Malaysia reached two Covid-19 milestones in February 2021.
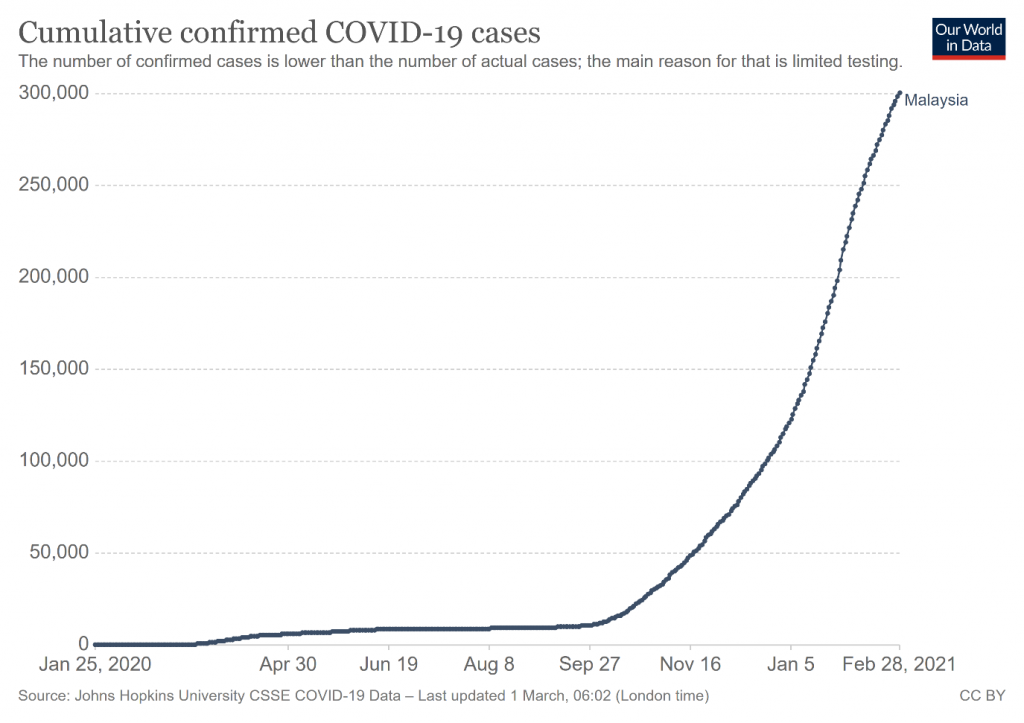
On February 28, 2021, the number of cumulative confirmed cases exceeded 300,000. Since September 2020, the numbers have been trending upwards. The number of cumulative confirmed positive cases exceeded 100,000 and 200,000 on December 24, 2020 and January 28, 2021 respectively. It took 334 days, 35 days and 31 days to exceed 100,000, 200,000 and 300,000 cases respectively.
On February 18, 2021, Malaysia’s ranking in the global league of cumulative confirmed cases reached 45, a jump from a ranking of 85 on November 18, 2020, within three months.
