KUALA LUMPUR, August 30 – Over half a million teenage girls in Malaysian secondary schools are estimated to have missed their human papillomavirus (HPV) jabs due to school closures during the pandemic and diversion of funding to Covid programmes.
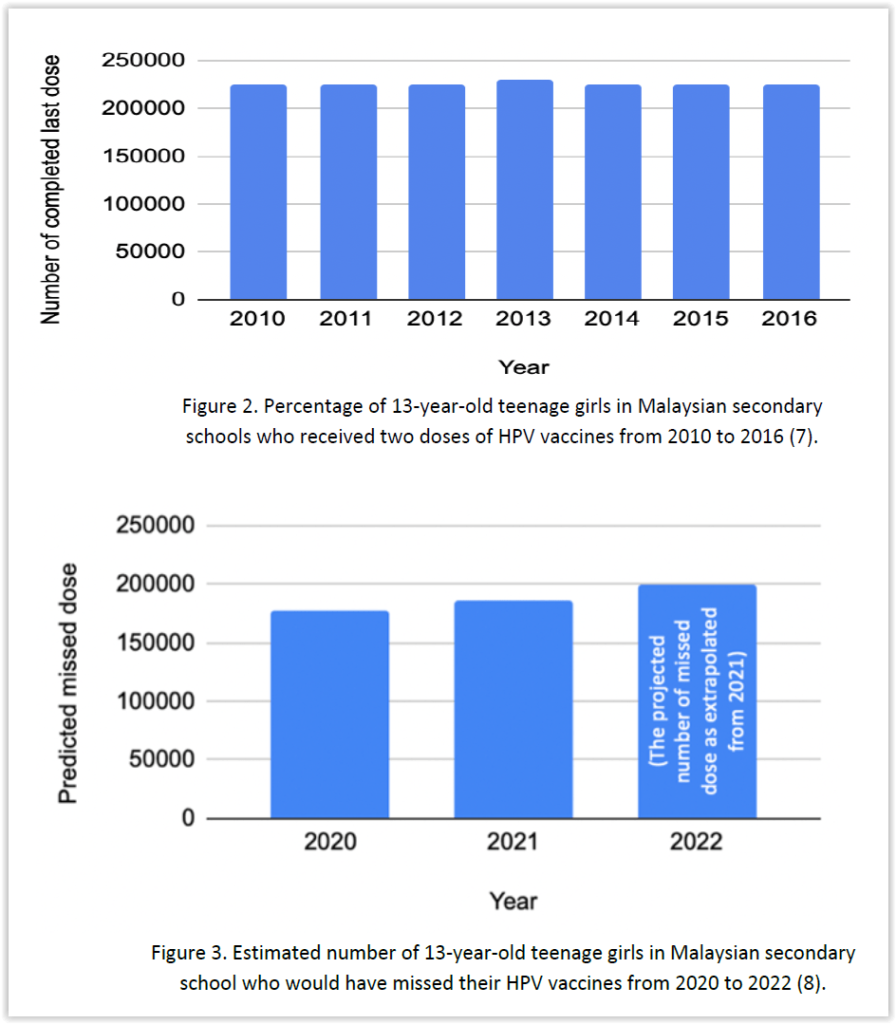
The National Cancer Society of Malaysia (NCSM) announced in a media briefing here yesterday that based on the HPV vaccination rate in previous years, at least 176,944 and 186,593 13-year-old girls would have missed their HPV shots in the disruption of the National Immunisation Programme (NIP) in 2020 and 2021 respectively.
A further 200,000 girls in this cohort are estimated to have missed out their vaccinations this year, leading to at least 560,000 teenagers in Malaysian secondary schools missing out on their HPV vaccination that prevents cervical cancer.
