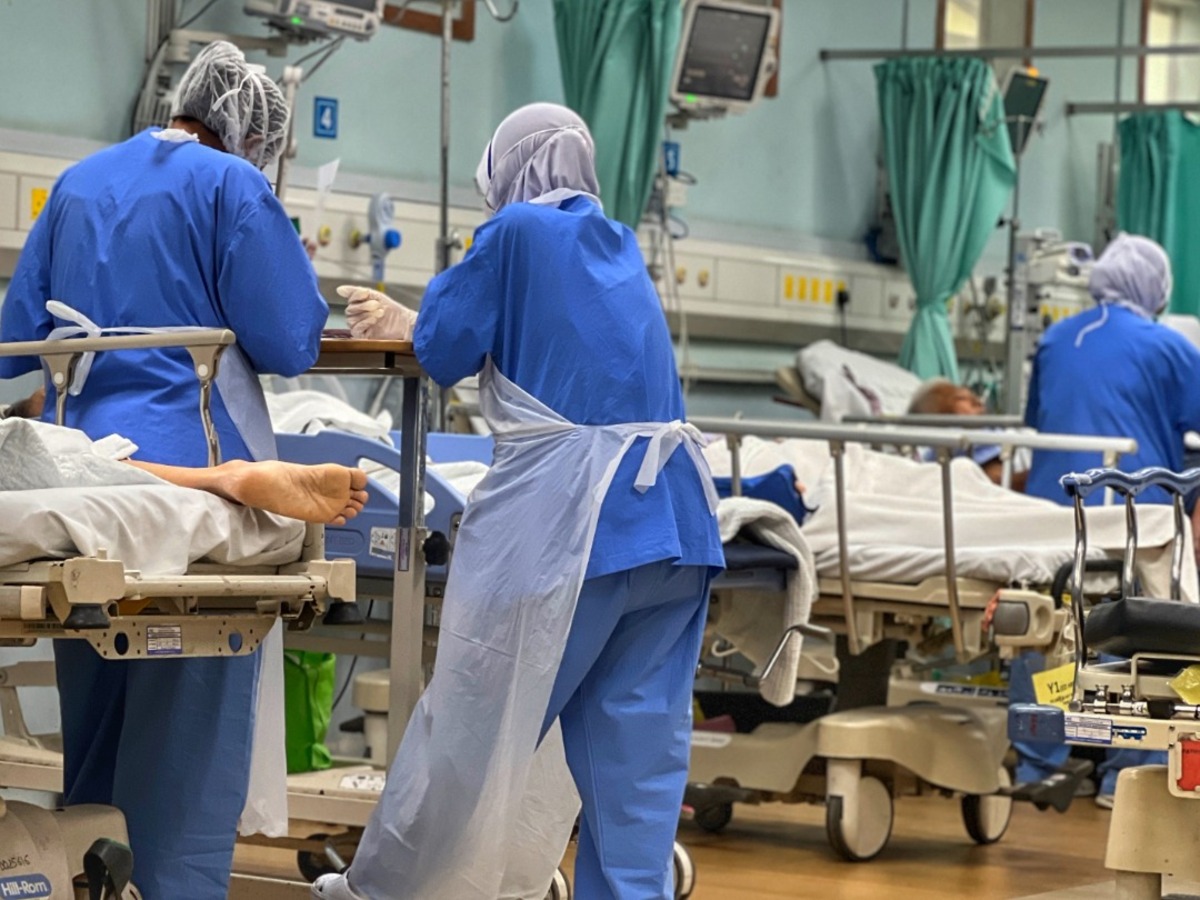
IPOH, Dec 16 – One of the reasons why doctors quit the public sector is guilt over the deaths of patients from bed shortages in hospitals despite their best efforts, a medical doctor said.
Dr Jamie (pseudonym) – who is based in Ipoh, Perak, and was formerly with the government health service – claimed that government doctors are punished for complaining to their superiors over the lack of resources in overcrowded public hospitals.
“They’re actually very concerned about patients,” Dr Jamie, who requested anonymity, told CodeBlue in a recent interview here.
“When a patient dies in casualty because there are not enough beds, the person who really dies inside is the doctor who looked after them because that doctor knows that this shouldn’t have happened. They have done their best.”
CodeBlue reported last Monday that critically ill patients, including ventilated cases, are stranded for up to six days in Raja Permaisuri Bainun Hospital’s (HRPB) emergency and trauma department – also known as casualty, ETD, or ED – for ward admission, due to insufficient critical care beds and doctors and nurses.
CodeBlue’s report on the severe congestion in the Ipoh general hospital’s ED documented two patients who died in general medical wards after waiting more than four days in the emergency department for admission. An HRPB medical officer said one of those patient deaths could have been prevented if she had been properly monitored or admitted early into the ward.
“Yes, the family has lost someone, but the doctor dies inside,” Dr Jamie said, without referencing any particular case. “Every time it happens, the doctor keeps dying inside. That is why staff become so demotivated – staff don’t want to do anything, they want to take a break. They quit because they can’t take it anymore emotionally.
“It’s not the work stress – they may be able to take the work stress – but they cannot take that the death is on their hands. Their hands are bloodstained with death.
