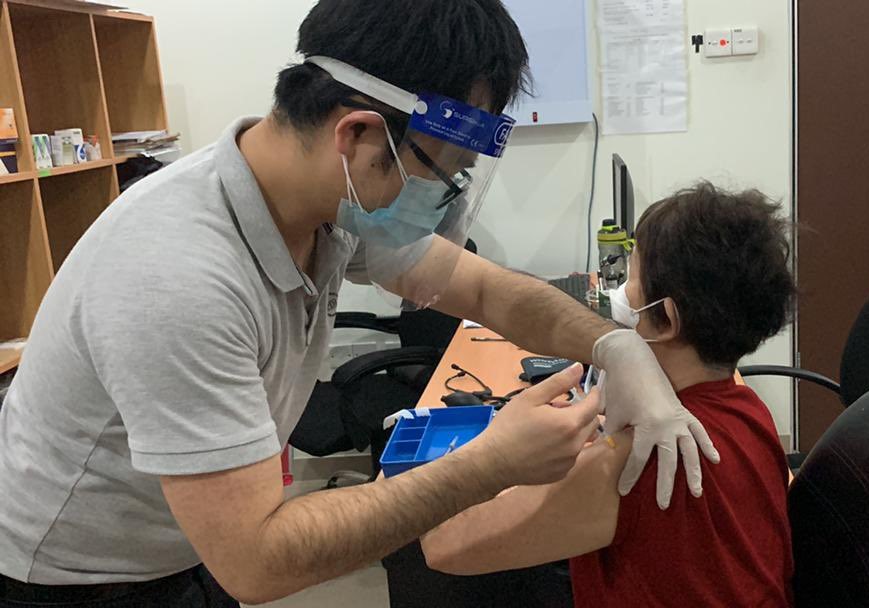
2021 was annus horribilis for Malaysia with Covid-19 dominating the year and the floods providing the finale for the year.
Covid-19 was the worst public health disaster in Malaysia. It will dominate 2022 just as in 2021, with 31,026 recorded deaths and 2,707,402 recorded cases on December 16, 2021. There were more than 23,000 deaths from June to September 2021 with the health care system on the verge of collapse then.
In comparison, there were 429 recorded deaths and 87,913 recorded cases on December 16, 2020, an increase of 7,232 per cent and 3,079 per cent respectively. No one could have imagined then the scale of the increase.
Thankfully, with widespread vaccination and the Greater Klang Valley Special Task Force (now renamed National Rapid Response Task Force), the dire situation in the Klang Valley was brought under some measure of control.
The finale to 2021 was the widespread floods with numerous lives lost and thousands made homeless, the human and financial costs of which have yet to be determined.
Both Covid-19 and the floods exposed numerous examples of irresponsibility and incompetence, which were underpinned by arrogance, lust for power and lack of insight.
The public’s humanitarian response in both events put many in authority to shame. There will be more of the same in 2022 if there is no sea-change in attitudes.
More Covid-19 Cases and Deaths
The Omicron variant is a reminder that the world is still not out of the woods. Its surges in South Africa, the United Kingdom, Europe and the United States will soon affect the rest of the world. The question about Omicron is not whether it will spread in Malaysia but when, and its scale and impact on the health care system.
Clinical data on Omicron is still emerging. Its numerous mutations enable it to spread more rapidly than the Delta variant and to escape the protective effect of current vaccines. Covid-19’s rate of spread has increased with new variants, i.e. Omicron more than Delta, which was more than Alpha, Beta and the wild variants.
A vaccine booster is necessary to restore antibody levels which wane with time. Even then, the protective effect is less than with that of the Delta and wild variants.
Emerging data indicate that children are also affected with increased hospitalisations reported globally. This is of particular importance as vaccines for the 5-11 age group are only expected to arrive in Malaysia at the end of the second quarter 2022.
Other Covid-19 variants are likely to arise in 2022, with its impact(s) on health care yet to be discovered. Will Omicron and other bizarre variants (hopefully not) overwhelm the Malaysian health care system in 2022? Only time will tell.
The only thing predictable about Covid-19 is its unpredictability.
Omicron is looking for the unvaccinated. They are at increased risk of Covid-19 compared to the fully vaccinated. The definition of fully vaccinated will change to one that does not depend on the number of doses.
However, the vulnerability of Malaysians remains with a 3 to 4 in 10 at risk of severe disease, i.e. males, age above 60 years, high blood pressure, diabetes, cardiac disease, chronic renal disease, asthma, obesity, and chronic pulmonary disease. Although the vulnerable and deprived will be disproportionately affected, it is disturbing that there has been no concerted attempt to address these risk factors.
Long Covid will have an impact on health care delivery, the scale of which is unpredictable.
Migrant workers will remain an Achilles heel. Most have received two vaccine doses. However, overcrowding, which is one of the root causes of viral spread, has not been adequately addressed, despite the Minimum Standards of Housing and Amenities Act (Amended 2019), with 17,457 out of 37,662 (47.15 per cent) peninsular employers found to be non-complaint with the law in inspections carried out between January 11, 2021 and November 30, 2021. What about the uninspected accommodations? Is there any sense of urgency?
