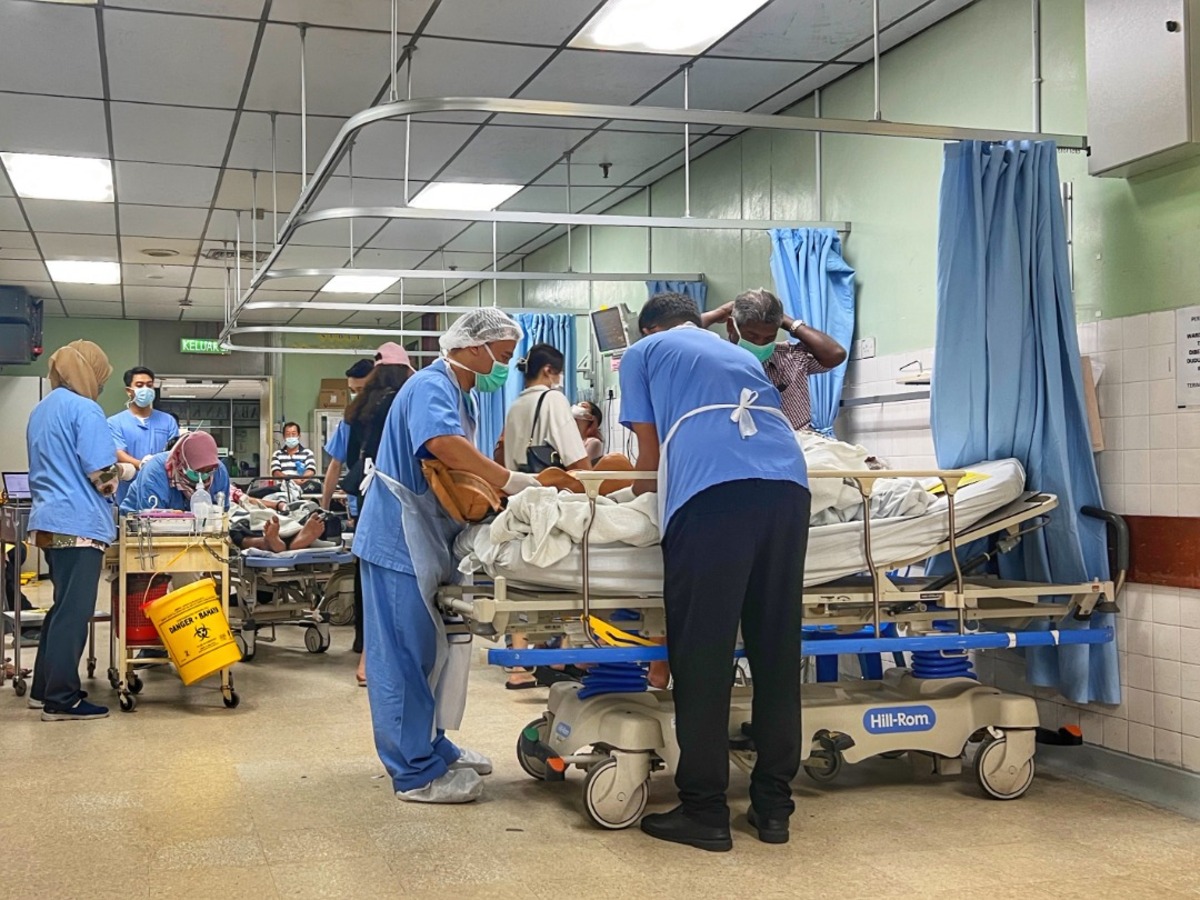
KUALA LUMPUR, Dec 15 – Severely congested emergency departments are an early signal of a deteriorating national health service struggling to cope with increasingly sicker Malaysians, said a medical doctor.
Dr David (pseudonym), who requested anonymity to discuss sensitive issues frankly, equated hospitals’ emergency and trauma departments – known as ETD, or just ED, or casualty – to the canary in the coal mine, referencing an old British mining tradition that is now used as an idiom to mean an early warning of danger or failure.