“How are they going to explain to family members? One day, when everything comes out, who’s going to take responsibility? For the patients, the front is the doctor or nurse who’s looking after them.
“The admins are all staff behind – they’re not going to take the blame, they’re not going to take the shouting, they’re not going to take the guilt. For them, that’s only a number on paper; they don’t see the person behind it.
“This is why doctors choose to become e-hailers and earn a bit less – because they cannot take that guilt anymore.”
In CodeBlue’s report, an HRPB medical officer talked about difficult decisions that doctors have to make about selecting patients for admission into the intensive care unit (ICU) amid limited beds.
Government Doctors Face Repercussions For Complaints
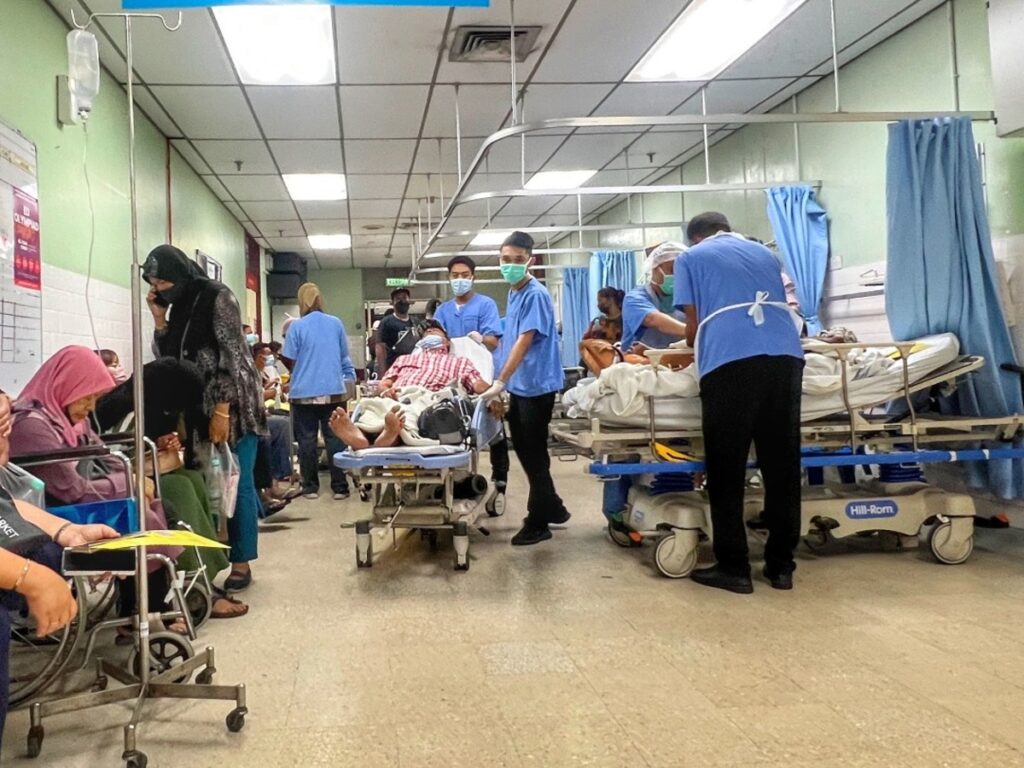
Dr Jamie said “everybody” sees the situation of overcrowded emergency rooms as a problem.
“But we have been heavily warned of repercussions that will happen if you’re the one reporting. They always say, ‘if you have a problem, report to us and we will take action’. But how many times do you go to the big bad wolf and complain, but only end up getting eaten in the end?” he said.
“We complain to the people who are marking our performance in the hospitals. I may have been the doctor who saved the maximum number of lives, but because I’m a ‘troublemaker’ – I keep going and saying, ‘we don’t have this, we don’t have that’ – they mark me down.
“I end up not progressing in my career because of that. We want to progress in our careers, what more contract doctors who are being marked for everything. There are a lot of people who want to voice out, so that’s why people end up writing anonymously and talking anonymously off the record.”
All four HRPB medical officers interviewed by CodeBlue about patients’ days’ long wait in the ED spoke on the condition of anonymity.
Contract issues are also another main driver of doctor resignations, Dr Jamie said, due to the lack of career pathways and even inability to get car loans, with renewals of short two-year contracts.
Dr Jamie said he personally knows a number of doctors, nurses, allied health workers, and medical assistants who quit the public sector after the Covid-19 pandemic struck in 2020.
He pointed out that many contract doctors were called into service during the Covid-19 pandemic after waiting ages for placements, but did not receive permanent posts when the acute phase of the pandemic subsided.
“During 2020, all those people who waited and waited and waited suddenly got called in. But when the pandemic became better, ‘thank you so much for your services, your time is up, bye’. So people have already learned from it – ‘Why should I go through that?’
“Even though the system has become better, a lot of people look at their seniors and say, ‘I don’t want that to happen to me’. So before that happens, they decide to call it quits.”
One of the HRPB medical officers who previously spoke to CodeBlue said housemen in the public tertiary hospital in Ipoh tend to quit, either midway training or immediately after completing housemanship. Another HRPB doctor spoke of feeling under-appreciated for their work, saying their hands are tied with limited resources.
