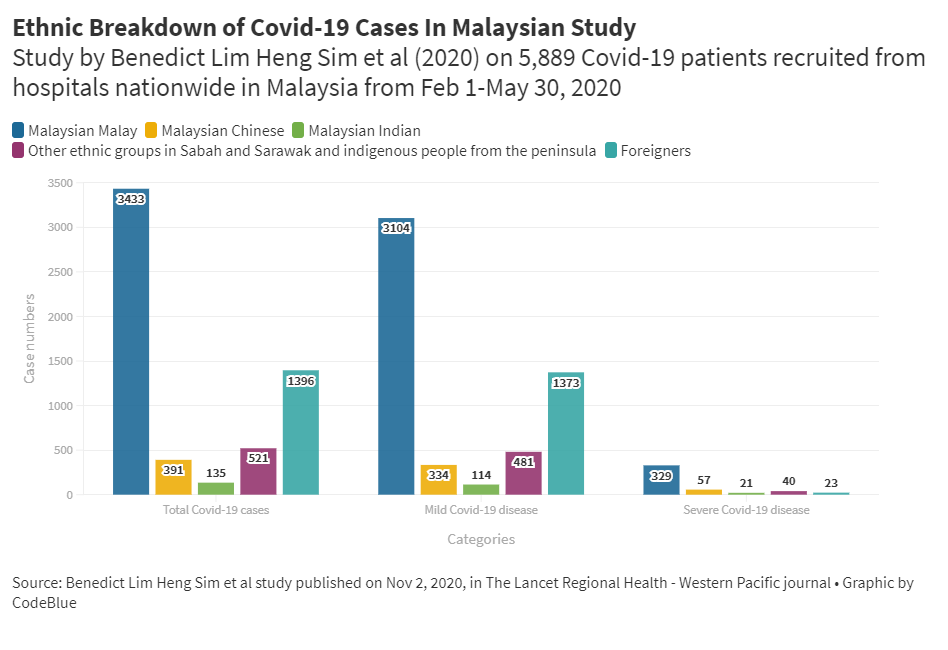
KUALA LUMPUR, Dec 7 — Unlike the United States and the United Kingdom, there were no differences in severity of Covid-19 based on gender and ethnicity in Malaysia, according to a local study.
The research by Benedict Lim Heng Sim et al, published on November 2 in The Lancet Regional Health – Western Pacific journal, cited other studies that showed health disparities in the US, with more African Americans suffering from poorer Covid-19 outcomes.
“The Malaysian public health care system is subsidised with good accessibility for both citizens and foreigners according to geographical coverage,” wrote the researchers from Sungai Buloh Hospital’s Infectious Disease Department, the Institute for Clinical Research’s Digital Health Research and Innovation Unit, and Seberang Jaya Hospital’s Clinical Research Centre.
The Malaysian research studied 5,889 Covid-19 cases who were admitted to hospitals nationwide and recruited from 18 designated Covid-19 hospitals between February 1 and May 30. Overall, 95 per cent presented with mild disease (Stages 1 to 3) on admission, and 3.5 per cent subsequently progressed to severe disease (Stages 4 and 5).
Covid-19 patients are categorised based on five clinical stages — Stage 1 is asymptomatic, Stage 2 is symptomatic without pneumonia, Stage 3 refers to pneumonia without hypoxia, Stage 4 patients have pneumonia with hypoxia; while Stage 5 patients are critically ill. Hypoxia is a condition when tissues of the body don’t receive sufficient oxygen supply.
The study reported up to 92 per cent of Covid-19 cases having mild disease, while 3.3 per cent, or 193 cases, were admitted to the intensive care unit (ICU). Fifty-one cases were admitted for at least 14 days in ICU. Almost 80 per cent of all ICU admissions occurred within the first five days of hospitalisation.
In terms of ethnic breakdown, 58.4 per cent of the 5,889 Covid-19 cases in the study were Malaysian Malay, followed by non-nationals (23.8 per cent), other ethnic groups in Sabah and Sarawak and indigenous people from the peninsula (8.9 per cent), Malaysian Chinese (6.7 per cent), and Malaysian Indian (2.3 per cent).
