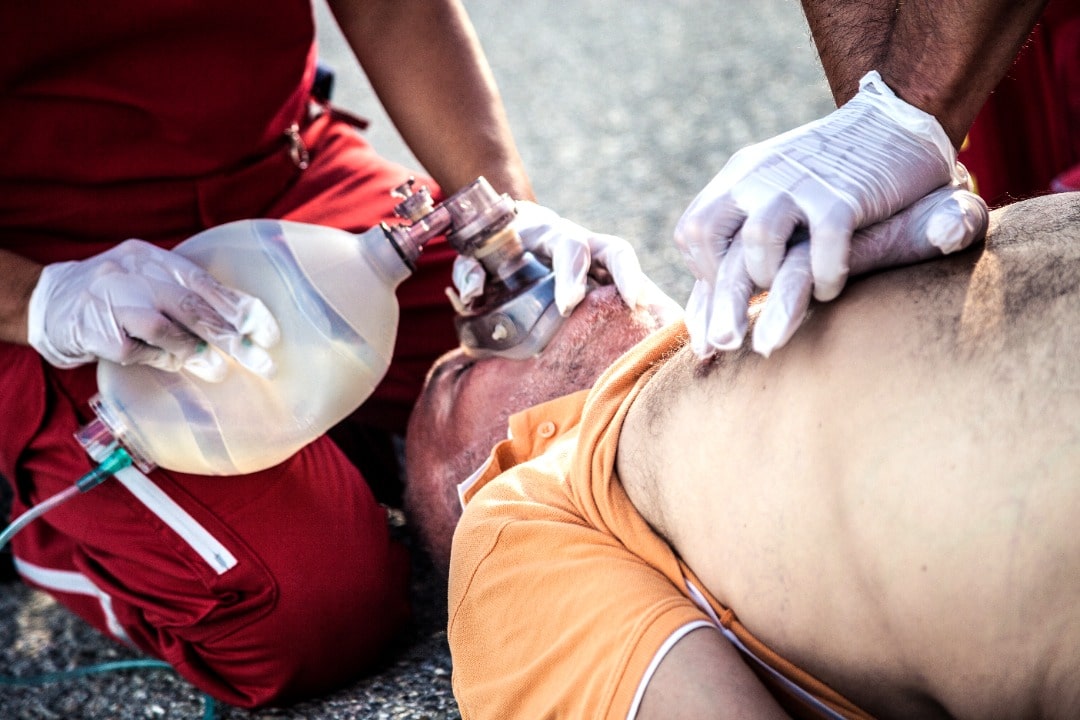
I used to think that the main problem with prehospital care was ambulances not being able to get to an emergency on time because of traffic or entitled VIPs who refuse to give way to ambulances.
Never would I have thought that Malaysia could have a potential problem with paramedics who don’t bother to try to save a person’s life because they’re automatically presumed dead.
The case of the late St Michael’s Institution teacher Kumaraveloo Terpari @ Thirupathy, who died from a heart attack at age 43, has shattered my faith in our public emergency medical services.
A medical assistant (MA), or paramedic, from Raja Permaisuri Bainun Hospital (HRPB) allegedly left Kumar in his car where he collapsed during a traffic jam in Ipoh, Perak, last April 13, withheld cardiopulmonary resuscitation (CPR) from the patient, and declared him dead to bystanders – despite the ambulance arriving at the scene in optimal time, within 13 minutes of the public hospital receiving the emergency call from the MERS 999 centre.
Kumar’s case is probably the first publicly recorded case of alleged lapses in prehospital or emergency medical care in Malaysia, due to the unusual access of the victim’s next-of-kin to official documents and police photographs of the scene that would not normally be made available to the ordinary rakyat.
MAs have come out furiously on Facebook in defence of their fellow MA – not to defend his reported decision to withhold CPR or to leave a patient in his vehicle – but to call for police investigations under the Official Secrets Act (OSA) for the disclosure of official documents.
In contrast, the Malaysian Association of Medical Assistants (MAMA) said in a statement to CodeBlue Sunday that the authorities should be given space to conduct investigations into Kumar’s case — without any preconceived notions or assumptions — stressing that MAs strongly hold to the values of their “professional oath to provide care to relieve pain and save lives.”
Kumar’s family said in a statement, after meeting with HRPB and Perak state health department officials last Tuesday, that the Ministry of Health (MOH) hospital admitted that the MA’s algor mortis finding was incorrect.
The MA in Kumar’s case had marked “algor mortis”, the first “clear sign of death” category in his prehospital care form that categorised the case as a “medical”, not trauma case. The paramedic’s assessment did not mention finding any traumatic injury on the patient. Algor mortis is the second post-mortem stage of death when the corpse cools until the body temperature matches the outside temperature.
However, MOH officials justified the MA’s decision to withhold CPR on the basis of a purported policy of a 15-minute cut-off point for the lifesaving intervention, according to Kumar’s family.
HRPB’s ambulance arrived at between 14 and 19 minutes from the time the 999 call was made by a bystander. Although Kumar reportedly collapsed at 6.10pm, based on an eyewitness account to CodeBlue, which was 20 minutes before the arrival of the ambulance, this does not necessarily mean that his heart immediately stopped beating at the moment of his collapse – unless it was measured at that point in time.