Then-Health Minister Khairy Jamaluddin told Parliament last March that 2,032 contract medical officers resigned between 2017 and 2021; about 38 per cent of them (768 doctors) quit last year.
Develop Batu Gajah Hospital For Elderly
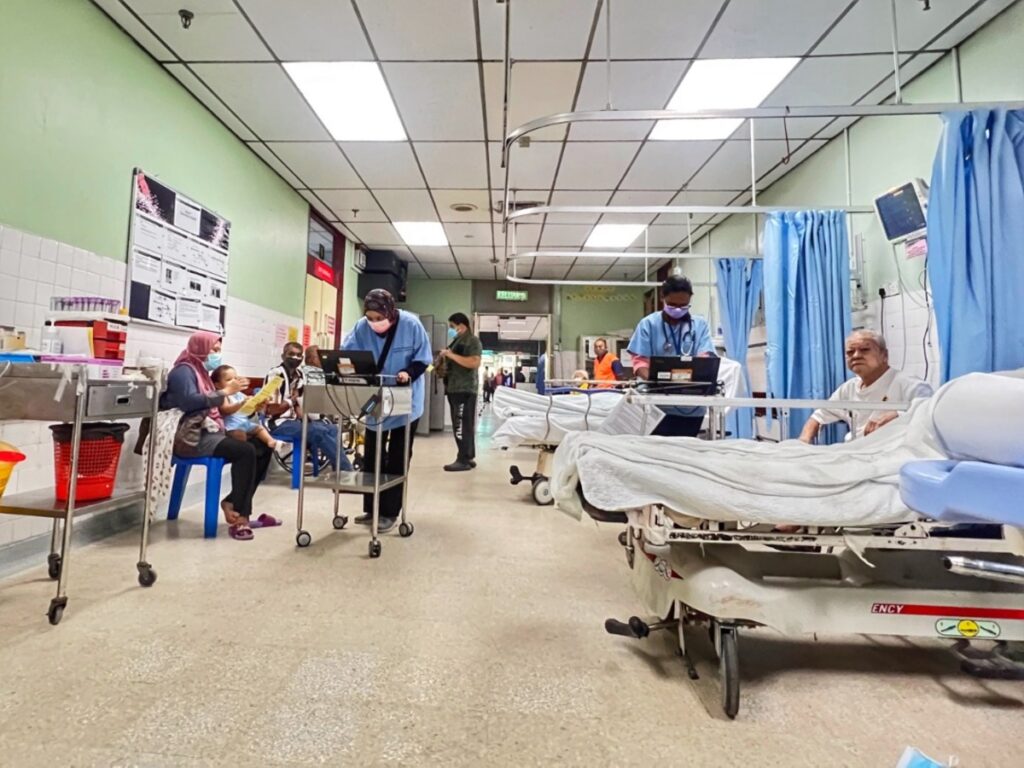
Dr Jamie also urged the government to expand old-age health care services for Batu Gajah Hospital to decongest HRPB, Perak’s main referral centre and tertiary hospital.
He pointed out that the public tertiary hospital in the state capital Ipoh – with just about 1,000 official beds – caters to a population of nearly 900,000 people.
According to Department of Statistics Malaysia (DOSM) population statistics, the Kinta administrative district in Perak recorded a population of 888,767 people in 2020.
“You’re trying to tell me that for every 900 people, there’s only one bed. And you’re talking about Ipoh – a city where people come to retire, people who are having comorbidities, people who are elderly, people who are at more risk of going to hospital.
“The odds are going to be higher, you’re talking maybe 1,800 people to one bed,” said Dr Jamie.
“Doctors have to start selecting patients – who they can admit and who they should discharge. That causes a legal concern because a doctor may be pressed to not admit a patient because of bed shortages.
“So it comes to picking and choosing, which is what medicine should not be. Everybody should get treatment as is.”
CodeBlue reported that most of the severely sick patients coming to HRPB’s emergency department are presenting with advanced non-communicable diseases (NCDs) — such as heart disease, kidney failure, and stroke — that worsened after the disruption of care from two years of Covid lockdowns.
Dr Jamie suggested that Batu Gajah Hospital, which is a secondary hospital, be expanded and developed with health care services from doctors, nurses, physiotherapists, and allied health care workers for the elderly community.
“Batu Gajah has a very high rate of elderly people — people who were born there and migrated off now come back to Batu Gajah to spend the remainder of their days there. So why not have old-age facilities, geriatric facilities there?”
Batu Gajah Hospital is some 15 to 20 minutes from Ipoh. Perak has the oldest population in the country. The state constituency of Pasir Pinji in the state capital city of Ipoh has one of the highest old-age dependency ratios in Malaysia.
Dr Jamie cited other towns like Simpang Pulai, Meru, and Jelapang with plenty of government land where public hospitals can be built, as well as universities that could construct hospitals.
“Ipoh is going to be a geriatric age city. We need enough facilities. I’m not even going into geriatric facilities yet; I’m talking about basic facilities so that people can get access to health care.”