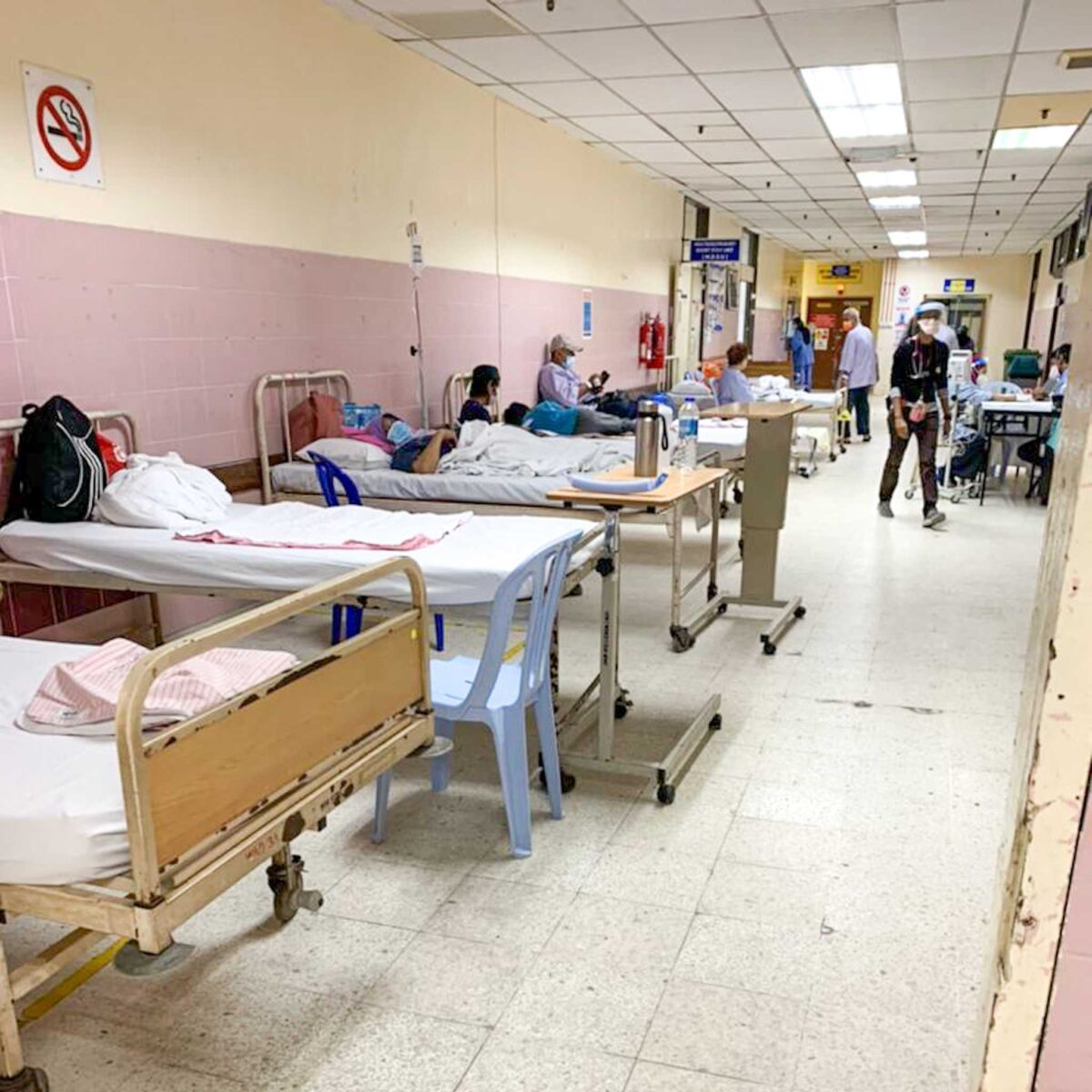
KUALA LUMPUR, July 7 — Contrary to authorities’ assertions that things are under control, anecdotal reports paint an unfolding nightmare of Klang Valley hospitals buckling under a vicious Covid-19 surge, akin to India’s crisis at the height of its epidemic.
Health care workers described scenes of patients lying on the floor due to full beds, converting wards or entire floors into Covid-19 treatment areas, and stacking bodies on trolleys to quickly clear victims’ beds for new admissions.
Bed turnover now is not routinely from discharge after recovery, but after death.
Multiple hospitals across Selangor and Kuala Lumpur are struggling to cope with an increased admission of critically ill Covid-19 patients requiring oxygen in the past two weeks.
