KUALA LUMPUR, Dec 28 — Malaysia looks set to end 2020 with a surging Covid-19 epidemic that may force infected people without symptoms to self-isolate at home, as hospital beds rapidly fill up.
As of yesterday, 20,233 active Covid-19 cases occupy about 80 per cent of 25,456 available hospital beds, although it appears that there are still sufficient intensive care unit (ICU) beds and ventilators; currently, there are 111 Covid-19 patients in ICU and 50 on ventilators.
Health director-general Dr Noor Hisham Abdullah told The Malay Mail that asymptomatic people who test positive for Covid-19 should self-isolate at home as they may not be taken to hospitals immediately — marking a break from conventional practice in Malaysia where everyone who tests positive for the virus, even if they’re not sick, are admitted into a facility. In many other countries, including the UK, only ill people are taken to hospital, while asymptomatic or mild Covid-19 cases isolate with their household at home.
On Boxing Day, the Ministry of Health (MOH) reported the highest 24-hour rise in Covid-19 infections at 2,335 cases, as coronavirus cases nationwide have exceeded 1,000 daily on average for the past four weeks since late November.
Former Malaysian Medical Association (MMA) president Dr Milton Lum described the pandemic as unprecedented, turbulent, challenging, and the toughest encountered by most health care professionals in their lifetime, irrespective of whether they were in the public or private sector.
“2020 was annus horribilis for health care professionals globally,” Dr Lum told CodeBlue.
On January 25, the first imported case of Covid-19 was detected among three Chinese nationals in Malaysia. MOH, which was then under the Pakatan Harapan administration, quickly set a standard guideline on the management of Covid-19 and designated 34 government hospitals in each state to screen for Covid-19.
On February 6, the first locally transmitted case was reported in Malaysia. In the midst of the coronavirus outbreak in Malaysia, there was also a political crisis that led to a change of the federal government to the Perikatan Nasional administration led by Prime Minister Muhyiddin Yassin on March 2. As of March 2, the cumulative number of Covid-19 cases reported was 29.
In March, a Muslim religious gathering took place in Sri Petaling, Kuala Lumpur, involving 16,000 participants, including 1,500 foreigners, that subsequently caused a massive Covid-19 outbreak dubbed the Tabligh cluster. The Tabligh cluster, which was the largest cluster at that time, had infected a total of 3,341 individuals and caused 34 deaths.
As Covid-19 cases were rising in March (190 new infections on March 15), the government announced a stringent Movement Control Order (MCO) on March 18, which was initially set for two weeks but extended for seven weeks until May 12, limiting people’s movements to 10km and closing most businesses except for essential services.
The seven-week long lockdown was successful in bringing down Covid-19 cases, as by the last week of MCO from May 6 to May 12, the average number of daily cases nationwide was only 51. In the following four months until mid-September, daily Covid-19 infections were below 100, mostly under 50, and even occasionally hitting zero cases.

Former Health deputy director-general (public health) Dr Lokman Hakim Sulaiman told CodeBlue that the drastic decision on implementing a MCO was necessary to flatten the Covid-19 epidemiological curve.
“It was necessary, and the objective was clear to most economies to buy time so that the country, the people, and the health system in particular could be strengthened to face the onslaught of the infection,” Dr Lokman said.
“Indeed, we did well in flattening the curve, and the number of cases came to single [digits],” the professor of public health from the International Medical University (IMU) said.
“There was a sense of confidence (overconfidence maybe) that we can conquer this infection with ease. There was a statement made that we may not need a vaccine to conquer this infection! Such was the confidence!”
Dr Lokman Hakim Sulaiman, professor of public health at International Medical University
Collateral Damage From Seven-Week Long MCO

Although the MCO was necessary to flatten the Covid-19 epidemiological curve, there was huge collateral damage that came along with the MCO.
The government suffered a loss of almost RM300 million per day of Gross Domestic Product (GDP) earnings during the MCO. Many people also lost their jobs, suffered pay cuts, while many businesses had to shut down.
Meanwhile, non-Covid-19 patients also suffered during the MCO. Firstly, it was due to a lack of comprehensive implementation of standard operating procedures (SOPs).
Secondly, elective surgeries, cancer treatment, and follow-up scans for cancer patients were all postponed. A study conducted by University Malaya and King’s College London found that with a delay in treatment, a cancer patient’s condition may just worsen to advanced stages, by which options for treatment will be costlier and prognosis will be poorer.
Thirdly, due to roadblocks, methadone patients defaulted on their treatment because they were too afraid that they could be caught by police while encountering them at the roadblocks.
Moreover, as many people were forced to stay at home and due to the stress that they faced from the economic impact of MCO on each household, many suffered from mental health issues, which currently is being called the silent epidemic.
Bukit Aman management director Ramli Din was previously quoted saying that there was one suicide per day during the MCO period.
Third Wave Started With Sabah Election