The local study showed that of the 471 severe Covid-19 cases, which comprised about 8 per cent of total participants, the proportion of men was mostly the same, at 71.5 per cent, as the male share in the mild disease group at 71.7 per cent.
However, the ethnic composition for Malays, Chinese, and Indians were higher in the severe disease category (70 per cent, 12.1 per cent, and 4.5 per cent respectively), compared to their share in the mild disease group (57.4 per cent, 6.2 per cent, and 2.1 per cent respectively).
Other Malaysian ethnic groups comprised 8.5 per cent of the severe disease category, slightly lower than their 8.9 per cent share in the mild group. Foreigners only comprised 4.9 per cent of severe Covid-19 cases, far smaller than their 25.4 per cent share of mild cases.
Majority of Malaysians and non-nationals with Covid-19 experienced mild disease. Most foreigners, or 98.3 per cent, had mild Covid-19 disease, followed by other Malaysian ethnic groups (92.3 per cent), Malays (90.4 per cent), Chinese (85.4 per cent), and Indians (84.4 per cent).
Researchers said their Malaysian study, titled “Clinical characteristics and risk factors for severe Covid-19 infections in Malaysia: A nationwide observational study” was the first national study in Southeast Asia for all lab-confirmed Covid-19 cases “representing a whole country’s experience with definite outcome showing low mortality”.
Compared to other countries like China, South Korea, Singapore, and US city New York that reported older Covid-19 patients aged between 40 and 63 years, the Malaysian study had a much younger group of patients with a median age of 34, while 72 per cent were male. (Cases aged below 12 years were excluded from the Malaysian research).
Local researchers attributed the skewed age distribution to a possible cluster effect from the three-day Muslim religious tabligh gathering in Kuala Lumpur in early March with more younger and male participants.
“As asymptomatic transmission and pre-symptomatic transmission of SARS-CoV-2 happens, clustering effects among young males can contribute to a higher transmission rate.
“In addition, effective contact tracing, early confinement and stringent social distancing limited the spread of disease from younger, mobile population to the elderly, as compared to overseas study.”
For all severe cases, around 40 per cent were admitted into ICU, with 29 per cent requiring invasive ventilation. Median hospitalisation for severe Covid-19 cases was 14 days.
The local study showed a low Covid-19 case fatality rate (CFR) of 1.2 per cent (73 in-hospital deaths, of which all except one occurred in those with severe disease), compared to other coronavirus epidemics like SARS (9.5 per cent) and MERS (34.4 per cent). Researchers noted that Covid-19 presentation was milder despite high virological similarity with SARS, causing higher transmissibility than the other two viruses.
“This could lead to underestimation of CFR due to underreporting of the asymptomatic infected population in the community,” said researchers, who also attributed Malaysia’s lower case fatality rate possibly to young cases with mild Covid-19 disease and early hospitalisation.
“Early hospitalisation leads to enforced separation from the greater community, especially those in vulnerable groups. In Malaysia, the strategy of hospital isolation of all suspected and confirmed individuals contributed to the reduction of local transmission. Our approach was similar to countries demonstrated lower CFR such as Singapore (0.05 per cent) and Republic of Korea (2.10 per cent) where ‘trace, test and treat’ was practised.”
More than half of the severe Covid-19 cases in the Malaysian study were aged 51 years and above. Besides older age, underlying chronic kidney disease and chronic pulmonary disease, fever, cough, diarrhoea, breathlessness, tachypnoea (abnormally rapid breathing), abnormal chest radiographs, and higher C-reactive protein (CRP) levels in the blood on admission were significant determinants for Covid-19 severity.
About 6 per cent of Covid-19 patients in the Malaysian study were health care workers. The Malaysian study had 71 pregnant women infected with coronavirus, including six with severe Covid-19 disease, of which two required intensive care.
Less than two-thirds, or 62.7 per cent, of participants had a history of contact with a confirmed Covid-19 case within the past 14 days of diagnosis and/ or symptom onset. The median of illness onset to admission was three days, while those with severe Covid-19 were admitted on Day 6.
About 70 per cent of participants did not have fever upon admission. Only a quarter of Covid-19 cases with mild disease reported fever as compared to three-quarters of those with severe disease. The pattern was similar for cough.