HRPB’s reported claim of a 15-minute cut-off time for CPR from the time of collapse is not a policy documented in any MOH guidance, including the National Committee on Resuscitation Training’s (NCORT) 2012 Guidelines for Resuscitation Training in Ministry of Health Malaysia Hospitals & Healthcare Facilities, the NCORT BLS subcommittee’s 2017 Basic Life Support Training Manual, or the Selangor state health department’s 2018 Guidelines and Policy: Ambulance and Prehospital Treatment Services. None of those MOH policies mention withholding CPR in adult basic life support.
Both the 2012 and 2017 guidelines by MOH’s NCORT, in fact, state that chest compressions shall be started with absence of breath or presence of abnormal breathing that is to be treated as a sign of cardiac arrest. Cardiac arrest happens when the heart suddenly and unexpectedly stops pumping.
MOH’s NCORT even states in its 2012 guideline that “it is a duty of every doctor to attempt resuscitation on any patients with cardiac arrest.”
The 2016 Recommendations on the Minimum Standards Required for the Management of Adult Out-of-Hospital Cardiac Arrest in Prehospital Care Services by the College of Emergency Physicians, Academy of Medicine Malaysia (AMM), which is a medical specialists’ association, does contain guidelines on withholding CPR.
AMM’s guidelines state that CPR should not be initiated on adult out-of-hospital cardiac arrest (OHCA) victims with signs of “clinical irreversible death”, either rigor mortis, dependent lividity, injuries incompatible to life (such as decapitation, transection, incineration with more than 95 per cent full thickness burns), or decomposition.
According to AMM, CPR intervention can also be withheld from traumatic cardiac arrest (TCA) victims with signs of clinical irreversible death or no signs of life reported in the preceding 15 minutes prior to the arrival of the prehospital response team. TCA is different from medical (non-traumatic) cardiac arrest; the former is caused by severe injury.
CPR also shall not be initiated when there is a do-not-attempt-resuscitation (DNAR) order, according to AMM’s recommendations. However, AMM states that it is appropriate for responders to initiate CPR in absence of DNAR order information, in line with ethics to provide medical care in the best interest of the patient. AMM’s guideline specifically states that initiation of CPR does not require consent “because any delay of resuscitation effort decreases the chance of OHCA victim’s survival.”
If MOH maintains that it is a national de facto policy to withhold CPR from cardiac arrest victims should ambulance response teams arrive in more than 15 minutes from the victim’s time of collapse, then this essentially negates the need for emergency medical services, since MOH’s own target ambulance response time is 15 minutes from an emergency call.
A victim’s time of collapse is also not officially recorded per se, unlike 999 calls, as it depends on approximations by eyewitnesses who are not likely to be looking at their watch or recording the exact time they see someone collapse.
Beyond all these documents, policies and timelines, the one thing that jumps out in Kumar’s case is a single haunting photograph of the man lying slumped in his car, with monitor leads attached to his chest under his shirt. Right till the end, the patient was never removed from his vehicle to be placed on a stretcher.
MOH needs to clarify if the first responders in Kumar’s case truly provided patient-centred care — in line with MOH’s own policies and guidelines — in the best interest of the patient’s survival.
Throughout the story of Kumar’s case, the role of the ambulance driver has also been unclear. What was the ambulance driver doing during the entire emergency response? Are ambulance drivers paramedics too who are trained in basic or advanced life support?
How does MOH perceive the role of the ambulance? Is it to transport patients from Point A to Point B (no different from a taxi) and/ or to stabilise an emergency patient for further treatment in a hospital?
What is the point of equipping ambulances with automated external defibrillator (AED) devices if paramedics automatically presume death when they see a flatline and don’t bother with resuscitation efforts?
Sending out teams of at least two paramedics, including the driver, would ensure mutual support and could reduce the probability of a single MA making unilateral decisions to withhold CPR from the victim.
Kumar’s case sheds light on Malaysia’s prehospital care and emergency medical response that may not have been updated for years. Unlike hospital settings, where doctors work in teams and do the best they can to save a patient’s life the second the patient enters the hospital, the work of a paramedic on the field out of hospital is often not witnessed in-person by fellow health care professionals.
There is a lack of mechanism for accountability in prehospital care in the event that a paramedic makes the wrong decision, especially if it leads to a patient’s death.
How many times have paramedics from public ambulance response teams across the country, not just HRPB, allegedly withheld CPR from cardiac arrest victims? For how many years have such alleged practices been going on?
According to the Department of Statistics Malaysia’s November 2021 report, ischaemic heart disease remained the main cause of death in Malaysia, comprising 17 per cent of 109,155 medically certified deaths in 2020. How many of these deaths occurred among patients who were denied CPR intervention in the event of a “witnessed collapse” (ie: collapse seen by eyewitnesses)?
We will likely never know, unless MOH does an extensive audit across HRPB and selected public hospital ambulance services from a few years before the Covid-19 pandemic to date.
The MA in Kumar’s case should not be made a scapegoat. Whatever he did on the field was likely approved by his supervisors and was the result of an apparent institutional culture that – unseen till now – allegedly permitted withholding CPR from cardiac arrest victims despite the victim’s uncertain status of death.
Unless MOH conducts an external inquiry – not just in Kumar’s case, but to review its entire emergency medical service – Malaysians will never know if a public ambulance team responding to a 999 call in the event of an unpredictable collapse will do everything in its power to try to save their life.

Boo Su-Lyn is CodeBlue editor-in-chief. She is a libertarian, or classical liberal, who believes in minimal state intervention in the economy and socio-political issues.