“Many people consider emergency departments as the canary in the health service coal mine. If the ED is bad, it shows the health service is sick,” Dr David told CodeBlue in a recent interview.
“For me, the Malaysian health service has been dying for the last 15 to 20 years. Now, it’s getting worse and worse and worse. You go to Taiwan and South Korea, you don’t see this problem. They’ve moved ahead because they fixed their system bit by bit and grew it.”
Dr David was responding to CodeBlue’s report that documented how critically ill patients, including ventilated cases, are stranded for up to six days in Raja Permaisuri Bainun Hospital’s (HRPB) emergency department for ward admission, due to insufficient critical care beds and staff.
Most of the severely sick patients coming to the ED at the public tertiary hospital in Ipoh, Perak, are presenting with advanced non-communicable diseases (NCDs) — such as heart disease, kidney failure, and stroke — that worsened after the disruption of care from two years of Covid lockdowns.
Dr David highlighted the limited screening and prevention of chronic conditions like diabetes, obesity, and hypertension. “It would be good if adult medicine physicians played a bigger role in preventing disease, rather than just treating the end result.”
“Diabetes, stroke, myocardial infarction injuries, and elderlies with pneumonia and other infections are the key things presenting in ED, besides trauma. You don’t see this ED problem for paediatrics or surgeries; it’s mainly adult medical problems,” he pointed out.
“The paeds team comes and picks up their patients from the ED. The surgical and orthopaedic teams respond quickly to surgical problems and trauma. Gynae O&G, patients go straight to them.
“We’re left with these adult medical problems as the bulk in ED. Perhaps the adult medical specialists need to look into being more involved in ED.”
Dr David pointed out that paediatric and surgical patients can get quick appointments in public hospitals.
“In fact, if you say you have a breast lump, the surgeon will give you an appointment in three days. But if you say you have diabetes that’s not so well controlled, it might be two to three months before you get to see a physician.
“Somebody else has to manage you first because they say clinics are choked — coming back to the original problem of limited disease prevention activities.”
Place Physicians In ED And Increase Medical Clinics, Not Open New Wards
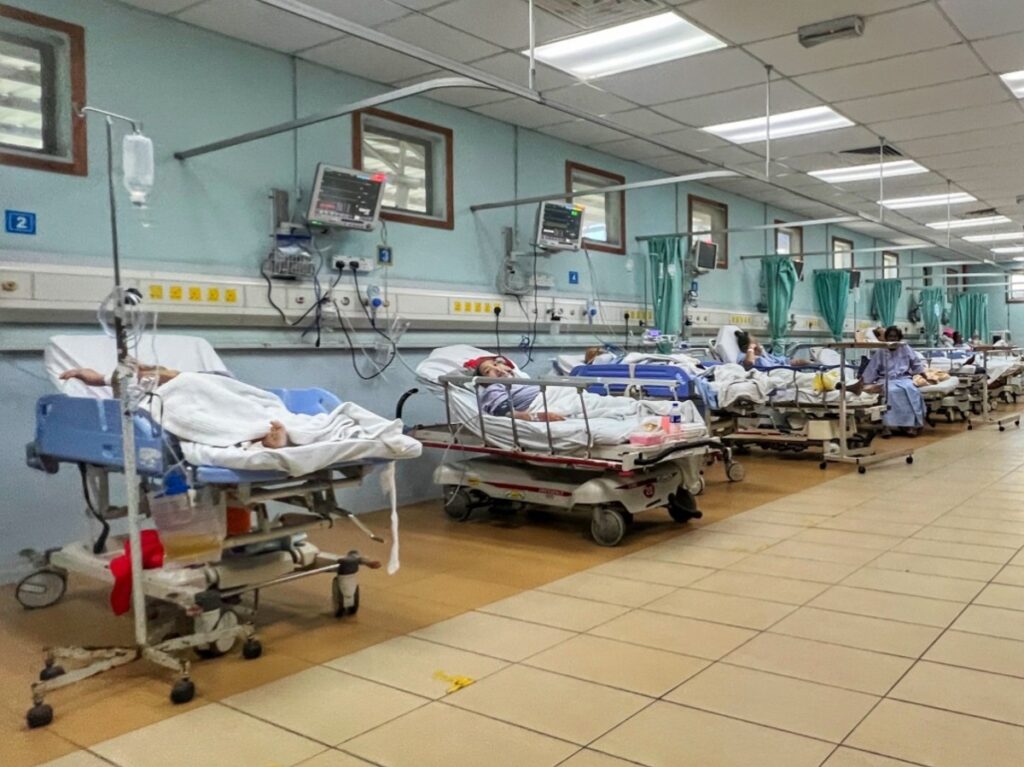
Dr David said many disciplines reduce patient admissions by improving outpatient clinic referrals or working closely with ED to send stable patients to outpatient clinics during office hours.