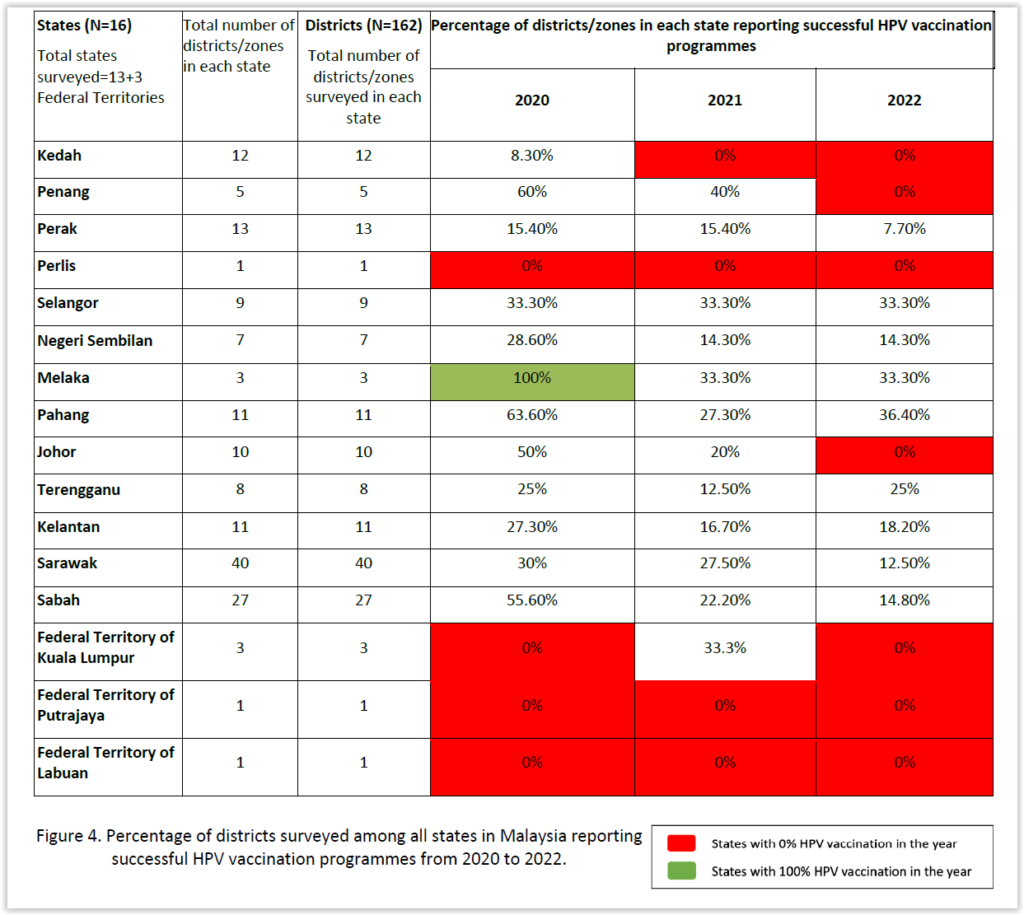
“Overall, most states did not report comprehensively conducting any HPV vaccination programmes from 2020 to 2022,” NCSM stated in its policy brief titled “Restart the HPV vaccination programme” released yesterday.
Districts surveyed in Perlis, Putrajaya, and Labuan did not report conducting any successful HPV vaccination programmes from 2020 to 2022.
“In 2020, there is only really one state — Melaka — that successfully conducted 100 per cent HPV vaccination. Everybody else has got little, little pockets of vaccination being done, but there are states that are completely in red, which is zero percent that they report having done HPV vaccination,” NCSM managing director Dr M. Murallitharan said at the press briefing.
“The situation is very similar in 2021 and now, which is why we are getting a bit anxious, a bit concerned. We are at the end of the second quarter, we are entering perhaps into the third quarter already in 2022, and we do not see any green light at the end of the tunnel.”
Melaka’s achievement of 100 per cent of its districts or zones reporting successful HPV vaccination programmes in 2020, however, did not hold for the following two years, reporting only 33.3 per cent for both 2021 and 2022.
According to NCSM’s investigation, national HPV vaccination rates have been declining over the past three years. In the year 2020, about 58 per cent of districts reported not conducting successful HPV vaccination programmes.
This increased to 72.2 per cent in 2021, before rising again to 79.6 per cent of districts this year reporting not having conducted a successful HPV vaccination programme.
In NCSM’s study, senior assistants in charge of student affairs or school counsellors were asked each year from 2020: “Did this school successfully carry out the HPV vaccination programme for 13-year-old teenage girls enrolled in the school?”
This year, not a single district or zone in Kedah, Penang, Perlis, Johor, and the three Federal Territories of Kuala Lumpur, Putrajaya, and Labuan reported successful HPV inoculation programmes.
NCSM and other civil society groups and advocates urged the government to restart the nationwide HPV vaccination programme for 13-year-old girls in secondary schools in Malaysia next year.
They also called for the implementation of a catch-up vaccination programme in 2023 for girls who missed their shots from 2020 to 2022.
NCSM cited the previous MyHPV programme by the National Population and Family Development Board (LPPKN) in 2019 that gave free HPV vaccines to unmarried Malaysian women born between 1992 and 1996.
“Number one, schools were closed during the lockdown. The poor girls were not going to school. Number two, money was diverted and you can’t blame the government,” Dr Narimah Awin, former director of the family health development division under the Ministry of Health (MOH), told the media briefing.
“If there was so much money for cervical cancer or for breast cancer, but to save lives of Covid, you will have to divert that resources. So for these two main reasons, HPV vaccination practically suffered.”