Hundreds of severely ill Covid-19 patients are being transferred each day to two of the country’s designated coronavirus hospitals, Sungai Buloh Hospital and Ampang Hospital, as patients at low-risk quarantine centres and those under home surveillance quickly deteriorate.
“We don’t really know what’s causing this,” a medical officer at Hospital Ampang told CodeBlue on condition of anonymity. “All we know is that these patients are in healthy condition one day, and they have breathing difficulties the next.”
On Sunday, the hospital received about 100 Stage Four Covid-19 patients from MAEPS (Malaysia Agro Exposition Park Serdang), according to the medical staff. The next day, it admitted another 120 severe cases from the same Covid-19 quarantine centre.
“It’s like trying to empty the ocean with a thimble.”
Anonymous medical officer at Ampang Hospital
“Admissions are high but discharges are low. And that is not inclusive of critical patients under pre-hospital care and ambulance calls or those who walked in,” the Ampang Hospital doctor said. “We accept them, but we don’t know what to do with them.”
In the past two weeks from June 22 to July 5, Kuala Lumpur and Selangor continued to record one of the highest Covid-19 incidence rates in Malaysia, after Labuan and Negeri Sembilan.
Kuala Lumpur’s incidence rate stood at 556.74 per 100,000 people, more than double the national incidence rate of 256.94 per 100,000 population, while Selangor had an incidence rate of 502.03 cases per 100,000 people.
In other words, the Klang Valley found about five Covid-19 cases in every 1,000 people in the past 14 days. Using incidence rates enables equal comparison across states with different population sizes.
Covid-19 death rates in Kuala Lumpur and Selangor were also among the top after Labuan and Negeri Sembilan, with Kuala Lumpur reporting 80.61 deaths per million population in the past fortnight — 2.4 times higher than the national rate of 33.55. Selangor’s death rate over the same period amounted to 67.13 per million population.
This is despite efforts to boost vaccination rates throughout the country. Kuala Lumpur’s high incidence and death rates do not seem to correspond with the federal territory’s high vaccination rate, amid the spread of the highly transmissible Delta variant, though one explanation could be that it takes time for protection from vaccines to kick in.
As of July 4, Kuala Lumpur had 85.6 per cent of its adult population who have received at least one dose, while 18.1 per cent of its adult population have been fully vaccinated. Selangor’s vaccination rate remains the slowest among states, with only 7.3 per cent of its adult population fully vaccinated. About 23.1 per cent, however, have received at least one dose.
Just Like India
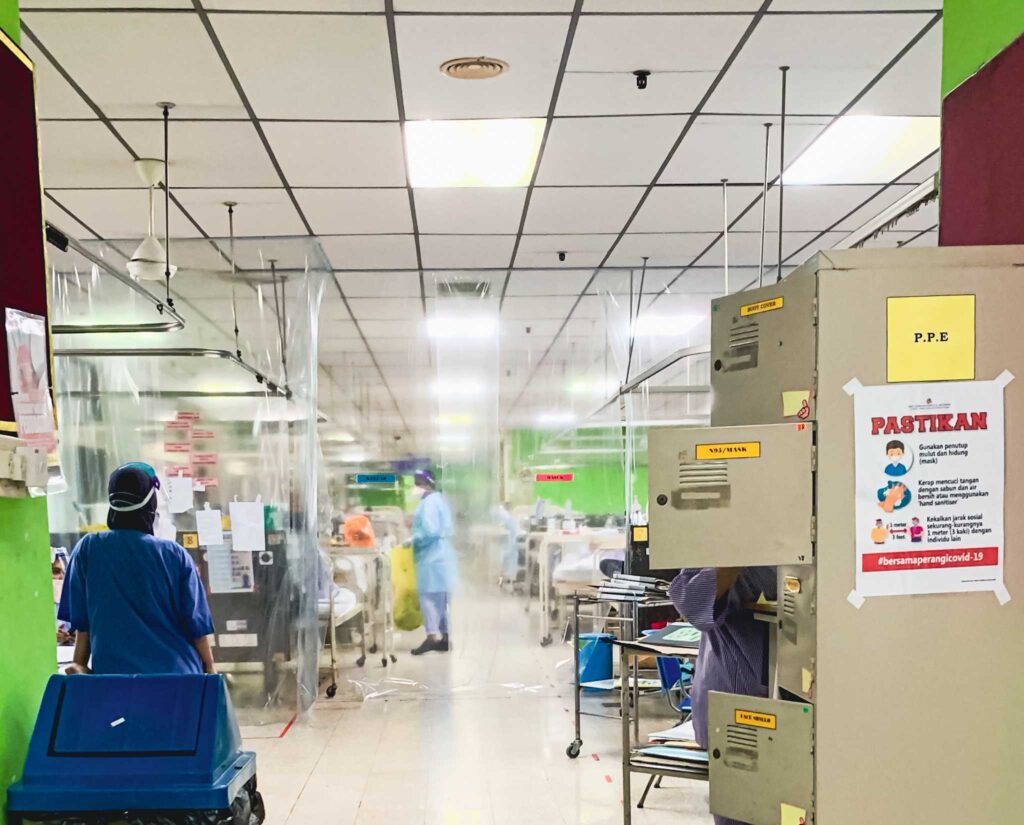
Similar scenes — overflowing wards, overworked medical officers, harried housemen and grieving families — are also transpiring in Covid-19 hybrid hospitals such as Hospital Kuala Lumpur (HKL), Hospital Selayang, and Hospital Tengku Ampuan Rahimah (HTAR) Klang.
