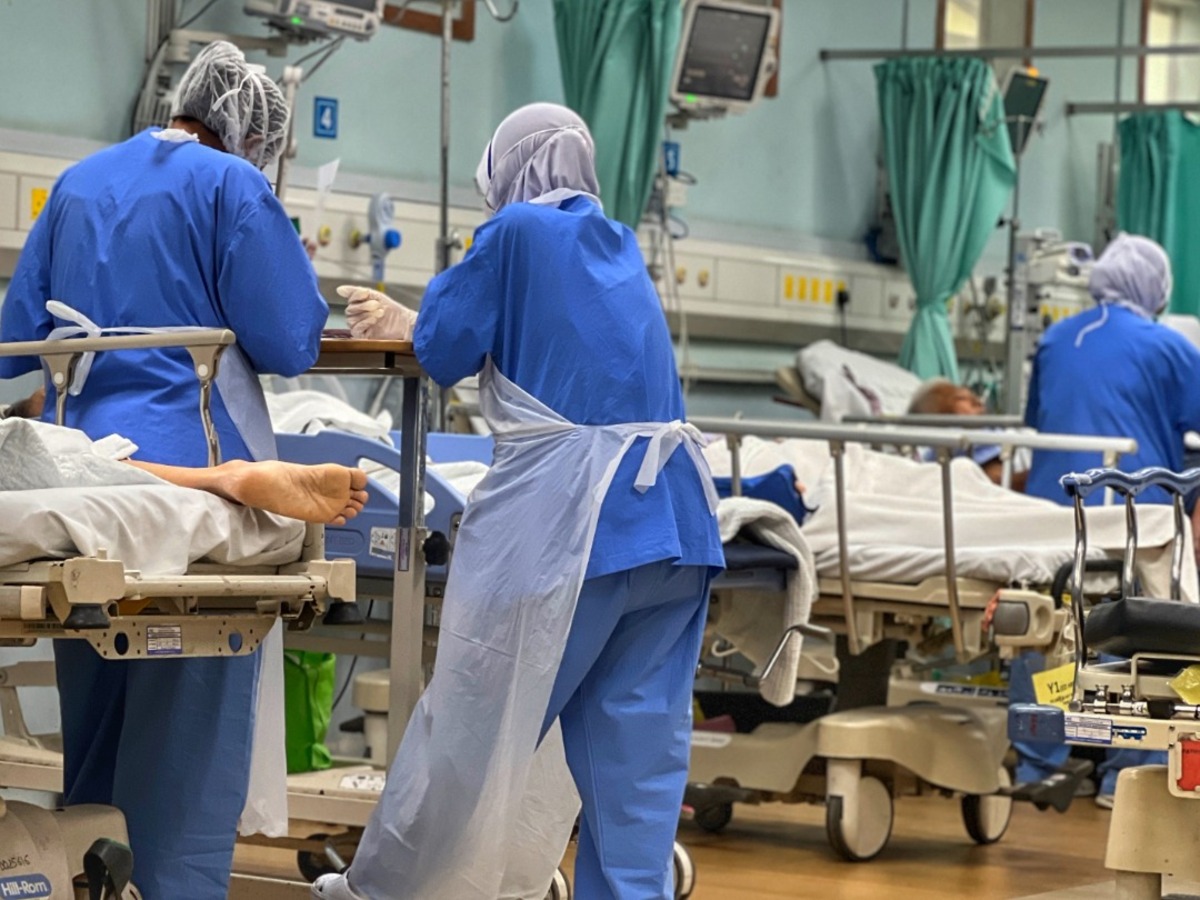
KUALA LUMPUR, August 7 – The highly disruptive relocations of over 4,000 medical officers reveals fundamental flaws in the Ministry of Health’s (MOH) human resource management, said the Galen Centre for Health and Social Policy.
Galen Centre chief executive Azrul Mohd Khalib affirmed concerns from multiple government doctors about the impact of staffing shortages triggered by the massive relocation exercise – particularly in severely affected states and tertiary hospitals – notably patient harm from delayed or inadequate care.
