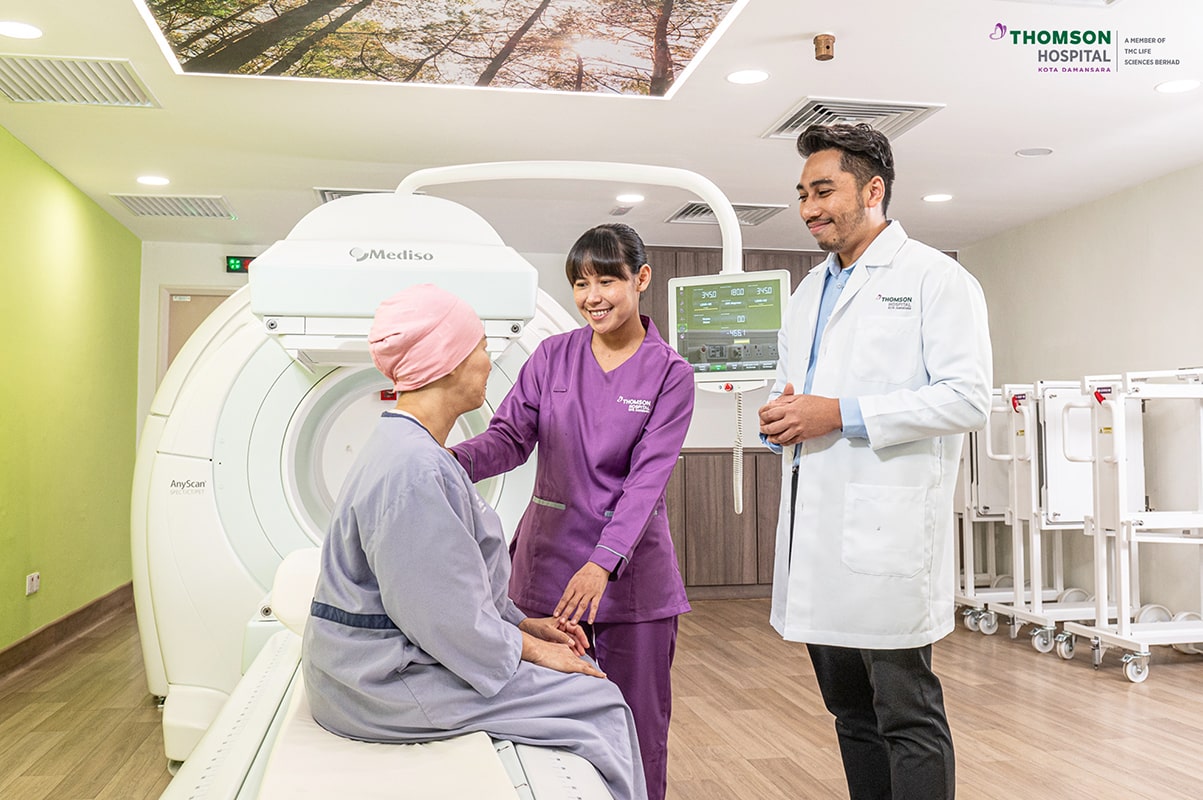
KUALA LUMPUR, Oct 6 – Thomson Hospital Kota Damansara (THKD) recently launched a new oncology and nuclear medicine facility, providing cancer patients treatment that is tailored to their specific needs.
At Oncology and Nuclear Medicine @ Thomson Hospital Kota Damansara, Selangor, the Mediso AnyScan SPECT/CT/PET imaging system provides clinicians with highly detailed and accurate information to improve the precision and effectiveness of cancer treatment.
The system combines SPECT (single photon emission computed tomography), CT (computed tomography), and PET (positron emission tomography) technologies into a single device, allowing doctors to gain a more complete understanding of the patient’s condition.
This includes identifying the location, size, and metabolic activity of cancerous tissues, that can help doctors choose treatment strategies that are tailored to the patient’s specific needs.
“Oncology & Nuclear Medicine @ Thomson Hospital is designed to house all cancer treatment modalities under one facility to provide multi-disciplinary care with the best experience throughout the entire patient journey,” said THKD CEO Nadiah Wan.
Dr Zool Hilmi Awang, who heads the nuclear medicine department, said the facility not only offers tools that can accurately identify problematic areas in the body and diagnose diseased cells, but also offers safe radioactive tracer injections that can help detect different kinds of cancer cells, like neuroendocrine tumours, prostate cancer, and thyroid cancer.
Using these advanced tools, physicians can more effectively target and treat visible areas of cancer cells, he said.

