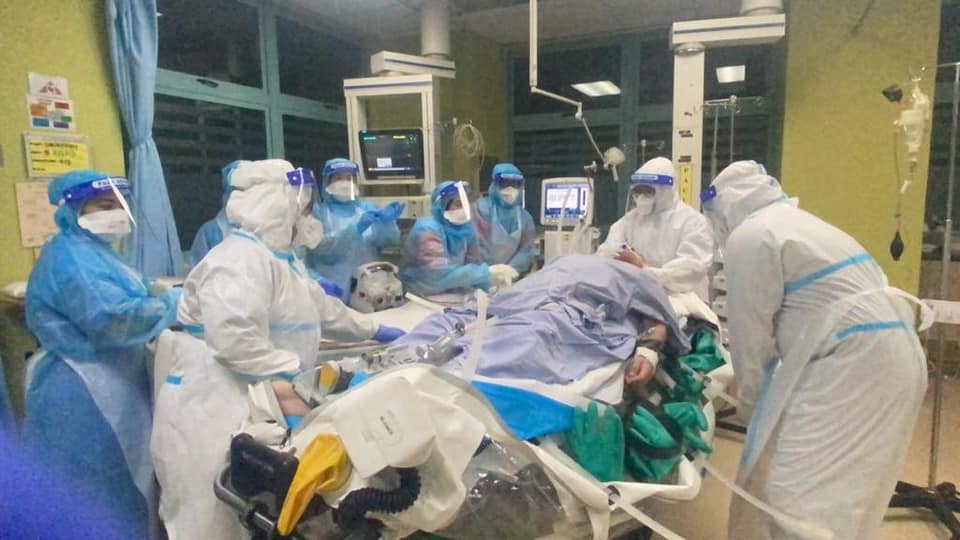
KUALA LUMPUR, May 17 — Across the Klang Valley, medical frontliners are pushed to the brink with rising Covid-19 cases as this time, unlike previous waves of the epidemic, patients are rapidly deteriorating.
They say that stable Covid-19 positive patients who undergo quarantine at home or at low-risk quarantine and treatment centres (PKRC) suddenly develop breathlessness and lethargy and quickly deteriorate after about seven days.
This is seen among the elderly above the age of 50 and younger patients in their 20s and 30s with underlying health conditions or among those who are obese.
Over the past week, between May 9 and May 15, Klang Valley has reported a total of 13,397 new Covid-19 cases and 93 coronavirus fatalities: Selangor (10,396 cases, 64 deaths), Kuala Lumpur (2,906 cases, 28 deaths), Putrajaya (95 cases, one death). Covid-19 cases and deaths in the Klang Valley comprised 45.6 per cent of 29,386 new confirmed infections and 44.5 per cent of 209 new deaths nationwide in the 19th epidemiological week.
The government has imposed a nationwide lockdown for about four weeks until June 7 amid the new surge of infections that has led to full intensive care units (ICUs) across multiple states.
CodeBlue interviewed three doctors from Sungai Buloh Hospital, Serdang Hospital, and Ampang Hospital about their experience in handling the sudden surge of Covid-19 cases in the Klang Valley. CodeBlue is keeping their identities anonymous as government doctors are not allowed to speak to the media without prior permission from their higher ups.
Over the past one month, patients, who initially tested positive with Covid-19 and were stable while being quarantined at home or at the PKRC, suddenly started presenting to the Emergency Department (ED) with shortness of breath and lethargy, an anonymous doctor from Sungai Buloh Hospital told CodeBlue.
“First few days after being diagnosed with Covid-19, they are stable at home or at MAEPS, but after about seven days they deteriorate so fast,” the anonymous doctor from Selangor’s main Covid-19 hospital told CodeBlue.
“Patients need oxygen up to high-flow mask as the lungs are already infected with the virus completely that makes them breathless. The virus is more virulent than before.
“They deteriorate rapidly and need high oxygenation such as face masks and high-flow masks. Currently, too many patients need oxygenation compared to the third wave,” the Sungai Buloh Hospital doctor added.
