MONTREAL, August 10 – Police training on harm reduction, an intervention that seeks to reduce harms linked with drug use and ineffective drug policies, can be a cost-effective strategy to cut down arrests and prevent overdose among people who inject drugs.
A study on a police education programme in Tijuana, Mexico, a major city on the border between Mexico and the United States, found that training officers on the public health benefits of syringe service programmes, methadone maintenance therapy, and on HIV transmission, could reduce fatal overdoses and help curb the spread of the disease.
Javier Cepeda, assistant professor of epidemiology at the US-based Johns Hopkins Bloomberg School of Public Health, said numerous studies and systematic reviews have shown that syringe confiscation from police has been associated with increased odds of syringe sharing and that law enforcement officers often target harm reduction sites to harass or arrest people who inject drugs.
“Police arrest often serves as a gateway to the criminal justice system, primarily through incarceration, which has been associated with many harms,” said Cepeda, who presented the findings last July 30 at AIDS 2022, the 24th International AIDS Conference, in Montreal, Canada.
He said people with a history of incarceration have higher HIV and hepatitis C incidents and are at an “extraordinarily” high risk of overdose mortality in the immediate post-release period after release from incarceration.
“So given this context and evidence suggesting that policing is actually a structural determinant of health, there was a novel police education programme called ‘Proyecto Escudo (Project Shield)’ that was conducted to align policing practices with evidence-based public health principles,” Cepeda said.
Under Proyecto Escudo, conducted by a binational team from the University of California (UC) in San Diego, US, and the US-Mexico Border Health Commission, a total of 1,806 municipal police officers in Tijuana received training on three modules.
The first module focused on harm reduction such as syringe services programmes and methadone maintenance therapy.
The second module was on decriminalisation reforms passed by the federal government in 2009, which established threshold amounts for drug possession and mandated treatment for repeat offenders, though “much of that was not being implemented” at the local level, Cepeda said.
The third module was on occupational safety on averting accidental needlestick injuries and basic HIV and hepatitis C epidemiology.
Researchers then measured outcomes among two cohorts, namely among police officers that were followed for two years, and a parallel cohort of people who inject drugs before, during and after training that had been followed up.
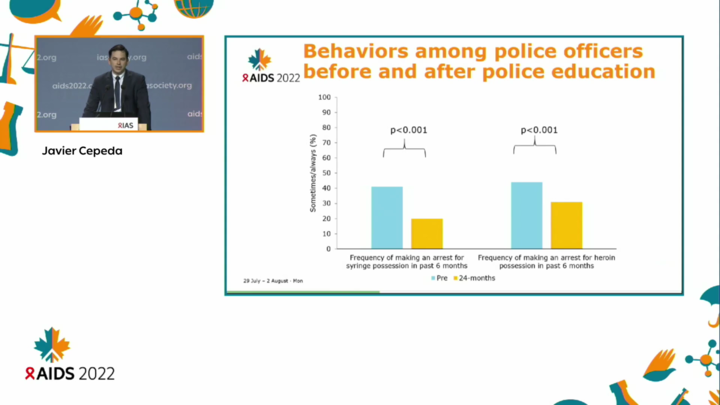
Police officers reported making significantly fewer arrests for syringe possession in the two years after the training was delivered, falling from 41 per cent to 20 per cent. The proportion that said they sometimes or always made arrests for heroin possession fell from 44 per cent to 31 per cent.
The finding was corroborated by data from the cohort of people who inject drugs, who were 68 per cent less likely to have been imprisoned in the post-training period compared to the period before training.
“So we really want to use that effect (our intervention effect) as a proxy on how police training could impact public health outcomes among people who inject drugs,” Cepeda said.
Following that, UC San Diego researchers used modelling techniques to project the short- and long-term impact and cost-effectiveness of the training on preventing HIV transmission and fatal overdoses.
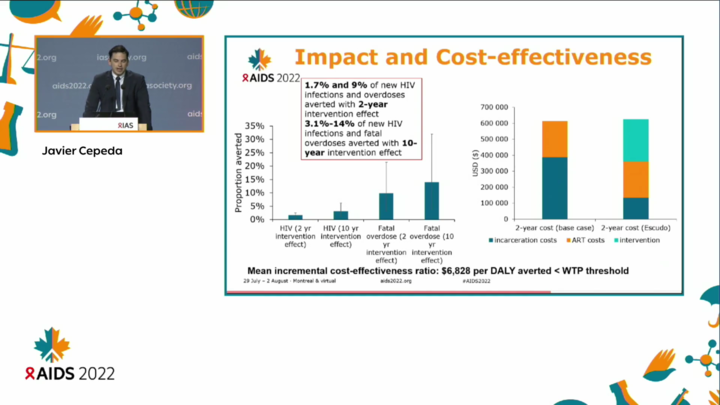
Their estimations suggest that the training would result in 1.7 per cent fewer HIV infections two years after the training and 3.1 per cent fewer HIV infections ten years after the training.
The impact on fatal overdoses would be more significant, with 9 per cent fewer overdoses within two years and 14 per cent fewer overdoses after ten years.
Cepeda added that despite the high cost of the training programme, it was offset by the decline in incarceration-related costs – indicating that the intervention was cost-effective.