Oncology and Nuclear Medicine @ Thomson Hospital offers a range of cancer treatments as well as systemic therapy, which includes chemotherapy, targeted therapy and immunotherapy, radiotherapy, nuclear medicine, and surgical services all under one roof.
The facility has performed over 2,600 diagnostic and therapeutic procedures with oncology patients in areas such as cervix, breast, lung, rectum, head, neck, and brain.
Among these, the radiotherapy team has treated breast cancer patients using the Deep Inspiration Breath Hold technique, and brain cancer with radiosurgery and craniospinal irradiation.
THKD is equipped with the state-of-the-art linear accelerator (LINAC) that has a surface image guided system (SIGRT). It is capable of treating various types of cancers and conditions.
Its nuclear medicine team has also performed PETCT scans that helped in detection and staging of various cancers. The facility also performed whole body I-131 scans for thyroid cancer patients.
Through these diagnostic scans, physicians can further determine and provide the most suitable treatment for patient. In nuclear medicine, THKD has also performed therapy like low dose I-131 for thryroid cancers and Lu-177 PSMA therapy for prostate cancer.
FAQs About Radiotherapy

“Each patient is special. There is no one-size-fits-all,” said Dr Tan Chih Kiang, consultant clinical oncologist and head of clinical oncology.
Dr Tan answered some of the most frequently asked questions about radiotherapy.
Radiotherapy and systemic therapy are different from each other. Radiotherapy uses radiation to treat and control the cancer, whereas systemic therapy, such as targeted therapy, uses drugs or medicines to treat the cancer.
“We cannot substitute one with another,” Dr Tan said.
“Different types of cancer, different stages, and intent of the treatment will influence the choice of treatment being chosen. So normally, the oncologist will assess the patient’s condition, the type and stage of cancer, before deciding whether to use systemic therapy, radiotherapy, or the combination of both to treat the cancer itself.”
Side effects from radiotherapy depend on a few factors, such as the area the radiation is given, the dose, as well as the number of sessions.
“We call it fractions. So I’ll give you two examples here: Example number one, radiotherapy given to the pelvic region for rectum cancer, for instance, may cause skin redness, diarrhoea, and urinary tract infection. Whereas, radiotherapy to the head and neck region from nasopharyngeal carcinoma may cause skin burn, sore throat, oral ulcer, or altered taste or dry mouth,” said Dr Tan.
“So, in summary, radiotherapy to different parts of your body may have different side effects.”
The consultant clinical oncologist also said radiotherapy generally does not cause hair loss, unless the radiotherapy is given for brain tumour, where the scalp receives a high dose of radiation.
Each radiotherapy session takes between 10 and 30 minutes, which normally is an outpatient procedure.
On the do’s and don’ts after radiotherapy, Dr Tan suggested eating a well-balanced diet, doing light exercise, and wearing loose clothing during the radiotherapy session to avoid friction between the fabric and treated skin area.
He also recommended to stop smoking because smoking will aggravate side effects and cautioned radiotherapy patients against applying cream or ointment on the treated area without consulting their doctor, as this may worsen skin side effects.
“Nowadays, it is very common for patients, family, friends, or even the public to search through Google or ask Dr Google on some questions relating to the treatment for cancer. So my advice is to not trust everything that Google provides because most of this information has not been validated.
“My advice to patients is to seek advice from your doctors, be aware of your own conditions, and what are the treatment options and the pros and cons before you make the decision.”
Myths About Breast Cancer

Dr Tan Gie Hooi, a consultant breast and oncoplastic surgeon at THKD, corrected several myths about breast cancer.
She explained that women have increased risk of getting breast cancer, compared to the average person, if they have a first-degree relative with the condition, such as their mother, sister, or daughter.
“Using deodorant does not cause breast cancer,” Dr Gie Hooi added.
Another myth is that wearing underwire bras increases a woman’s risk of getting breast cancer.
Men can also get breast cancer. “But of course their chances of getting breast cancer is lower compared to a woman.”
Dr Gie Hooi said a mammogram does not cause breast cancer, but helps detect it at a very early stage – even before a lump can be felt in the breast.
The consultant breast and oncoplastic surgeon also dismissed the myth that a lump in the breast necessarily means breast cancer, saying that not all lumps found in the breast are cancerous.
“Out of 10 women presented to the clinic with a breast lump, actually only one of them will be diagnosed with breast cancer. If you ever feel a lump in your breast, do not panic; go and see a doctor,” Dr Gie Hooi said.
“Usually what the doctor will do is a triple assessment. First, a clinical assessment – the doctor will ask questions to understand your risk profile, reproductive history, lifestyle, and family history of breast cancer to determine are you in the higher risk group of developing breast cancer.
“Then the doctor will perform a clinical examination to examine the breast. This will be followed by imaging, either a mammogram or ultrasound, then followed by a biopsy.
“These three assessments will allow us to derive at an accurate diagnosis of the nature of the lump.”
Dr Gie Hooi urged women to check their breasts every month and to go for a check-up if symptomatic, besides encouraging regular screening.