Across the Klang Valley, hospitals are struggling to make more beds available for both Covid-19 and non-Covid patients. In a bid to tackle the shortage of beds, HTAR has converted its orthopaedic, surgical, and medical wards into Covid wards, based on an individual account.
“Covid-19 patients who require oxygen supplementation, like a nasal prong or high flow mask, and those who do not require one, will be placed in the Covid ward. Those in a more serious condition will be in intensive care units (ICUs),” one staff member at HTAR told CodeBlue.
“But don’t forget we still have non-Covid patients who require admission, so where do they go? They are at the emergency department. Some have to lie down in front of the payment counter because we’ve run out of clean wards,” the person said.
“The whole scenario is like India — patients are lying on the floor everywhere.”
Anonymous staff member at Hospital Tengku Ampuan Rahimah (HTAR) Klang
India’s deadly surge in coronavirus infections that began in mid-March had pushed the country’s health care system to the brink of collapse as patients were seen dying in parking lots and ambulances outside hospitals and overwhelmed crematoriums.
Hospitals had to turn away patients and beg for more oxygen, as families pleaded for beds and medicine. Across the country, hospital lobbies had been turned into wards.
In the Klang Valley, oxygen supply remains stable, though health care workers warn that if cases continue to dramatically spike, hospitals will quickly run out of beds and oxygen supplies.
At Selayang Hospital — where referrals from Kuala Kubu Baru, Sungai Buloh, Ampang, and as far as Shah Alam and Klang are being admitted — stretcher beds are being deployed next to hospital beds as patients continue to stream into its emergency unit.
Total hospital admissions at the Selayang facility increased by 150 per cent in the past two weeks, according to a medical staff who had worked up to 20 hours a day on an extended shift that ran as late as 1am. The next working shift began at 5am.
Negative To Positive
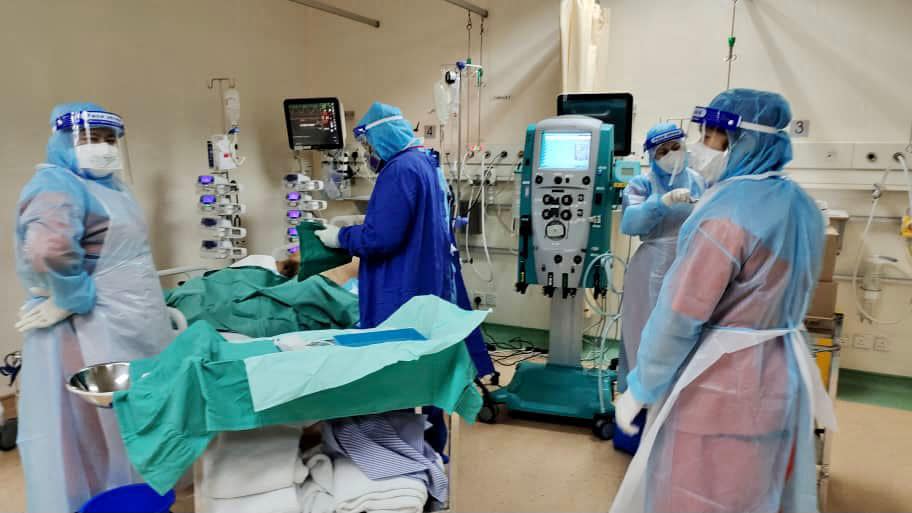
Apart from new Covid-19 admissions, hospitals are now reporting an increased number of non-Covid patients who are catching the virus in hospitals.
“That’s another issue that we are facing,” said a Selayang Hospital staff member.
“Patients are popping up positive (for Covid-19) in the ward from out of nowhere. It’s literally like stepping into a land mine.”
Anonymous staff member at Selayang Hospital
“It’s frustrating,” the person said. “When it happens, you have to lock down the cubicles, lock down the wards, swab everyone and suddenly, out of nowhere, you are also positive.”