Due to overwhelming patients who require supplemental oxygen in Sungai Buloh Hospital, patients have to wait at the ED before being admitted to the ward, said the anonymous doctor.
On May 11, in the middle of the night, Sungai Buloh Hospital doctors had to quickly discharge Covid-19 patients from the ward to Pusat Kawalan Kusta Negara (PKKN) to make room for more patients from the ED to be admitted to the ward.
The doctor explained that previously during the second and third wave, patients were mostly in Category 3A Covid-19 (not requiring supplemental oxygen but have pneumonia), so Sungai Buloh Hospital was able to discharge the patients quickly on Day 10 or Day 12 out from the ward.
“But as currently most of our patients are Category 4A (requiring supplemental oxygen), the discharge rate is slowing down,” the anonymous doctor said, while pointing out that currently patients can be admitted up to 20 days.
“We need to treat patients up until we are able to turn off their oxygen (when they no longer need oxygen support), then discharge most of them home.”
The government has yet to acknowledge that the country is now in the fourth wave of the epidemic, but public health experts have urged the government to increase testing so that more cases can be detected early before patients themselves present to the hospital with severe Covid-19 symptoms.
Meanwhile, because more patients are severely ill this time, the ICU in Sungai Buloh Hospital is overloaded with patients who require ventilation hence, some ventilated patients are being treated in the critical wards instead of the ICU.
“When we don’t have enough ventilator support, we also transfer some patients to other hospitals for ICU admission and ventilator support,” the doctor told CodeBlue.
In Sungai Buloh Hospital, the medical frontliner said that both young and the elderly are affected with severe Covid-19. For younger patients, most of them usually are either obese or have multiple comorbdiites.
“The youngest patient who needed ventilation was a 27-year-old man who was obese and had underlying hypertension,” the doctor added.
With Rising Severe Covid-19 Cases, Ampang Hospital Lacks Manpower
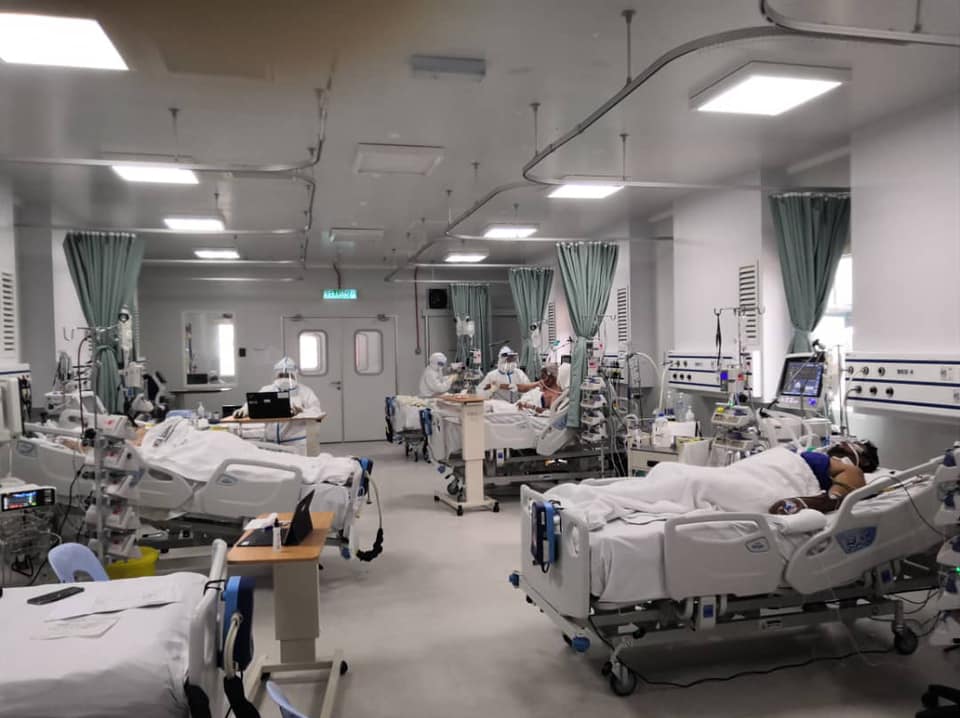
Similarly, like in Sungai Buloh Hospital, Covid-19 patients admitted in Ampang Hospital are also very ill and deteriorate rapidly.