“They are concerned that this will result in the loss of life, premature deaths of patients. Unfortunately, we will need to monitor the five most affected hospitals and the three states most affected by this exercise for these indicators. They will happen,” Azrul told CodeBlue.
Obstetrics & gynaecology (O&G) doctors at Selayang Hospital have openly highlighted concerns of substandard care and even patient mortality due to the relocations stripping their already understaffed department of medical officers, as O&G is an “unpredictable” department where “anything can happen at any time”.
CodeBlue previously reported that five tertiary referral centres – Tuanku Ja’afar Seremban Hospital in Negeri Sembilan, Melaka Hospital, and three in Selangor (Sungai Buloh Hospital, Sultan Idris Shah Serdang Hospital, and Selayang Hospital) – lost more than 80 to nearly 120 medical officers each.
The doctor relocation exercise primarily benefited Sabah, Sarawak, Johor, and Pahang – each of which received more than 400 to over 500 net medical officers – at the expense of the Klang Valley (Selangor and the federal territories of Kuala Lumpur and Putrajaya), Melaka, and Negeri Sembilan that suffered net losses each of between 130 and nearly 190 doctors.
“MOH’s human resource system is fundamentally flawed. It is anchored by the Public Services Commission (SPA) which treats all civil servants equally. This is the mistake,” Azrul said.
“Doctors should be treated special. Period. As a result of the Covid-19 crisis, we are arguably more vulnerable and exposed to future health emergencies than before 2020.
“During the pandemic and every day today, these are the professionals who are there with people on the worst day of their lives while they are sick, injured, or dying. We depend on them and, yes, need them, especially those who work in the public sector. We cannot afford to lose even one of them. It would be a mistake to treat this as business as usual.”
Azrul Mohd Khalib, chief executive of the Galen Centre for Health and Social Policy
The Health White Paper (HWP) tabled by Health Minister Dr Zaliha Mustafa – a document outlining health reforms over a period of 15 years that was recently passed by Parliament – completely omitted mention of setting up a Health Services Commission to regulate health care professionals in the public sector separately from other civil servants.
During debate in the Dewan Rakyat last June on the HWP, Dr Zaliha dismissed the need for a Health Services Commission, saying that this required two-thirds majority to amend the Federal Constitution and that the separate commission would not solve issues in the MOH. The Pakatan Harapan-Barisan Nasional unity government has previously boasted two-thirds majority in Parliament.
Azrul pointed out that unlike doctors, other civil servants are not usually asked to work up to 33 hours straight. Teachers, he noted, work regular hours between 7.30am and 4.30pm.
“Doctors work those hours [33 hours], may be on call, and be required to be available and working when their counterparts are already in bed. This can happen many times in a month. Some are worked to the point of mental and physical exhaustion.
“Tired and weak, doctors have even lost their lives due to road traffic accidents returning home from work. The responsibility of effectively treating and sometimes, survival of patients, are placed on the shoulders of such individuals.
“Public health care workers, particularly doctors and nurses, are not like other civil servants. This is why they need their own Health Services Commission.”
Why Begrudge RM5,000 Relocation Cost At The Price Of Losing RM1 Million Investment Into Training Per Doctor?
