The controversial Waktu Bekerja Berlainan (WBB) pilot project is no more. After weeks of public outcry and vehement dissent from health care workers, the Ministry of Health has officially pulled the plug.
The initiative, touted as a novel solution by the health minister, has been consigned to the scrap heap of ill-conceived policy experiments.
For many, the decision to cancel WBB represents a victory for grassroots advocacy — a testament to the power of collective resistance against policies that fail to consider realities on the ground.
Yet, the deeper question remains: what happens now? With the government forming yet another committee to address Malaysia’s long-standing health care crisis, the stakes are higher than ever.
The Real Crisis: Acknowledging Overwork And Underpay
At the heart of Malaysia’s health care woes lies a truth too glaring to ignore: health care workers are the backbone of the system. Without them, there is no health care.
Yet they remain overworked and underpaid, caught in a web of systemic neglect.
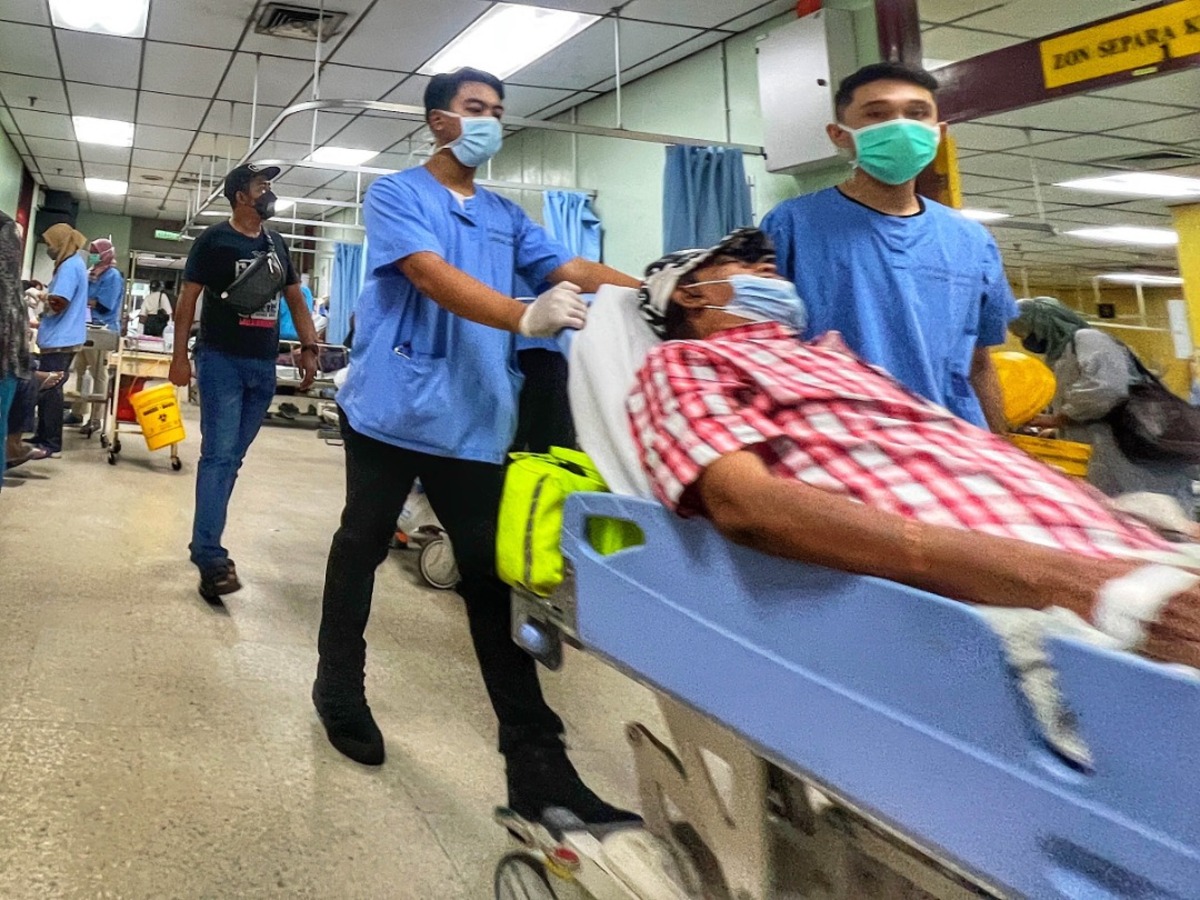
Public hospitals and clinics handle an estimated 70 per cent of the nation’s patient load. With the rise of non-communicable diseases, an aging population, and increasing medical complexity, the burden has reached unsustainable levels.
