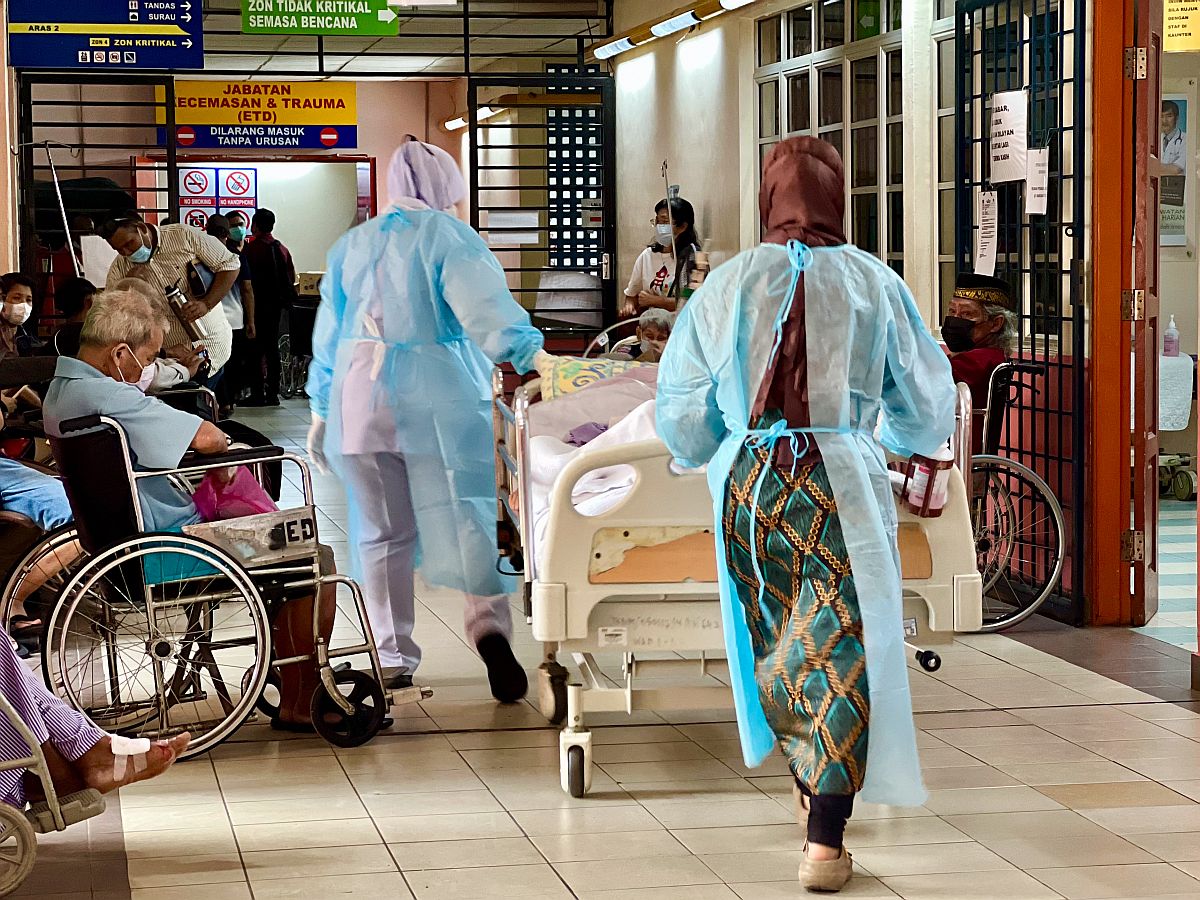
All health systems can only function with health care professionals (HCP). The attainment of the health component of the Sustainable Development Goals and Universal Health Coverage is dependent on the availability, accessibility, acceptability, and quality of HCP.
The health care workforce has a vital role in the ability of a health system to respond to natural or man-made disasters as well as related environmental, technological, and biological hazards and risks.
The consequences of the Covid-19 pandemic were devastating with Malaysia having the highest death rate per capita of the population in Asean. Not only that, the illnesses and disabilities from long Covid-19 have yet to be quantified.
Malaysians owe a mountain of debt to the sacrifices of the junior doctors who provided them care, whether in hospitals or clinics for Covid-19.
Junior doctors faced very challenging personal and professional conditions like long working hours in personal protective equipment (PPE), trying to protect themselves and their families from potential illness; having to adapt to new ways of working; and with training opportunities replaced by service provision and examination postponements.
The sacrifices of junior doctors were critical in containing the pandemic; some junior doctors even gave their lives for their fellow citizens.
Yet it appears that many people, particularly decision makers and politicians, have forgotten the critical contributions of the junior doctors during Malaysia’s worse public health disaster.
This memory lapse was reflected in the media reports of the Ministry of Health’s (MOH) management of the transfers of its junior doctors, in the past two months. Various unflattering adjectives have been used to describe the exercise, including “KKM treats its doctors like slaves”.
What A Mess
It is difficult to dispute that the transfer exercise and permanent appointments were a disgraceful mess that have included, among others:
- Lack of communication between Putrajaya and state health departments resulted in major hospitals, with heavy workloads, short of doctors with consequential disruption and/or suspension of health care service delivery, which were announced to the public. A doctors’ group estimated that the waiting times in emergency departments for admissions at major hospitals to increase by 50 to 100 per cent with all its attendant consequences for patients.
