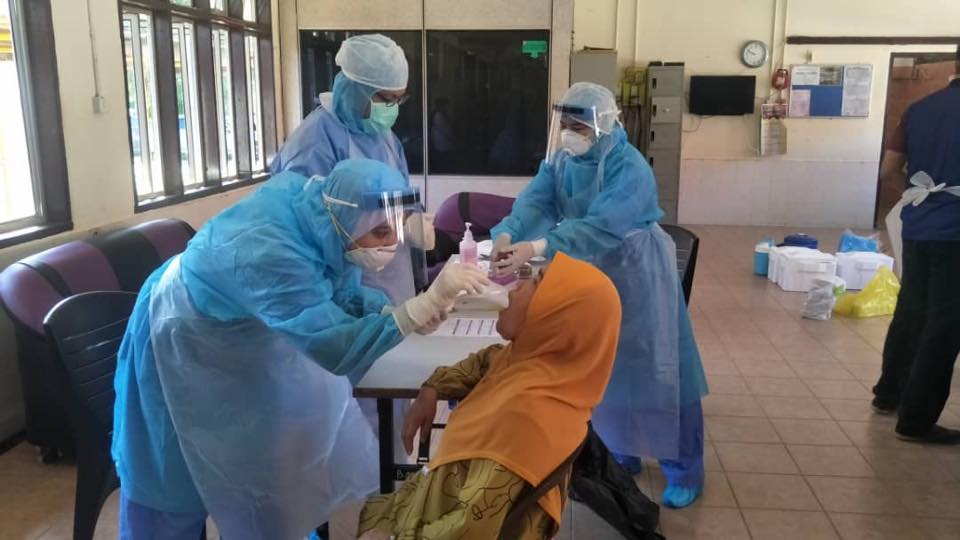
On June 4, 2020, the Director-General of Health Malaysia said exposure to infected detainees at the Bukit Jalil Immigration Centre in Kuala Lumpur had caused 270 other migrants to contract Covid-19. The new cases were discovered after the second samples were taken from detainees at the centre.
This cluster was first announced by DG on May 21, two days after Myanmar informed that at least five of its nationals had tested positive for the virus after being deported from Malaysia. Around 645 individuals in Bukit Jalil had their samples taken, 35 tested positive, 400 tested negative while 210 more were still awaiting results.
By May 28, Bukit Jalil had 283 cases with no pending results out of 1,545 samples screened (1,421 detainees, one child of detainee, 123 staff).
According to the Lapuran Kluster Covid19 yang Aktif (Report of Active Covid19 clusters) there were no cases the next three days till Wednesday June 3 (55 cases, total 338) and June 4 (270 new, total 608).
It was not clear if the 55 on June 3 and 270 on the 4th were new positive cases from swabs taken each day, or positive laboratory results which were progressively released from tests on the second round of (?1,545) swabs taken (?June 1-2).
Spikes In Daily Positive Covid Cases In DG’s Press Releases – Correlation With Laboratory Results Or Active Case Detection Or Real Ongoing Transmission?
I would like to know the present field-to-laboratory turn-around time for RT-PCR from nasal swab collection to results release for our Ministry of Health.
The implications of this apparent “sudden spike of large numbers of positive cases” after a few days of zero in this centre, will be less alarming if we had been told that the positives announced on 3rd and 4th were the results of large numbers of second round of swabs taken on days prior to it (active case detection).
If we knew that on the 29 May – 31 May (weekend) no nasal swabs were taken at Bukit Jalil, we would understand that zero positive on those days refers to “no results” or “no test done”, rather than “no positive case”.
If, however, the daily swabs from contact tracing and active case detection are taken regardless of public holidays or Sundays from detainees, and there had been really zero positives since 28th, the sudden surge of new cases would be alarming indeed.
It is clear that active transmission is ongoing in the Bukit Jalil centre and a total of 608 (as of 4 June) out of 1,422 detainees had contracted Covid presumably while in detention. I have not seen any report of any staff being infected.
The good news (epidemiologically, not politically) is that 42.7% of the detainees have been infected, raising the herd immunity there. Being young and without medical comorbidities, they should recover under good medical monitoring. Hopefully, when they return to their countries, they will have some degree of protection. But who is case #0?
Asymptomatic Transmission — The Achilles’ Heel Of Current Strategies To Control Covid-19
There are published reports on Covid-19 outbreaks in nursing facilities in USA which show the devastating tsunami of cases and deaths among residents, staff and visitors that could arise from a single infected case in enclosed populations.
The reports also point to the large number of cases without symptoms, who were identified only during active case detection with nasal swabs.
Ineffective infection control and preventive measures and staff members working in multiple facilities contributed to the intra- and inter-facility spread.
On February 28, a woman resident of a long-term care skilled nursing facility (SNF) in King County, Washington was confirmed positive for Covid-19.
As of March 18, 167 confirmed cases (101 residents, 50 health care personnel and 16 visitors) were epidemiologically linked to the facility. Except for seven in whom no symptoms were documented, most cases among residents included respiratory illness consistent with Covid-19. 54.5% of the 101 residents had to be hospitalised and 34 died. 6% staff had to be hospitalised, none died.
Symptom-based screening in skilled nursing facilities failed to identify approximately half of residents with Covid-19.
A symptomatic health care provider worked at a second SNF, also in King County on 26, 28 February. On 1 March, she tested positive for Covid-19. By 6 March, seven residents were symptomatic and tested positive.
On 13 March, CDC performed symptom assessments and RT-PCR twice (13 Mar, 19-20th) for 76 of the 82 residents. They were categorised as asymptomatic or symptomatic at the time of testing, based on the absence or presence of fever, cough, shortness of breath, or other symptoms on the day of testing or during the preceding 14 days.
Among 76 residents, 48 (63%) had positive RT-PCR results, with 27 (56%) asymptomatic. Symptoms subsequently developed in 24 of these 27 residents (within a median of 4 days) and they were reclassified as pre-symptomatic. By the end of this outbreak, 57 residents had tested positive, 15 (26%) died.
The RT-PCR indicated large quantities of viral RNA in asymptomatic, pre-symptomatic, and symptomatic residents, suggesting the potential for transmission regardless of symptoms.
It is notable that 17 of 24 specimens (71%) from pre-symptomatic persons had viable virus by culture one to six days before the development of symptoms.
Preparing For Covid-19 In Nursing Homes – CDC Guidelines May 2020
- Nearly one in 10 nursing homes nationwide in USA has reported coronavirus cases. The death rate for infected residents may be more than 25-35%.
- Long term care facilities, institutions with enclosed populations (e.g. prisons, shelters), mental hospitals, hospitalised inpatients should take proactive steps to prevent introduction of SARS-CoV-2.
- Visitors and staff members should be screened for potential infection and history of contact.
- All new residents may need to be routinely RT-PCR screened on admission.
- Once a confirmed case is identified, all residents should be placed on isolation. Symptom-based screening alone will miss a high proportion of infectious cases and is not enough to control transmission in this setting. Mass screening is preferred, with isolation of confirmed cases and quarantine of contacts.
- Protection for staff if possible with personal protective equipment (PPE) when dealing with confirmed or suspects.
For more on “Covid-19 in older adults”, check out Aman Nanda.

A fusion opinion from a Sarawakian public health specialist, paediatrician, ex-associate professor, disaster relief and medical volunteer, passionate about helping people learn.
- This is the personal opinion of the writer or publication and does not necessarily represent the views of CodeBlue.