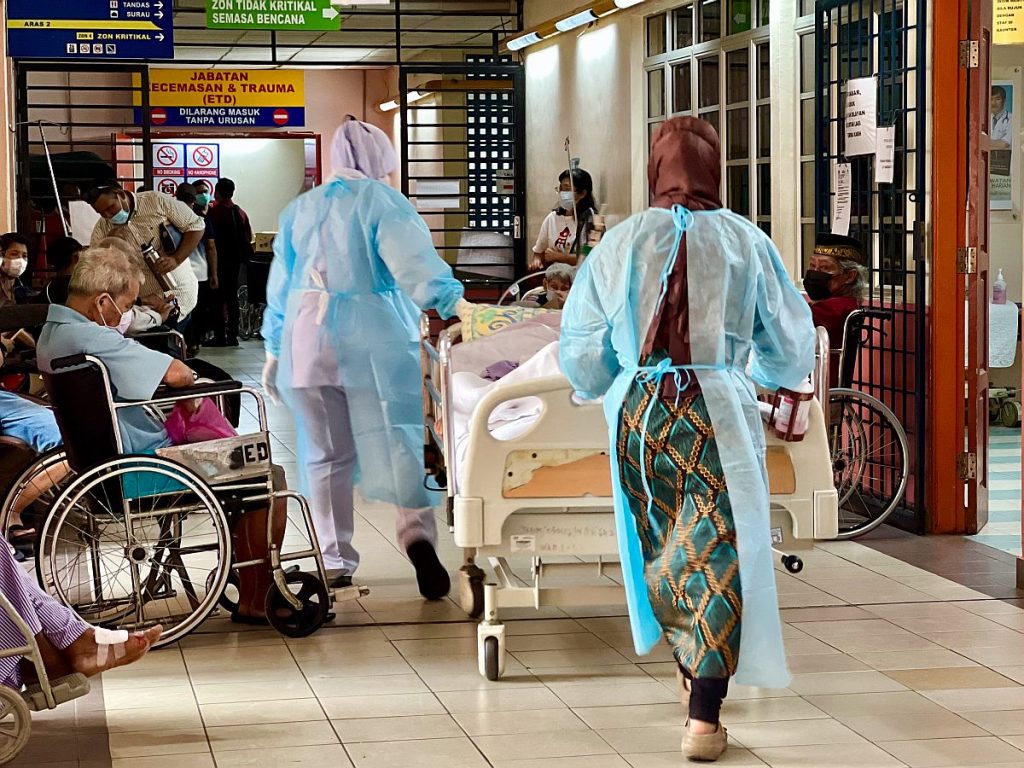
Azrul said the redistribution of medical officers demonstrated the lack of efficiency and level of disconnect between doctors, health care facilities, and top decision makers in Putrajaya.
“This measure is likely to cause severe disruptions across all affected hospital departments and clinics, especially for those states whose medical facilities will not be receiving any medical officers to replace those which have been assigned to new posts,” he said.
“It is causing conflict, dissatisfaction and disgruntlement among the affected health care professionals when the costs associated with the relocation, which are in the thousands of ringgit, are not covered due to a technicality, despite years of service.
“There are no offers of assistance. It implies a lack of appreciation and recognition, complacency, and apathy.”
Azrul Mohd Khalib, chief executive of the Galen Center for Health and Social Policy
The 4,700 over government health care professionals (over 4,100 doctors, as well as more than 600 dentists and pharmacists) – who obtained placements for permanent positions this year – were not eligible to claim for transfer expenses because of a disruption in their period of service from contract to permanent.
The Galen Centre questioned why the MOH merged permanent position offers with a mass redistribution exercise. The date for effect of the permanent appointments was the same as the date to report for duty: last July 31.
“It could have offered the permanent positions first, followed by the relocation later,” Azrul said.
“This could imply that Putrajaya is unwilling to foot the bill of relocating thousands of affected health care workers estimated to be at least RM30 million. If they were already permanent workers, the government would be obligated to pay for the costs of the transfers. This way, the government would not have to pay.
“If that were the case, I am bewildered how the government would begrudge paying at least RM5,000 for the cost of relocation, when the estimated investment which has gone into training one doctor is almost RM1 million. We would lose that and the years of experience, each time a doctor leaves in despair.”
Azrul Mohd Khalib, chief executive of the Galen Centre for Health and Social Policy
The Galen Centre noted that medical officers have rejected offers of permanent positions, “as they feel pragmatically that they cannot afford to move their households during a cost of living crisis”.
CodeBlue reported a doctor as saying that of the 49 medical officers assigned to Dungun Hospital, only 30 plus reported for duty last July 31. When this group reported for duty at Dungun Hospital, they found out that their actual placement was at the new non-operational Dungun Hospital, a “sick project” that was still under construction.
Most of the 30 plus medical officers were redirected to “temporary” postings to other hospitals in Terengganu, many of whom chose not to report for duty, including one who resigned from their job, the source said.
