expenditure was for cancer at RM1.84 million or 79.7 per cent of total expenditure of RM2.3 million for the TCM cost category.
CVD accounted for nearly RM470,000 or 20.1 per cent.
The report noted that the biggest chunk of expenditure on TCM was on complementary Indian therapies for cancer patients at RM1.1 million, nearly half of the total RM2.3 million spending on TCM across cancer, CVD, and diabetes.
Study Limitations
Data from the MOH-WHO cost analysis study on diabetes, CVD, and cancer was mostly only available for MOH facilities that was then extrapolated to estimate expenditure in private facilities.
MOH was able to provide complete records for a cost component, such as Casemix data itemising inpatient costs and expenditure totals for specific drugs, in several instances. Estimated unit costs in the public sector were calculated using the two private sector fee schedules as a starting point.
The project was conducted remotely by the working group comprising officers from MOH and the WHO country office without any opportunity for in-country data collection.
A number of significant items were excluded from the costing due to the lack of readily accessible data, notably hospitalisations in two university teaching hospitals and all military hospitals; admissions to rehabilitation and long-term care facilities; day care and ambulatory care; outpatient rehabilitation services and allied health services; antibiotics, painkillers to treat complications of NCDs, but not specific to NCDs; electrocardiograms in outpatient settings; liver function tests and blood investigations for tumour markers; medical consumables; and TCM encounters in private facilities.
The total estimated direct health care costs of RM9.65 billion for diabetes, CVD, and cancer accounted for 16.8 per cent of total health expenditures in 2017, relatively small compared to the average 26 per cent proportion across 51 low- and middle-income countries.
However, researchers said this comparison should be interpreted with caution since the cost estimates were intended to reflect actual expenditures on the three NCDs in 2017. The estimates further only covered diagnosed and treated patients, excluding people with one or more of the three NCDs who were either undiagnosed or diagnosed but not treated.
The study authors also said that the RM22.53 billion combined cost burden from diabetes, CVD, and cancer (including lost productivity costs), equivalent to 1.56 per cent of Malaysia’s 2017 GDP, likely reflected insufficient resources being invested in the prevention and early diagnosis of NCDs.
“I think it’s important to keep in mind that NCDs are largely avoidable. And so what this report shows and these estimates show is that greater investment in prevention is really required to contain this economic burden,” Jaithri told the panel discussion.
“But a limitation of the cost of illness studies is that it tells you the size of the burden, but it doesn’t tell you what you need to do about it. And to do that, we need cost effective analysis to actually show where we should invest our time and money to have the greatest value for money impact on these NCDs.”
The MOH-WHO report was primarily written by Prof Marj Moodie (lead investigator), and Huong Ngoc Quynh Tran and Jaithri Ananthapavan from Deakin Health Economics, Institute of Health Transformation, School of Health and Social Development, Deakin University.