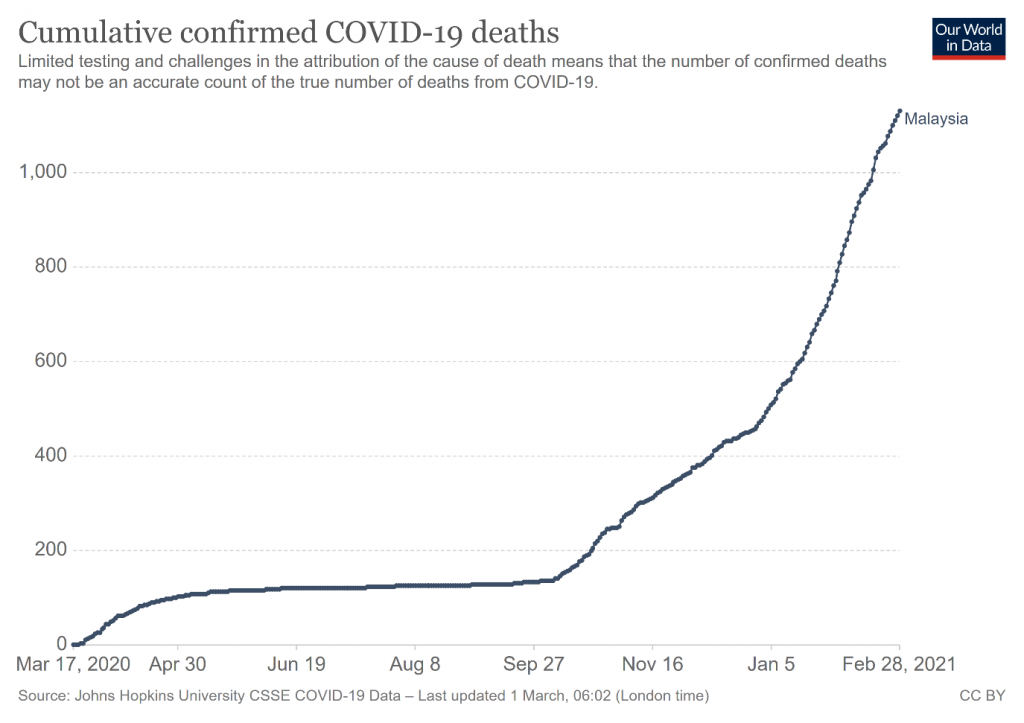
The deaths from Covid-19 showed a similar trend with 471 deaths in 2020, 289 in January 2021 and 370 in February 2021. What was disturbing were those who were brought in dead (“BID”). This phenomenon would not be unexpected in Sabah because of poverty and infrastructural deficiencies there. But what was unexpected was that the third and fourth highest BID rates were in urbanised Kuala Lumpur and Selangor. The delays in the reporting of BID was also unexpected.
The official daily narrative about the number of cases, the almost daily publication of R-naught since the end of January 2021 and the introduction of Covid-19 vaccination have led many to perceive that Malaysia has turned the corner. This perception was fostered by the official statement that the number of cases may possibly drop to two digits by May 2021.
But has Malaysia turned the Covid-19 corner? The following considerations would help in providing some answers.
What Is The Prevalence Of Covid-19 In Malaysia?
This is the unaddressed question which may shed some light on the prevalence of the infection.
Serology surveys that are able to detect antibodies after Covid-19 infection have the potential to identify those who were asymptomatic and were not identified by symptom reporting, thereby providing a more complete picture of the prevalence and severity of the disease. Repeating these tests will provide better understanding of the prevalence in the population.
The Health Ministry has not published any serology surveys that it may have carried out.
However, data from other countries report that the Covid-19 prevalence is between 10 and 15 times the numbers tested positive.
For example, a China Centre for Disease Control seroprevalence study of 34,857 participants in Wuhan, Hebei and six other provinces after containment of the first wave reported a 4.43 per cent prevalence in Wuhan followed by 0.44 per cent in Hebei province (outside Wuhan), and less than 0.1 per cent in the other provinces.
As Wuhan has an estimated population of about 11 million and reported about 50,000 cases, it suggests that about 500,000 i.e. 10 times the cases, may have been infected.
The actual numbers infected i.e. prevalence in Malaysia is unknown. Based on data from other countries, it is likely that between 3 to 4.5 million in Malaysia have been infected i.e. between 9 to 14 in 100 in Malaysia have been infected. And it is rising!
Has The MCO Helped?
The World Health Organization situation report has stated there was community transmission in Malaysia since September 2020.
Yet the country is still subjected to the inappropriate containment intervention of the Movement Control Order (“MCO”) when mitigation interventions are needed.
The narrative that the MCO, since January 13, 2021, has reduced the number of positive cases was, in the words of a former Deputy Director General (Public Health), “an epidemiological artifact. The number of reported cases follows the trend of testing of samples. The more you test, the more cases will be reported. When the number of samples tested decreases, the number of cases also declines.” There was an increase of testing in the first week of 2021 but a subsequent decline from the third week of 2021.