The third wave of Malaysia’s Covid-19 epidemic started with the Sabah state election in September. A few weeks before the state election, Sabah already started reporting an increasing trend of Covid-19 cases due to the Benteng LD cluster from a prison that eventually spread to the community.
However, MOH decided that the election could still be held with strict adherence to SOPs.
September 12 was the beginning of the Sabah state election campaign, ending with polling day on September 26. Politicians travelled in and out of Sabah to campaign, and it was clearly seen through various social media posts that many of them, while campaigning, did not wear their face mask and adhere to SOP.
Not to mention, there was no mandatory Covid-19 screening done for all Sabah returnees during the campaign, despite the high number of cases reported in Sabah as compared to the rest of peninsular Malaysia.
Dr Lokman said that the large movement of politicians and supporters during the elections and immediately after the elections helped spread the infection from Sabah to elsewhere.
“Several clusters of infection appeared with direct link to this inter-state movement,” Dr Lokman said.
The mandatory screening for Covid-19 for all Sabah returnees was only implemented post-elections, which was too late because there were already cases reported in the peninsula among those who returned from Sabah.
And although screening was made compulsory after the election, there was still no mandatory 14-day quarantine implemented for Sabah returnees who only needed to self-isolate pending the results of their airport screening.
On October 20, MOH reported that 30.8 per cent (eight) of the 26 active clusters in Selangor was first detected in individuals who returned from Sabah.
Poor Planning And Management Of Third Wave
When the third wave hit Malaysia in October, the government’s public health response was poor as authorities frequently changed SOPs, practiced double standards in enforcement, failed to foresee and prevent outbreaks among migrant workers, prisoners, and detainees, and chose the harmful lockdown method over mass testing.
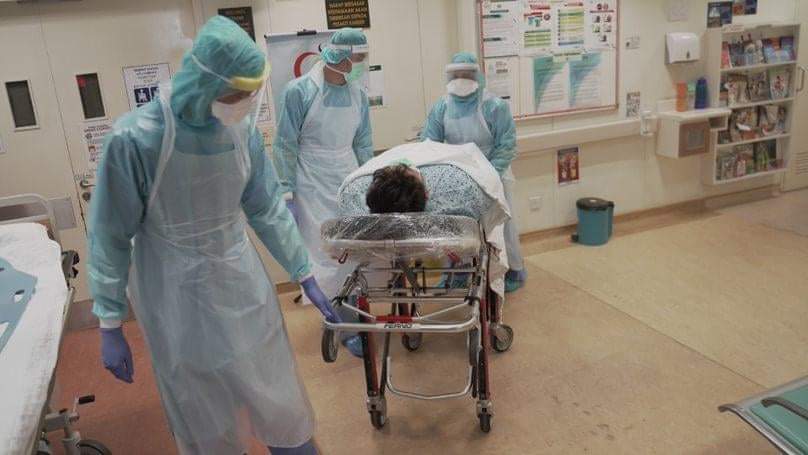
Sabah’s health care system was severely overwhelmed. Medical frontliners described the situation as Ground Zero, full beds with sick Covid-19 patients, understaffed hospitals, fatigued health care workers laboring 24/7 as their colleagues contracted Covid-19, and protective gear stocks running low.
At the same time, doctors also said that many undocumented immigrants in Sabah refused to seek early treatment for Covid-19 as they were not able to pay for their treatment, coming in only when they were really sick. This led to more outbreaks among the community.
The third wave was also when MOH reported the youngest death due to Covid-19, a one-year-old baby girl in Semporna on October 6.
After Sabah, cases started rising in the Klang Valley and despite being warned by public health experts as well as MPs, the government decided to implement a Conditional Movement Control Order (CMCO) in Klang Valley on October 14, which has now been extended till the end of the year.
However, the authorities lifted interstate travel restrictions from December 7. The CMCO, according to Muhyiddin, had cost Malaysia RM17 billion in GDP loss.
One of the weaknesses seen during the implementation of CMCO was poor communication of SOPs. For instance, when the CMCO was announced, the government said that dine-ins were not allowed and gyms would have to be closed. One day later, dining in restaurants was allowed and a week later, gyms were allowed to operate.
Secondly, there were also clear double standards that were practiced in terms of SOPs among public officials or elected lawmakers, and the general public. On one hand, the public was getting fined for not wearing a face mask, and on the other hand, politicians were seen in pictures on social media without a face mask among large groups and not getting fined for it.