- There were also allegations that patient safety was compromised by the shortage of medical officers.
- Doctors were not eligible for transfer claims, which resulted in some having to pawn jewellery, withdraw from savings accounts etc. The financial loss incurred by doctors transferred to Sabah and Sarawak were particularly high.
- Doctors posted to Sabah and Sarawak were instructed to return to the Peninsula at short notice.
- Doctors posted to facilities which had no more vacancies for medical officers.
- Doctors posted to the new Dungun hospital which is still under construction.
- Disruption of specialty training for doctors preparing for or in the Masters specialisation training after they were transferred to other facilities, as their training necessitated them to be in specified facilities. Some appeals were rejected, while others were instructed subsequently to report back to the original facility.
- Issuance of transfer instructions on the weekend prior to reporting for duty.
- Not permitting mutual exchanges of postings.
The contract doctor issue has been around since 2016. Transfers and appointments to permanent positions are a norm in the Health Ministry. Yet, 2023 was the first occasion that such messiness came into the public domain.
Who was responsible for this mess? Was it poor communication, poor coordination, incompetence, irresponsibility, or a combination of these factors? Were there other factors?
Going Forward
The health care workforce, particularly junior doctors, have a critical role to play if the country is to achieve its health and developmental objectives in the next decades.
A paradigm shift has to be adopted with strategies to plan, educate, deploy, manage and reward the health care workforce, particularly junior doctors.
It is critical that urgent steps are taken to improve the working lives of junior doctors. This would include, among others, some of those listed below.
It is an immediate priority to address burnout which has been described by the World Health Organization (WHO) as “a syndrome conceptualised as resulting from chronic workplace stress that has not been successfully managed and characterised by three domains: feelings of energy depletion or exhaustion; increased mental distance from one’s job, or feelings of negativism or cynicism relating to one’s job; and reduced personal efficacy”.
Burnout is associated with adverse personal behaviours like drug misuse/ abuse, relationship breakdown, and consequential effects on patient care with doctors who suffer from burnout more likely to be involved in adverse patient incidents.
The fair financial compensation of junior doctors and specialists has been a long-standing issue. The on-call allowances of junior doctors per hour have been reported to be less than that of fast-food staff. The unkindest cut of all were reports of delays in payments of on-call allowances.
One wonders whether other civil servants are treated in this manner.
With the rising cost of living, accommodation etc the issue of financial compensation contributes to the poor morale of junior doctors.
Specialty training is through the Masters programmes of the local universities or the Royal Colleges examinations (also termed “parallel” pathway). Selection for the Masters programmes can be described as opaque, to say the least.
Some contract doctors, who have difficulties in entering the Masters programmes, have taken the parallel pathway examinations on their own.
However, there is no clear pathway for these contract doctors to be absorbed into permanent service as specialists. Many politicians who exhorted the Health Ministry to deploy more specialists into hospitals in their constituencies have, strangely, been silent about this administrative logjam.
The MOH’s response on August 4, 2023 was a general statement that did not address the impact of doctor shortages on patient safety and quality of care.
The MOH claimed that “through these new placements, officers will obtain more exposure about the health care system and can develop their own capacities. This experience will make officers more mature and empathetic, and tougher (berdaya tahan) in surviving their career as a public servant”.
Resilience is desirable of all junior doctors as they have substantial responsibility for patients’ lives and wellbeing, work long hours, encounter difficult situations and have to try to balance personal and professional challenges.
However, resilience is not an innate attribute in everyone. It often needs to be nurtured by various means like good physical and mental health, recognising and managing conflict situations in the workplace, and maintaining strong personal relationships, all of which would be enhanced by mentorship and other support mechanisms as well as resilience and leadership training programmes, which are sadly lacking in the Health Ministry.
The gratification from doing a good job is an important factor in keeping junior doctors resilient. Doctors who experience joy in work are happier, more secure, have greater job satisfaction, greater career fulfilment and consequently, provide higher quality and safer patient care, which is what the public wants.
Decision makers and management in the Health Ministry, as well as the general public, have to value junior doctors. Decision makers and management in the Health Ministry have to ensure that all HCPs have joy at work.
The goal of joy at work was stated succinctly by the institute for Healthcare Improvement (IHI): “The most joyful, productive, engaged staff feel both physically and psychologically safe, appreciate the meaning and purpose of their work, have some choice and control over their time, experience camaraderie with others at work, and perceive their work life to be fair and equitable.”
The politicians at the MOHy appear to have forgotten their individual and party’s promises prior to appointments to their current positions.
The current junior doctors’ mess has to be cleared up urgently. Is the Public Service Department (JPA) and the Health Ministry up to the task of doing so? Is there the political will and leadership to do so? Or will it be kicked down the road to the next government?
Only time will tell.

Dr Milton Lum is a Past President of the Federation of Private Medical Associations, Malaysia and the Malaysian Medical Association. This article is not intended to replace, dictate or define evaluation by a qualified doctor. The views expressed do not represent that of any organisation the writer is associated with.
- This is the personal opinion of the writer or publication and does not necessarily represent the views of CodeBlue.