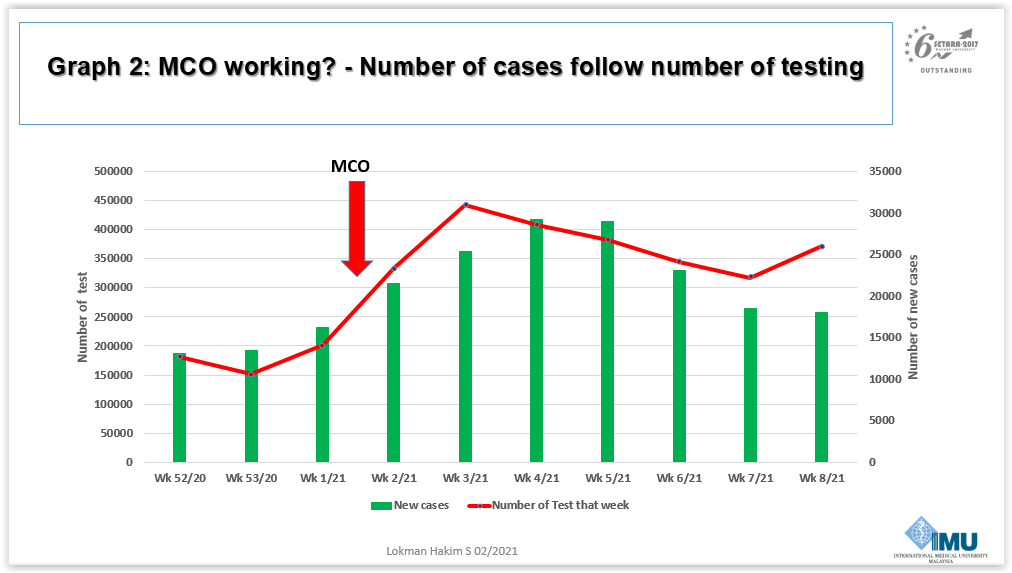
Variants
When any virus spreads to the population, they evolve over time, through mutations, which are changes in the viral genetic sequence. As such the emergence of new variants is not unexpected.
A changed virus is called a variant of the original virus. Variants can differ by one mutation or many. These changes may result in the virus spreading more easily, increase disease severity or influence the efficacy of diagnostics, therapeutics or vaccines.
The more the SARS-CoV-2 virus, which causes Covid-19, circulates through its spread in the population, the more opportunities it has to mutate and spawn new variants.
The United Kingdom warned in December 2020 of a new, more transmissible variant that was rapidly becoming the dominant form of the virus there. At about the same time, there were reports of the impact of faster-spreading variants in South Africa and Brazil.
Variants have also been reported in the United States, an increasing number of countries in Europe and Asia. The UK variant is expected to become the dominant strain in the US within this month.
The impact of the variants on vaccines became evident in late January 2021. Novavax reported that its clinical trial data reported that its vaccine had 89 per cent efficacy in the UK, but only 49 per cent in South Africa.
About a week later, data revealed that the AstraZeneca vaccine only provided limited protection from mild to moderate disease against the South African variant. Johnson and Johnson’s vaccine had 57 per cent efficacy in South Africa, 66per cent in Latin America, compared to 72 per cent in the US.
The US Centers for Disease Control and Prevention director, Rochelle Walensky, warned, on March 1, 2021, “Please hear me clearly; at this level of cases, with variants spreading, we stand to completely lose the hard-earned ground we have gained. These variants are a very real threat to our people and our progress.”
Michael Osterholm, an epidemiologist and director of the Centre for Infectious Disease Research and Policy at the University of Minnesota, who advised Joe Biden’s transition team on the pandemic, warned on NBC’s Meet the Press on 31 January 2021 that a category 5 Covid-19 hurricane is approaching the US.
According to Malaysia’s Health Ministry, the UK variant was found in a returnee in December 2020. Six cases of the South African variant were reported in the Philippines on March 2, 2021.
A global consensus is emerging that the main variants are more transmissible and may evade infection- and vaccine-induced immunity.