Dr Lum told CodeBlue that with the passage of time, there are increasing questions about Malaysia’s future roadmap, including the differential treatment for non-compliance with SOPs, with the one rule for those in authority and another for the general public.
The physician also highlighted MOH’s refusal in sharing their data on Covid-19 cases with the Selangor Task Force For Covid-19 (STFC), unlike before, which previously helped STFC carry out their own screening for Covid-19 within the high-risk community.
“Refusal to share data on indicators, clinical data etc with doctors, Selangor government. Poor risk communication, example: non-disclosure of sites visited or residences of positive cases; delays in disclosures of positive cases in Klang, Serdang, Selayang, Ampang hospitals,” Dr Lum said.
This was seen during Covid-19 outbreaks among health care workers in several government hospitals in the Klang Valley, especially in Tengku Ampuan Rahimah Hospital (HTAR), Klang, which had gone unreported by MOH until it was highlighted by the media.
“Learn from Thailand how their community empowerment has been very successful in their Covid-19 response. They did nothing extraordinary but they empower their community from Day Zero, whereas we continue to hide where the cases are from the public.”
Dr Lokman Hakim Sulaiman, professor of public health at International Medical University
Another weakness of the public health response during the third wave was the government’s failure to engage with general practitioners (GPs) to handle non-communicable disease (NCD) patients, as well as to conduct more Covid-19 screenings within the community.
“Almost negligible engagement of general practitioners in management of Covid-19 and non-Covid-19 patients; and of non-governmental organisations assisting the vulnerable,” Dr Lum said.

The government also failed to foresee an outbreak in detention centres and migrant workers, despite having a few outbreaks in prisons previously during the second wave. This led to the outbreak of Malaysia’s largest cluster — the Teratai cluster involving migrant workers from Top Glove Corporation Bhd living in Klang, Selangor.
As of December 26, the Teratai cluster reported a whopping 6,050 cases out of 9,065 people screened, which means two-thirds out of those screened were positive for Covid-19. The cluster has spread from Selangor to Kuala Lumpur, Putrajaya, and Terengganu.
Unlike Singapore, Malaysia did not test all migrant workers nationwide during the earlier waves of the epidemic, announcing a one-time mandatory screening only from December 1, after daily Covid-19 cases surpassed 1,000 for weeks.
The Malaysian government also did not look into the poor living conditions of migrant workers months ago, when daily coronavirus infections were reported below 50 or 100, initiating investigations on overcrowded workers’ dormitories only after the explosion of the Teratai cluster.
Although the government acknowledged that prisons were running at over-capacity, many non-violent offenders have also not been freed by the Prisons Department.
Malaysia’s Covid-19 Vaccine Strategy

Minister of Science, Technology, and Innovation Khairy Jamaluddin announced last Wednesday that the government has made solid agreements with Pfizer, COVAX, and AstraZeneca to immunise 40 per cent of the population. The first batch of a million doses of the Pfizer-BioNTech vaccine is expected to be delivered to Malaysia in February 2021.
The government is also currently negotiating with Sinovac and CanSinoBIO from China, as well as with Russia, to procure an additional 42.8 per cent population coverage with Covid-19 vaccines.
Dr Lokman said that it is commendable that the government is giving free vaccines to Malaysians, but there are questions that should be answered, including the vaccination priority list, whether or not the public will get the option to choose which vaccine they want, logistics, and manpower to carry out the vaccination.
Although Malaysia is behind its neighbour Singapore, which has already received their first batch of the Pfizer vaccine, it is hoped that the government stays transparent, comes up with a clear vaccination strategy, including logistics, educates the public about getting vaccinated, and not politicise the vaccination strategy and procurement.
Singapore’s MOH said yesterday, after the government fully accepted the recommendations of Singapore’s expert committee on Covid-19 vaccination, that health care workers would be vaccinated from December 30, while elderly people would be immunised from February 2021.