An anonymous doctor from Ampang Hospital in charge of severely ill patients said that the facility lacks manpower because severe Covid-19 patients are continuously being admitted.
“Manpower is not enough obviously. Sometimes, staff nurses have to take care of two to three patients in an intensive care setting,” the doctor said.
“Doctors also not enough as lots of admissions recently and most of them with respiratory issues turn out to be positive for Covid-19. I wish we can get more staff, equipment and proper ICU or ward setting to manage Covid.”
The doctor said that patients in the ICU in Ampang Hospital are in Category Four and Five, meaning they are severely ill and require supplemental oxygen or intubation.
“Luckily, so far we have enough ventilators, but seeing the trend, I’m not sure. Because the conditions now are as tight as we can and we don’t have enough beds.”
The doctor also noted that because patients are more ill than previous waves of the epidemic, the discharge rate has also been slow.
Serdang Hospital’s ICU Full, Patients Wait Hours In ED

An anonymous doctor from Serdang Hospital, who is part of the Covid-19 team, said that in Serdang Hospital, which is a Covid-19 hybrid hospital, five wards have been allocated for Covid-19 patients.
Despite that, patients still have to wait for hours in the ED before being admitted to the ward as both wards and ICU are full.
The doctor also said that this time the virus is more virulent as most patients are in Category Four, needing supplemental oxygen.
Although the doctor has been vaccinated, the fear of bringing the virus home to family members who have yet to be vaccinated against the virus is still there.
“I feel the same way. (However), I have not compromised my safety, it is personal protective equipment (PPE) all the way,” the doctor told CodeBlue.
The doctor also pointed out that the Covid-19 allowance that each Covid-19 frontliner should be getting doesn’t come in consistently for all. Some frontliners get it on time, while some get it later.
“My November allowance came in last month,” the doctor said.
Health director-general Dr Noor Hisham Abdullah said last Saturday that the bed occupancy rate for 850 ICU beds nationwide designated for Covid-19 patients has reached 80 per cent as of May 14. Selangor, Kuala Lumpur, Penang, Sarawak, Kedah, and Perak have exceeded 80 per cent occupancy in Covid-19 ICU beds, while Covid-19 ICU beds in certain hospitals are already full, he added.
It is unclear if the severe nature of the new surge of coronavirus infections is due to increased virulence from new strains, or because many Covid-19 patients this time are being diagnosed at a late stage of their disease due to a lack of testing and contact tracing.
In a recent report on the 18th epidemiological week in Malaysia from May 2 to 8, the Ministry of Health (MOH) said that they have identified 20 Covid-19 cases with the South African B.1.351 variant, as well as one Covid-19 case with the UK B.1.1.7 variant. Prior to this batch, seven Covid-19 cases have been identified with the UK B.1.1.7 variant, two with the Nigerian B.1.525 variant, and 28 cases with the South African B.1.351 variant.
In a study done in the UK, it was found that the B.1.1.7 variant is associated with an increased risk of death compared to non-B.1.1.7 variants.
Meanwhile, South African researchers said that the B.1.351 variant may be around 50 per cent more contagious based on its faster rate of transmission since its emergence. Nigeria Health Watch reported that currently there is no evidence to indicate that the B.1.525 variant from Nigeria is a variant of concern and further analysis is being conducted.
Malaysian authorities — who do limited genomic sequencing on Covid-19 — have so far detected two imported cases with the B.1.617 variant originating from India that the World Health Organization recently designated as a “variant of global concern”.