“If you think that person doesn’t need admission, just send them straight to us. We’ll manage from the clinic and decide about admission. Or if they’re severely ill, just call for us to pick them up straight from ED,” he said.
“Adult medicine doesn’t do that. If they had a few physicians rotated through casualty every day, then they could make decisions on the spot and optimise patients – ‘I think you don’t need to be admitted, why don’t you see me in the clinic tomorrow?’
“You have to be ‘at the door’ to do this. Currently, they expect ED to manage as their beds are full.”
CodeBlue’s report highlighted that some patients, including seriously ill ones, waiting for days in HRPB’s ED are stranded in what an HRPB medical officer dubbed as “no man’s zone”, due to poor monitoring and unclear patient responsibility between the emergency and ward teams.
Dr David noted that in some countries, hospital administrators make the decision to choke the wards instead of the ED to improve ownership of cases.
“They put the patients in the ward corridor and they find that by doing that, the physicians manage better because the patients become theirs,” he said.
“Now, the patients are not the physician’s yet. There’s no ownership for this. But there’s a lot of complaining – workload, not enough staff, not enough wards.
“I can tell you, the moment you grow another ward, the ward will be full. You’ll be back to square one.”
Two to three medical officer (MO) trainees can be placed full time in EDs, said Dr David, to organise cases – and more importantly, take ownership of patients and recognising the ED as their “ward” – by either sending patients to be admitted to ward or less sick ones to medical outpatient clinics.
While Dr David acknowledged that some increase in beds was necessary – perhaps 40 per cent – he stressed the need to reorganise management of adult medicine cases as a whole. Otherwise, opening new wards is akin to building another flyover to handle traffic jams without improving public transport.
Boost Ambulatory Care, Community Health Services, Nursing
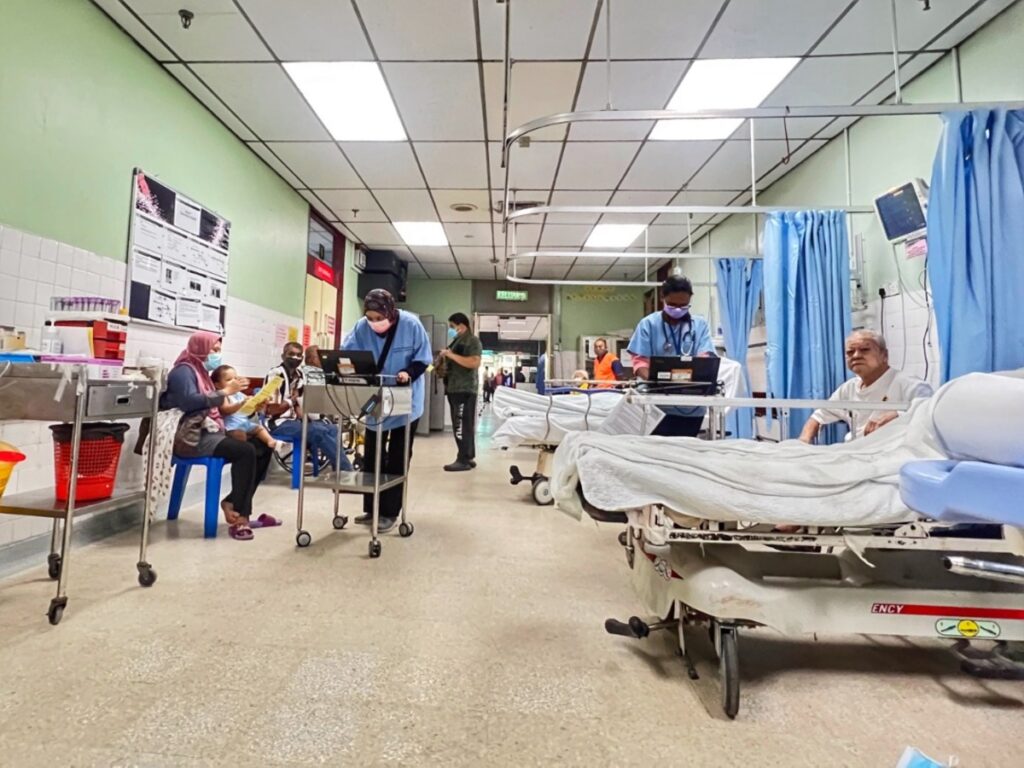
Dr David called for an expansion of ambulatory care and community health services like nursing and rehabilitation.
