KUALA LUMPUR, March 16 – Nearly three times more adults in their 40s and 50s with underlying health conditions died from Covid-19 in Malaysia in the past five weeks than seniors aged 60 and older without comorbidities.
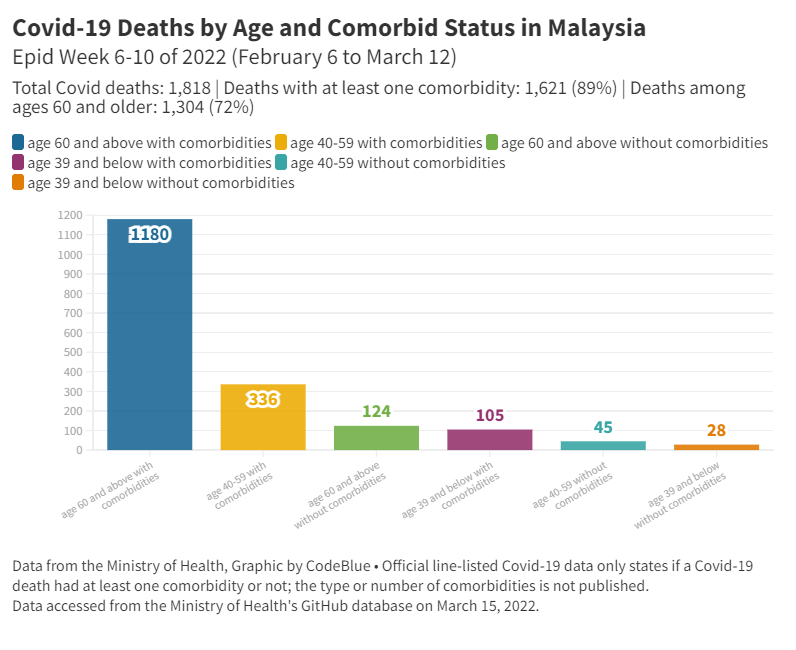
Official Covid-19 mortality statistics showed 336 deaths reported in the 40 to 59 age group with comorbidities from epidemiological week six to 10 (February 6 to March 12), 171 per cent higher than 124 fatalities recorded in those aged 60 and older without underlying health conditions.
Senior citizens and the elderly aged 60 and above with comorbidities recorded the highest number of Covid-19 deaths at 1,180 cases, comprising 65 per cent of total 1,818 coronavirus-related casualties in the past five weeks.
Similar Covid-19 fatality rates were reported between adults in their 30s and younger with comorbidities and healthy elderly people aged 60 and above, with 105 deaths reported in the former – just about 18 per cent lower than 124 fatalities in the latter group.
Surprisingly, the 105 coronavirus deaths reported among unhealthy young adults in their 30s and younger exceeded the 45 fatalities reported in older adults aged 40 to 59 without underlying medical issues by 133 per cent.
The fewest Covid-19 deaths were reported in healthy adults aged 39 and younger in the past five weeks at 28 cases, just about 2 per cent of the 1,180 fatalities recorded in the highest-risk group of seniors in their 60s and older with underlying health conditions.
This shows that about 42 unhealthy elderly people die from Covid-19 for every healthy young adult who succumbs to the virus.
Most Covid-19 deaths occurred among Malaysians from February 6 to March 12 at 1,739 cases (96 per cent of total 1,818 deaths). Fatalities in Malaysian males (1,018) outnumbered females (721) with a ratio of 1.4 to 1.
According to MOH data, those with comorbidities across age groups comprised 89 per cent of Covid-19 deaths in that period at 1,621 cases.
By age, 72 per cent of Covid-19 victims were aged 60 years and above, regardless of their underlying health status, with 1,304 fatalities.
CodeBlue’s analysis was based on the Ministry of Health’s (MOH) mortality figures, accessed yesterday, that classifies Covid-19 death cases according to their health status, ie: whether victims had at least one reported comorbidity or not. Malaysia’s overall Covid-19 case fatality rate throughout the pandemic is 0.9 per cent; it is currently at 0.3 per cent.
MOH’s line-listed mortality data does not state which or how many comorbidities were suffered by unhealthy Covid-19 victims. The CovidNow team, which manages MOH’s online Covid-19 dashboard, told CodeBlue that they would provide data requested on the prevalence of the type and number of comorbidities among Covid-19 deaths from February 6 to March 12, saying that specific pre-existing conditions are not published in line-listed data due to privacy concerns.
Health care advocates previously warned of a non-communicable disease (NCD) crisis in Malaysia. According to the National Health and Morbidity Survey (NHMS) 2019, nearly two of five adults in the country are estimated to have diabetes.
Some 1.7 million Malaysian adults have all three risk factors for diabetes, high blood pressure, and high cholesterol, while 3.4 million suffer from two of the three main chronic conditions.
As of March 14, some 2.5 million people aged 60 and above in Malaysia have received their Covid-19 booster shots, or 71 percent of 3.5 million people in that age group. CovidNow does not state the boosted percentage of adults for more specific age groups.
MOH has been repeatedly promoting third Covid-19 vaccine jabs for senior citizens, but CodeBlue’s analysis shows that younger adults with underlying medical conditions – even 30-somethings or younger – may have similar or higher risk of dying from Covid than their older counterparts who are in good health.
Malaysian data showing higher Covid-19 deaths among younger people with comorbidities than healthy older adults is consistent with an October 2021 cohort study in Canada that showed the number of comorbidities was a strong risk factor for deaths and severe outcomes among younger individuals infected with Covid-19 aged below 50.
An August 2021 study by Mat Din, H. et al from Universiti Putra Malaysia reported that most of the studied Covid-19 deaths had pre-existing medical conditions, predominantly diabetes and hypertension, and were aged 70 years old or above. Researchers concluded a probable link between Covid-19 mortality and diabetes.
A January 2021 study conducted by the Department of Community Health, Faculty of Medicine, at the National University of Malaysia (UKM), Universiti Kebangsaan Malaysia Medical Centre (UKMMC), and Universiti Malaysia Sabah noted that the highest comorbidity risk factors for Covid-19 mortality in Malaysians were hypertension, followed by diabetes, cardiovascular disease, extra-pulmonary solid malignancy (tumour situated outside the lungs), pulmonary disease or lung disease such as asthma, and pulmonary malignancy or lung cancer.
A retrospective study in Indonesia undertaken from March to September 2020 revealed that high blood pressure, cardiovascular disease, and diabetes were the most common comorbidities in patients’ deaths due to Covid-19. More than half of the patients had two or more comorbidities.
Patients with Covid-19 disease who have comorbidities, such as hypertension or diabetes, are more likely to develop a more severe course and progression of the disease, based on a June 2020 literature review by Sanyaolu, A. et al in the early phase of the pandemic before vaccines were available.
The United States’ Centers for Disease Control and Prevention (CDC) lists comorbidities with the risk of severe illness from Covid-19, including health issues that are common with advancing age (age-related comorbidities), for example, heart conditions, hypertension, and Type 2 diabetes, as well as other comorbidities such as smoking, lung disease, and genetic conditions like Down’s syndrome and sickle cell disease.