Overwork is not just a problem — it’s a crisis. Recognising this reality is the first step toward meaningful reform.
The Capacity Conundrum
Addressing overwork requires scaling up infrastructure and manpower. Malaysia’s health care facilities are woefully ill-equipped to handle the rising tide of chronic illnesses.
For example, patients with suspected colorectal cancer face weeks, even months, of delay for diagnostic scopes due to a shortage of gastroenterologists and endoscopic equipment.
Breast cancer screenings are similarly constrained, leaving many undiagnosed until it is too late.
Cancer isn’t waiting, and neither are other diseases. Obesity-related complications, diabetes, and heart conditions are silently adding to the load.
Strengthening primary prevention — starting with healthier school meals and banning sugary, calorie-dense options from hospital cafeterias — must be a national priority. Prevention saves lives and money, shifting the system away from its illness-driven model.
Fixing Retention: A Matter Of Respect And Security
One of the largest contributors to the exodus of health care professionals is job insecurity. Malaysia’s doctors are frustrated by opaque processes for promotions, erratic job placements, and unclear paths to specialisation.
The creation of an independent Health Service Commission could revolutionize workforce management, replacing the current rigid civil service structure with a responsive, health care-focused approach.
The arbitrary nature of job placements for Malaysian doctors are also a source of great frustration. Many doctors find themselves assigned to roles or locations that fail to align with their interests, training, or career goals.
For instance, a doctor deeply passionate about hospital-based acute care may find themselves placed in a primary care clinic in another state, while a doctor aspiring to build a career in community medicine is assigned to a hospital ward.
Such mismatches not only demoralise doctors but also result in suboptimal use of their skills, ultimately affecting patient care.
To address this, Malaysia could adopt a system inspired by the National Resident Matching Program (NRMP) used in the United States. The NRMP leverages advanced algorithms to match doctors with training programs, balancing individual preferences with institutional and regional needs.
Adapting such a model for Malaysia’s health care workforce could ensure fair, data-driven placements that better satisfy both doctors and health care facilities.
Clear promotion criteria and a merit-based system would also restore faith in the system. When health care workers feel valued and supported, they are far more likely to stay.
The National Curriculum for specialty training offers a valuable framework. Each specialty pathway clearly outlines the competencies, qualifications, and benchmarks required for progression, leaving little room for ambiguity.
For instance, entry into specialty training should be tied to well-defined assessments based on the National Curriculum’s blueprint. These include clinical skills, research contributions, and leadership experience, allowing candidates to demonstrate their readiness for higher responsibilities.
By increasing transparency in promotions and providing a structured pathway from entry-level positions to specialised roles, the health care system can address one of its most pressing retention challenges: doctors’ perceived job insecurity.
Paying Doctors What They’re Worth
On-call allowances have not been updated in over a decade, and doctors’ wages fail to keep pace with inflation. The narrative that doctors are overpaid ignores the reality of their academic and professional sacrifices.
Around the world, doctors are respected as knowledge workers of the highest order, with salaries to match. Malaysia must follow suit, not only to retain talent but to reflect the essential role these professionals play in society.
This is not a matter of entitlement — it’s a matter of survival for the health care system. A demoralised workforce cannot provide the care the nation needs.
Building A Culture of Respect And Wellbeing
Workplace culture needs urgent attention. Reports of sexual harassment, verbal abuse, and a lack of mental health support paint a grim picture. Hospitals must prioritize occupational health, create mechanisms to report grievances, and foster a culture of respect.
Recognising and rewarding excellence — whether it’s naming a “Nurse of the Month” or celebrating departmental achievements — can go a long way in boosting morale.
Team-building activities, family days, and mental health programs should become standard practice. Suicide prevention initiatives and stress management workshops are not luxuries — they are necessities in a high-stakes environment like health care.
A Time For Courage
Some reforms will require funding, but many demand something even more elusive: political courage. Reallocating budgets from inefficiencies to innovation is critical.
The Ministry of Finance must weigh the cost of continuing with an antiquated, crumbling system against the potential of a modern, agile health care infrastructure.
Malaysia stands at a crossroads. The collapse of WBB is not just the end of a failed policy — it’s an opportunity for a fresh start.
With visionary leadership, innovative solutions, and a renewed commitment to those who carry the system on their shoulders, the nation can build a health care system that not only survives but thrives.
The time for incremental changes has passed. Bold action is needed now, for the wellbeing of both the health care workers and the patients they serve.
The author is a doctor at a public hospital in the Klang Valley. CodeBlue is giving the author anonymity as civil servants are prohibited from writing to the press.
- This is the personal opinion of the writer or publication and does not necessarily represent the views of CodeBlue.