The halting of the national HPV vaccination programme, advocates warned, has a hidden cost.
According to former Malaysian AIDS Council president Dr Raj Abdul Karim, many girls drop out of school when they reach Form Three. Hence, suspension of the HPV vaccine roll-out and the lack of a catch-up programme could result in losing those girls.
“If we don’t have the catch-up programme, the girls who have missed, the 13-year-old girls – they are now in Form Three, and we need to catch the girls before they go to Form Four because you see that the dropout rates of Form Three is high. So we need to be very strategic so that we can get these girls as fast as possible,” Dr Raj told the media briefing.
Preserving the health of these young women is important, but there is much to lose in terms of cost as well if the government does not move quickly.
The United States’ Centers for Disease Control and Prevention (CDC) recommends that two doses of the HPV vaccine be given to children aged 11 to 12, with a gap of six to 12 months between each jab. For adolescents aged 15 and above, it is recommended that they receive three doses over a period of six months.
Therefore, as the clock ticks, these girls who are still within the two-dose age limit will soon move into the three-dose requirement, costing the government more money if it does not act with haste.
“If you vaccinate our girls before the age of 15 they will only require a two-dose regimen, but once they cross the 15 years, that threshold, they now need to start getting three doses for it to be a successful completion of the HPV vaccination regimen,” Dr Murallitharan said.
“This means per year, we are already looking at just for every 100,000 girls, we are looking at an additional 100,000 doses…and equivalently, this is just extra money which I think the government and the country can ill-afford at any point in time.”
In Malaysia, adults seeking to be fully inoculated (three doses) against HPV can expect to pay RM1,000 upwards in private health care facilities. As an example, Sunway Specialist Center charges RM1,888 for the full three doses, while Kelana Jaya Medical Centre charges RM1,750.
That being said, Dr Narimah assured the panel that the money for the HPV vaccines, while unavailable this year, is almost a certainty next year.
”Kementerian Kesihatan is putting up a case, they may get [it], but not certain yet. What I was told was more than 60 per cent chance, they will get the money to buy vaccines this year. So, restarting the program in 2023 is almost a certainty.”
Cervical cancer is the third most common cancer among women in Malaysia and is mainly caused by HPV. HPV vaccines, by preventing HPV infections, protect individuals against 90 per cent of HPV-related cancers.
Since 2010, the Malaysian government has implemented a national school-based HPV immunisation programme, giving 13-year-old girls in secondary schools fully subsidised vaccines in a two-dose regimen six months apart.
From 2010 to 2016, MOH reported that 85.8 per cent of this cohort – about 250,000 individuals per year – have been vaccinated.
“HPV vaccination as part of the National Immunisation Programme, which was introduced for 13-year-olds, has been an ongoing programme,” Dr Murallitharan said.
“What that has successfully done, in many countries…is when you vaccinate your entire adolescent female population, that really helps in reducing the infective serotypes which cause cervical cancer, especially the 16 and 18 serotype [that] is very instrumental in driving cervical cancer. And that has been successfully reduced in many settings, including ours, through a nationwide vaccination programme.”
Some Muslim Parents Reluctant To Vaccinate Daughters Against HPV

Dr Narimah also brought up her experiences with Muslim parents who were unwilling to allow their daughters to receive the HPV vaccine because they were afraid that by being vaccinated, their children might become more promiscuous.
“This is one vaccine where the child needs to get the consent from the parents, and there were many parents, not a big percent, but there were several parents – all Malays, all Muslims – who said, ‘I don’t want my daughter to get this vaccine because you’re telling me this is sexually transmitted. My child knows that she is prevented from a sexually transmitted disease because of the vaccine, they become sexually active’.”
Dr Raj emphasised the need to educate the public about cervical cancer and the need for vaccinations to avoid vaccine hesitancy that comes with all vaccinations and immunisations.
“Any vaccine that comes along will bring with it people’s perceptions, people’s attitudes, and even from the medical circles as well. So, we need to be upfront and very strong in our convictions and in our data that the HPV vaccine is very important for cervical cancer,” she said.
“Since we may not have the budget for this year, the end of the year, I was going to suggest that we focus on community awareness and dissemination of information to the public and especially to girls again and to their parents, because you know you need consent. ”
Dr Murallitharan reiterated the demands of the NGOs.
“We appeal to the government so to please do these two things: one is reenergise, restart, rejuvenate the vaccination programme, and of course, we need to very seriously put resources into a catch-up programme.”
Dr Narimah said she would work to include HPV vaccination in the Health White Paper that Health Minister Khairy Jamaluddin intends to table in Parliament by year end.