“It’s a frustrating situation because it’s a lot of work.”
Respiratory droplets and close contact were previously considered to be the primary modes of infection for Covid-19. However, both the World Health Organization (WHO) and the United States’ Centers for Disease Control and Prevention (CDC) have since recognised aerosol as a key mode of spread; in other words, the virus is airborne.
One study published by the CDC, based on experiments conducted across several laboratories, found that the virus can linger in aerosol form for up to 16 hours — leading to calls for natural ventilation and improved indoor air quality to reduce the risk of Covid-19.
Recently, a government audit in Victoria, Australia, sighted by ABC found that nearly 50 per cent of hospital isolation rooms in the state failed to meet ventilation guidelines.
Last year, over 4,000 hospital workers in Victoria were infected with Covid-19. And 11 per cent of all hospitalised Covid patients in Victoria contracted the illness in hospital, according to the Victorian Department of Health.
In Wales, local media reported that nearly a quarter of people who have died from Covid-19 in the country were infected in hospital. To date, Wales has recorded a total of 5,575 deaths.
At UKM’s Canselor Tuanku Muhriz Hospital (HCTM), where admissions reach 100 per cent capacity every day, more wards are being converted into either Covid wards or wards for persons under investigation (PUI) or severe acute respiratory infection (SARI) as new infections crop up.
“It’s getting quite crazy now, it wasn’t as bad before. Just imagine, we converted an entire level (level 7) into a Covid floor. After that, half of our surgical floor on level 5 was converted to Covid when more of our surgical patients became positive.
“Now, one of our three obstetric and gynaecology wards is also a Covid ward. So, every department is now facing that scenario,” according to one junior doctor at the hospital.
All Systems Down

Amid the chaos, it comes as a shock that places like Selayang Hospital are currently operating manually, due to a system malfunction that dates back to January.
“There’s a lot of paperwork involved, and we are doing it manually,” said a Selayang Hospital staff member.
“Back when we previously had a fully computerised system, we had everything ordered and traceable via a functional system. But right now, everything is manual so blood samples get lost, it’s not received by the lab, and results sent out are not received by the ward.”
Anonymous staff member at Selayang Hospital
“It’s a system malfunction since January, and it has never been fixed. It’s a Covid-19 situation with admissions at 150 per cent and blood tests are missing,” said the Selayang Hospital staff member. “And this is you poking the patient for the umpteenth time for the umpteenth result.”
The hospital’s top management did not immediately respond to CodeBlue’s request for comment on the matter.
Stacking The Dead
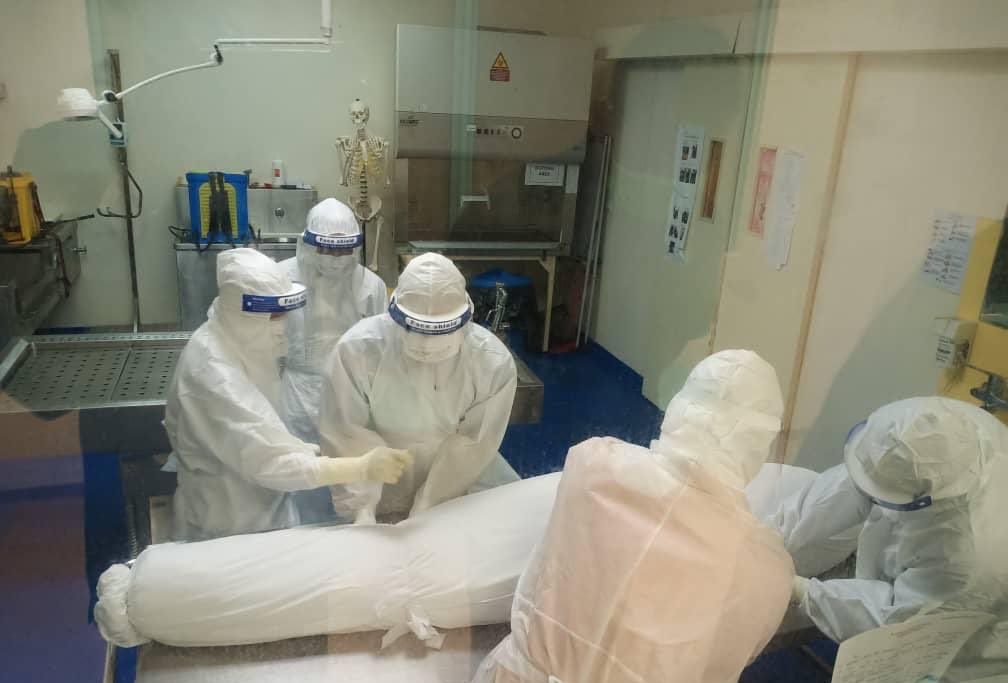
With new patients arriving and doctors working non-stop, Klang Valley hospitals seem to be having a catastrophic knock-on effect. Many are reporting a higher number of single-day deaths.