The metrics of Covid-19 will shift from the current ones to more utilitarian metrics, for example hospitalisations, severe disease and deaths and their risk factors; testing, contact tracing and treatment capacities; compliance with ventilation guidelines, physical distancing and mask mandates, and the scale of Long Covid etc.
Basics Remain with Variations
Individual and shared responsibilities in controlling Covid-19 will remain, but there will be variation with new knowledge in 2022. The former includes physical distancing, face masking, frequent handwashing, and avoiding crowds, confined spaces and close contacts.
The latter includes testing, contact tracing, isolation / quarantine, treatment, vaccination, and appropriate risk communication.
There will be more rapid and extensive testing, more effective treatments and vaccines; and hopefully, prevention of spread with vaccination.
However, vaccines will not end the pandemic. It is probable that regular vaccination will be necessary. Israel is rolling out the fourth dose for those above 60 years and those at risk like health care staff. Will the rest of the world follow Israel in rolling out another booster for the general population? And the fifth dose or variant-specific vaccines?
The scale of surges will increase if the public health response is inadequate and/or the public do not comply with their individual responsibilities and vaccination appointments.
Pandemic fatigue will be aggravated by poorly considered measures, like the deferred amendments to the Prevention and Control of Infectious Diseases Act.
Non-Covid Diseases
The incidence of non-communicable diseases (“NCD”) will continue to rise with increasing undiagnosed and uncontrolled numbers because there is no coordinated effort to control it, with its consequent impact on Covid-19 incidence.
Other communicable diseases, for example dengue, diphtheria, and rabies, will continue to take its toll.
Backlogged surgeries and treatments for NCDs will lead to premature and excess morbidity and mortality. Another Covid-19 surge will further aggravate the situation.
Public Trust and Health Policies
Health care will be increasingly provided by non-health sectors with technological tools, for example internet purchases of pharmaceuticals and medical devices.
The Health Ministry’s budgetary allocations cannot assure improved patient safety and quality care unless wastages, inefficiencies and the role of middlemen are reduced markedly; and there is an open and just culture within the ministry.
As long as health policies are formulated without genuine consultation with stakeholders, success will be limited or absent.
Public trust will continue to wane for various reasons that include poor risk communication; non-compliance to Covid-19 standard operating procedures (“SOPs”); failure of authorities to engage meaningfully with the private sector, universities and civil society; misuse and abuse of social media; lack of transparency; and poorly considered measures. This will be so particularly when cases and deaths persist.
Vaccine hesitancy will persist as long as civil society and non-governmental organisations are not actively involved in the messaging of its benefits.
At a tipping point, the pressure for change will be unstoppable and the government of the day will have to oblige.
Increasing Health Care Expenditure
Health care expenditure will continue to rise because of the ageing population; NCDs; Covid-19; other infectious diseases; new technologies; increasing patient demands; and the unrestrained middlemen in health care.
Increasing out-of-pocket expenditures in the private and public sectors will lead to more families facing financial ruin if they or their relatives get catastrophic diseases, for example cancer heart attack, Covid-19; or are made redundant.
Medical inflation will continue to rise unabated.
More general practitioner (“GP”) clinics and even private hospitals will close because of financial unsustainability and physician burnout.
Medical Workforce
Medical unemployment and disgruntlement will continue with the issue of contract doctors yet to be adequately addressed, more than five years after the first contracts were first issued.
It is apparent that decision makers, in the government and the civil service, have yet to fully appreciate the contributions of contract doctors in the management of Covid-19 at all levels. When the blood, sweat, and tears of the contract doctors in the public sector are met with an uncaring governmental response, it raises the fundamental question about the value systems in the government and civil service.
Another junior doctors’ hartal cannot be ruled out.
The best and brightest graduate doctors will seek employment abroad with Malaysia one of the few countries that train them, at public expense, for other countries.
There will be mergers, acquisitions, and closures of some private medical schools.
General practitioners’ minimal or non-involvement in management of Covid-19 and NCDs in public sector patients will impact negatively on population health and the risk of Covid -9 and other infections.
Medical Technologies
New technologies, for example portable diagnostics, smart drug delivery mechanisms, genome sequencing, machine learning, artificial intelligence etc will impact more on health care.
Issues of patients’ confidentiality and security; patient safety; and the successes and failures of the new technologies will be problematic.
New technologies are just tools. Whether it adds to or detracts from humane health care has to do with how and why it is used. Discrimination and careful evaluation are essential and not technological exuberance.
Stay Healthy and Stay Safe
Health care is avoided by staying healthy. A healthy diet, maintaining an appropriate weight, regular exercise, sufficient rest, safe sexual practices, avoiding smoking, moderate alcohol consumption, and keeping vaccinations current are necessary. This requires effort, smart lifestyle choices and the occasional medical check-up.
Covid-19 risks can be minimised by compliance with one’s individual responsibilities and vaccination.
Wishing all readers good health in 2022. Remember — rakyat jaga rakyat. Take care and stay safe.

Dr Milton Lum is a Past President of the Federation of Private Medical Associations, Malaysia and the Malaysian Medical Association. This article is not intended to replace, dictate or define evaluation by a qualified doctor. The views expressed do not represent that of any organisation the writer is associated with.
- This is the personal opinion of the writer or publication and does not necessarily represent the views of CodeBlue.