Separately, a pregnant medical officer based in Kuala Lumpur – who said she had to choose Klinik Kesihatan Kapit in Sarawak for placement as there were no spots available in the Klang Valley – told CodeBlue that just a couple of days prior to the reporting day, the MOH’s human resource changed her placement to a hospital in Johor.
“I gave up on my permanent post,” said Dr Anna Mae (pseudonym), adding that she plans to join the private sector after she gives birth to her second child in January next year.
It’s Not Just About Filling Vacancies, Doctors Can’t Be Uprooted Without Consequence

Dr Zaliha recently said vacancies would be filled by December, five months away, to address doctor shortages in certain hospitals.
The Galen Centre pointed out that some of the vacancies have existed much earlier, due to increased burnout, depression, and job satisfaction among health care workers caused by the Covid-19 pandemic.
“We will be lucky if these vacancies will be filled by December,” Azrul said.
“This is not about simply filling vacant positions. This is about being able to provide the same level of service as before the redistributions. You cannot treat doctors as if they can be easily uprooted and transplanted across the country without consequences.
“Many have already worked several years with the Ministry of Health as contract workers. Many have families or take care of elderly parents. Some are young mothers who are breastfeeding or currently expecting.”
The Galen Centre added that burnout and staff resignations among health care workers have become more chronic since the Covid-19 crisis, but are not documented.
“Anybody who claims that high numbers of resignations and burnouts in public health care services are normal and this is business as usual do not know what they are talking about.”
Azrul Mohd Khalib, chief executive of the Galen Centre for Health and Social Policy
“The pandemic has caused massive burnout and untold trauma to health care workers which has mostly gone undiagnosed and untreated. When compared to before the pandemic, resignations have risen to 1,000 per cent higher when compared to five years ago,” Azrul said.
“The ongoing redistribution of doctors’ exercise is likely to cause more harm than good as it will push doctors who are on the verge of resigning, to finally decide to throw in the towel. We might lose more doctors through this exercise. I do not think the Ministry of Health has taken this into account.”
Emergency Services And Specialised Care Will All Be Disrupted

The Galen Centre expects the first three months of the relocations to be critical in determining the impact of staff shortages on health care services and waiting times.
“This is due to a number of reasons: fundamentally, in many departments, there will now be fewer doctors available to meet with patients for consultation; there are doctors who need familiarisation or training in their new departments; the number of patients coming in will not likely reduce, but the capacity of the health care facility to properly provide care or even see patients will be significantly affected.”
Azrul said public hospitals would likely be forced to turn patients away or refer them elsewhere, such as to private health care facilities, to prevent people from wasting hours in the emergency department.
“Those responsible in managing the health services must recognise that avoiding causing harm to people who are seeking medical attention is more important than the optics of asking people to go elsewhere,” he stressed.
“Would you prefer they wait eight hours before being seen by a doctor in a congested public hospital, or telling them that it would be better if they go to a private clinic or hospital?”
Azrul Mohd Khalib, chief executive of the Galen Centre for Health and Social Policy
Doctors have warned the MOH that the relocation exercise would exacerbate waiting times in the emergency department for admission that are extremely long as it is: at least one to two days for admission and up to four days for intensive care unit (ICU) beds at Kuala Lumpur Hospital; two to three days at Melaka Hospital; and over 12 hours at Tuanku Ja’afar Seremban Hospital.
The Galen Centre also highlighted disruptions to specialised care, such as oncology, nephrology, or even dermatology, due to the departures of trained medical officers from transfers.
“Even with new doctors coming in, it could take several months to train a person to reach the level of expected proficiency. Consultations, surgeries, and follow-up sessions will all be disrupted.”
A surgeon at Melaka Hospital – who said the general hospital is looking at halving the number of elective surgeries offered due to the exodus of medical officers transferring out – noted that patients were already waiting two and a half to three months for certain surgeries.
“The leadership of the government and Ministry of Health must step up and fight for the welfare and wellbeing of health workers. We owe a duty of care to them,” Azrul said.