“We can clear out a whole cubicle of 10 (critically ill coronavirus patients) in a day,” according to a frontline medical worker at a government hospital in Selangor.
In the same hospital, bodies are being piled up on a trolley between each trip from the ICU to the mortuary to cope with the high amount of daily deaths.
“At one point, the mortuary worker had to — because he was working alone — stack one patient over the other to keep up with the deaths that are going on in the ward because you have to clear up the beds, so that new admissions can come in faster.”
Anonymous frontline medical worker at a government hospital in Selangor
“And in the Covid ward, when patients die, there is this whole process of terminal cleaning which includes sanitisation of the bed and all other procedures.
“So, to keep up with the turnover, there was a point where the mortuary came in and put three bodies on the trolley and pushed them to the morgues. Then, they came back to stack three more that whole night. So, the turnover is really bad,” the medic told CodeBlue.
“Even today (Monday), I had two Covid deaths. It’s a lot. And signing a burial permit now has become a routine that you just know what to fill in.”
A Bleak Future

Weary frontline health workers — the bulk of whom comprise contract medical doctors — have been pleading desperately for help as Covid-19 patients continue to overwhelm emergency rooms and ICUs, doubling the patient load on hospital staff who did not contract the virus.
A contract doctor at the MAEPS quarantine facility in Serdang previously wrote to CodeBlue that seven medical officers had active Covid-19 infections as of Monday.
“If everyone would just sit down and come up with a system, life would become so much easier for all of us. Standardise the standard protocol, and keep everyone informed on what kind of system we should have for all these hospitals,” one junior doctor said.
“If everyone just sits down and has a standardised system on how we are going to admit patients, how do we decide when a ward closes or opens, what kind of patients are we going to screen, what is the standard protocol to screen a patient, maybe life could get a bit easier.
“I don’t know, maybe it’s wishful thinking, but it’s frustrating when there is no system.”
Anonymous junior doctor
Over the weekend, the government announced plans to increase bed capacity and manpower, as well as outsource non-Covid-19 patients to private hospitals, in order to mitigate the rush of Covid-19 patients in Categories Three to Five into the public health care system.
Health Minister Dr Adham Baba acknowledged that total bed capacity in the Klang Valley has reached over 85 per cent, and an increase in hospital beds is needed.
Citing HKL as an example, he said HKL’s emergency and trauma unit receives between 60 and 70 Covid-19 patients per day, with an average of three patients in Categories Four and Five requiring oxygen supplementation. Patients in Category Five require ICU treatment.
Health workers from certain states will also be mobilised to support government hospitals and university teaching hospitals in need of additional manpower in treating Covid-19 patients.
“Final-year nursing students under the ministry’s trainee institutes undergoing practical training at vaccination centres (PPVs) will be optimised. Experienced nurses previously assigned to PPVs will be reassigned to support hospitals under the ministry,” Dr Adham said Sunday.
While plans are being carried out, doctors and nurses reeling from burnout as they face yet another, more infectious wave of Covid-19.
“It’s a multifactorial issue that just adds up to the stress. We are all burning out and I’ve had friends saying ‘I’m burnt out and I come to work crying because I’m just so tired’,” said a junior doctor. “This is why many of us are spirited to join the Hartal movement.”
“No one should have that thought of quitting on the first day of work,” another contract doctor said. “The current system doesn’t just enable that thought, but it encourages it because the system is in overload and nobody bothers to look at it and provide a solution to it.
“Policymakers are failing and systems are collapsing. Hospitals are going down the drain, doctors are exhausted. We are working 100 hours a week. Who’s taking care of us? Nobody is.”
CodeBlue attempted to contact the top management of all hospitals cited in the article. With the exception of HKL that issued a statement July 3 in response to viral images of patients lying on the floor in the facility — just to state that oxygen supply sufficed and that beds are managed according to need — other facilities have not responded at the time of writing.
CodeBlue spoke to five medical staff — one each at Ampang Hospital, HTAR, and Selayang Hospital, and two from HCTM.
Correction: CodeBlue amended the 11th paragraph under the “Negative To Positive” section to state that admissions at HCTM reach 100 per cent capacity every day. CodeBlue erroneously reported earlier that admissions at HCTM were up by 120 per cent. The error has been corrected.