The continuing diversification of the SARS-CoV-2 virus could prolong the pandemic substantially and vaccination programmes with variant- specific vaccines are likely to be required.
Gene sequencing of the virus in Malaysia is limited compared to other countries, with no published reports on the prevalence of the variants in Malaysia.
Reinfection
There are increasing reports of reinfection of persons who previously had Covid-19 infection. These have involved existing strains, but evidence of reinfection involving the E484K mutation have been reported in Brazil.
Reports of secondary infection have also been reported in Hong Kong, Holland, Belgium, Poland, Ecuador, and the US.
Could the brought in dead (“BID”) cases been due to reinfection, particularly those in the urbanised states? Whether reinfection has occurred in Malaysia and, if so, the prevalence has not been published.
The susceptibility of previously infected individuals to reinfection is currently not well understood.
Migrant Workers
There are an estimated two million documented migrant workers in Malaysia, with an unknown number of undocumented workers.
Although foreigners comprised 23.8 per cent of 5,889 consecutive Covid-19 cases treatment in 18 Malaysian public hospitals between February 1, 2020 and May 30, 2020, there was no organised screening until January 1, 2021 i.e. seven months later, when screening of migrant workers was made mandatory in the Klang Valley. This was later extended to other states.
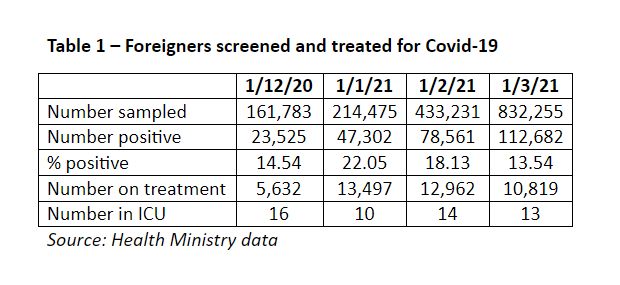
Screening of migrant workers only took off in February 2021 with a positivity rate between 13.54 per cent and 22.05 per cent.
If the current positivity rates are extrapolated to the estimated 1.2 million migrant workers yet to be screened, the estimated additional number of positives could potentially be between 162,500 and 264,600. This assumes that there is no undetected infection or re-infection among the migrant workers as the migrant workers are not screened regularly.
How many cases are there among the undocumented migrant workers?
The root cause of the overcrowding of migrants’ living accommodation, which is a breeding ground for Covid-19, has yet to be addressed.
Vaccination
Covid-19 vaccination started on February 24, 2021. The government has targeted to complete vaccination of 70 – 80 per cent of the population by the first quarter of 2022.
The clinical trials of the vaccines were done at different phases of the pandemic in different countries. The clinical trials of some vaccines were completed by the time the variants came on the scene, unlike that of the others which were completed earlier. Whether the latter are just as effective against the variants is yet to be worked out.
The key questions are whether vaccination and newer versions of vaccines can run ahead of the variants. If not, those who have not been vaccinated would be at increased risk of infection by the variants.
The attitude of those vaccinated towards the continued use of non-pharmaceutical interventions e.g. physical distancing, use of masks, frequent hand washing, and avoidance of crowded places, confined spaces and close contacts are critical. Will these individuals, particularly those who think they have more rights than the general public, throw caution to the wind?
There are also availability and logistics issues with vaccination that need to be streamlined as they would impact the Covid-19 situation in Malaysia.
Summary
Can anyone state that the Covid-19 variants, the susceptibility of previously infected individuals to reinfection, and prevalence among migrant workers will not impact the situation in Malaysia?
Would Covid-19 become endemic?
Would current vaccines provide sufficient protection or would repeat vaccinations be necessary?
It would be brave for anyone to claim or give the impression that Malaysia has turned the Covid-19 corner.

Dr Milton Lum is a past President of the Federation of Private Medical Associations, Malaysia and the Malaysian Medical Association. This article is not intended to replace, dictate or define evaluation by a qualified doctor. The views expressed do not represent that of any organisation the writer is associated with.
- This is the personal opinion of the writer or publication and does not necessarily represent the views of CodeBlue.