Ambulatory care, he said, is not just about day care surgery that doesn’t require admission, but can be extended to paediatrics and adult medicine. For example, instead of keeping a child with pneumonia in a ward unnecessarily, who just needs a few more days of IV antibiotics, the child can either be sent to an ambulatory care centre for antibiotic infusion or sent home, where a nurse will come by to give the antibiotics.
“Many oncology patients can be managed in ambulatory care. So if we can do it for oncology, even children with cancer, surely you can do it for many other people. That’s how we can reduce the bed volume.”
Community health services are necessary for transition care, Dr David said, citing another problem of patients with chronic conditions who are unnecessarily stuck in a ward because their families prefer to let the hospital take care of them.
“As an example, if an elderly person has a stroke, the family feels that the hospital can do a better job of caring for him as they are not able to do so at home. Hence, they leave him in the hospital.”
Dr David estimated that about 5 per cent to 7 per cent of hospital beds are occupied by these chronically ill people. Perak has the oldest population in the country. The state constituency of Pasir Pinji in the state capital city of Ipoh has one of the highest old-age dependency ratios in Malaysia.
He noted that although Batu Gajah Hospital has been opened up as a rehab centre, people complain about having to travel from Ipoh to Batu Gajah to see their family, instead of seeing them in HRPB nearby.
“This is a problem of society having no care for people with chronic needs,” he said.
“We don’t have community services like nursing and rehab that can do the transition care. If you have, you can say to this woman, ‘Don’t worry, we’re going to send your father home. One nurse will come every morning and look after him’.
“You cannot expect public health staff to do this. They’re running on thin ice, their services are so stretched from womb to tomb that they can’t do this.
“We need a cadre of nurses, which we don’t have because we have not boosted our nursing manpower and let them be ‘stolen’ by Singapore and Saudi instead.”
The Association of Private Hospitals Malaysia recently called for a liberalisation of the nursing labour market to allow foreign nurses into Malaysia, highlighting an unprecedented shortage of nurses in private and public hospitals.
Dr David highlighted the lack of nursing positions created by the Public Service Department (JPA), stressing that the government health service needs to have an accurate number of the positions needed and the percentage filled, so as to reflect the actual shortage. The nursing sector can then be grown to fill those vacancies.
“In the general medical ward, it should be one nurse to four patients. Right now, it’s three nurses to 32 at times. That’s assuming there are no canvas beds and extra beds around.”
He called for higher salaries for nurses, as well as better quality nurses: “Many people don’t think about nurses. Nurses are the executor of health; doctors are just the instructor, except when it comes to surgical procedures, then they’re the executor.”
Reorganising work management in adult medicine, Dr David said, will also enable personalised care in the public sector so that patients can see the same doctor for better outcomes, instead of physicians having to rush through a large volume of patients impersonally.
“Solutions are possible. Run more medical clinics, make yourself accessible, transition some people straight from ED to the medical clinic, see them, optimise them, send them home. Tell them to come back again tomorrow, ‘we do some more care for you’.”